The document discusses cancer and India's National Cancer Control Program. It provides details on:
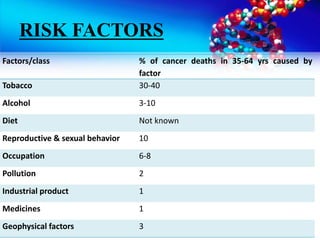
- Cancer burden and risk factors in India such as tobacco use and diet
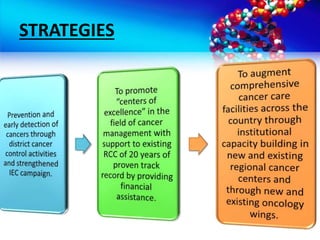
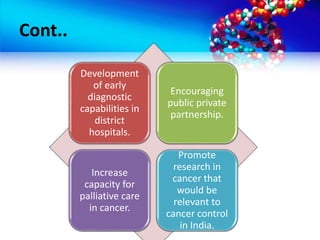
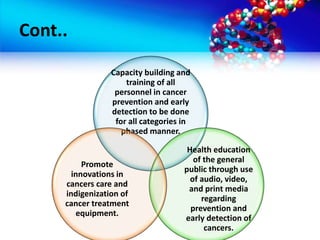
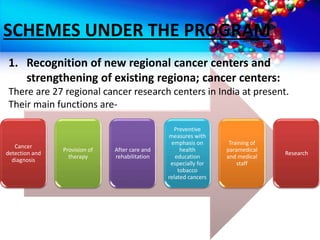
- Objectives and strategies of the National Cancer Control Program to address prevention, early detection, treatment and palliative care
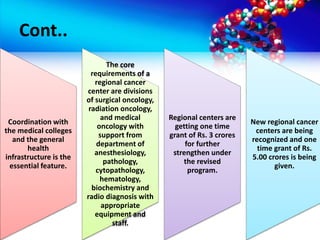
- Implementation of the program through various schemes targeting medical colleges, districts, NGOs and voluntary organizations
- Perceptions of surgical oncologists that oncology education in India can be improved during medical school, residency and for practicing physicians