The document discusses euthanasia and provides information on its history, types, laws, and religious views.
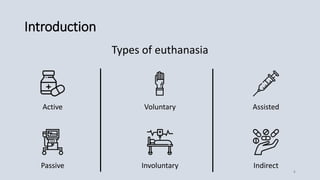
[1] Euthanasia refers to intentionally ending a life to relieve pain and suffering, and can be active, passive, voluntary, or involuntary. It was first discussed in ancient Greece but largely rejected throughout history.
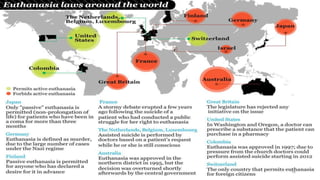
[2] Currently, only the Netherlands and Belgium legally permit euthanasia under certain conditions like voluntary requests and consultation. Assisted suicide is legal in some places with restrictions.
[3] Most major religions disapprove of euthanasia due to beliefs that God gives and takes life, though some accept passive forms or withholding treatment. Views vary between faith