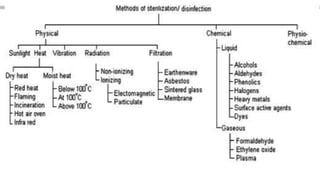
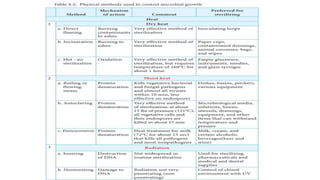
This document discusses various methods for decontamination, sterilization, and disinfection important for laboratory biosafety. It defines key terms like sterilization, which aims to eliminate all microbial life, versus disinfection, which aims to eliminate pathogens but not bacterial spores. Various physical methods for sterilization are covered, including heat/thermal methods like autoclaving, radiation methods, and filtration. Specific sterilization techniques using heat, chemicals, and gases are then described in more detail. The document emphasizes the importance of choosing the appropriate sterilization or disinfection method based on the level and type of contamination present.