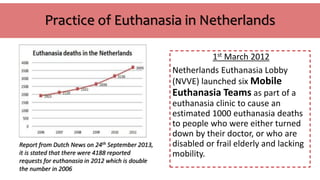
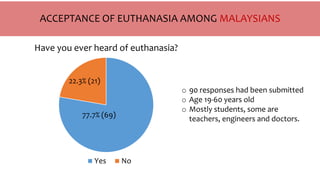
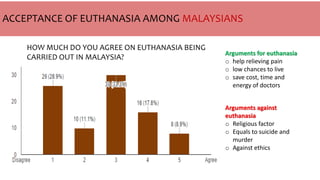
The document provides an overview of euthanasia, including its definition, types, and legal status in various countries, such as Canada, the Netherlands, Australia, and Japan. It discusses public perceptions and moral arguments for and against euthanasia, particularly referencing Islamic perspectives that oppose the practice. The document highlights the evolving legal landscape surrounding euthanasia and varying cultural attitudes towards it.