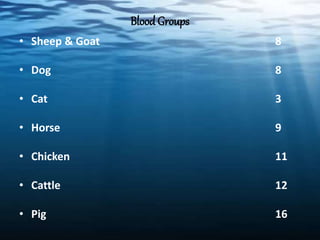
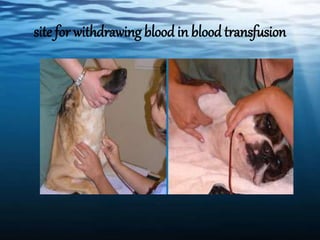
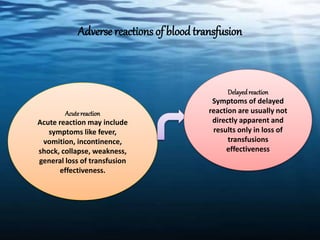
The document discusses blood transfusion in animals, including definitions, indications for transfusion, blood typing of different species, donor selection criteria, blood collection and storage methods, cross-matching to ensure compatibility, administration procedures, potential adverse reactions and treatments, and uses of blood products like plasma, packed red cells, and platelets. Proper donor screening, cross-matching, warming, and slow infusion are important to avoid transfusion reactions in animals.