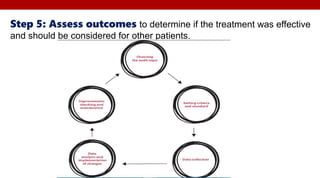
This document discusses evidence-based practice (EBP) in nursing and healthcare. It defines EBP as using research-based evidence to guide holistic patient care. The benefits of EBP include improved patient outcomes, reduced costs, and enhanced nursing practice. EBP involves five steps: asking a clear clinical question, acquiring evidence, appraising the evidence, applying the evidence to practice, and assessing outcomes. Barriers to EBP include lack of time, resources, and skills to implement research into practice. Overall, the document emphasizes that properly applying EBP through all five steps can help strengthen nursing practice and improve patient care.
![EVIDENCE BASED PRACTICE [EBP]
IN NURSING/MEDICAL CARE](https://image.slidesharecdn.com/group4-240202075534-4be5f139/75/EBP-pptx-1-2048.jpg)