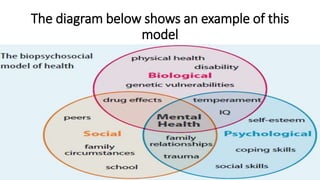
The document discusses the biopsychosocial model proposed by George Engel, emphasizing the importance of biological, psychological, and social factors in understanding medical conditions. It highlights how these components can influence each other, particularly in cases of chronic pain, and the relevance for physiotherapists in designing intervention programs. Furthermore, it covers the types of pain and the need for comprehensive assessments to address individual patient experiences.