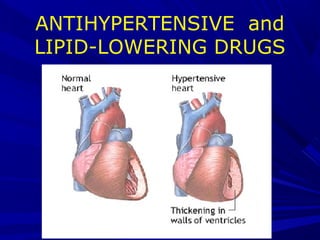
Antihypertensive and Lipid Lowering Drugs
- 2. 22
- 3. 33 ANTIHYPERTENSIVE DRUGS:ANTIHYPERTENSIVE DRUGS: I. DIURETICSI. DIURETICS:: HydrochlorthiazideHydrochlorthiazide ((DichlothiazideDichlothiazide)) –– Tab. 0.025 and 0.1 gTab. 0.025 and 0.1 g FurosemideFurosemide ((LasixLasix)) – Tab. 0.04 g ; amp 1%-2 ml– Tab. 0.04 g ; amp 1%-2 ml BumetanideBumetanide ((BurinexeBurinexe)) –– Tab. 0.001 g; amp 0.025% - 2 mlTab. 0.001 g; amp 0.025% - 2 ml IndapamideIndapamide – Tab. 2.5 mg (0.0025 g)– Tab. 2.5 mg (0.0025 g) VerospironeVerospirone ((SpironolactoneSpironolactone)) – Tab. 25 mg– Tab. 25 mg AmilorideAmiloride – Tab. 2.5 and 5 mg– Tab. 2.5 and 5 mg TriamterenTriamteren – Caps. 50 mg (0.05 g)– Caps. 50 mg (0.05 g)
- 4. 44 HydrochlorthiazideHydrochlorthiazide ((DichlothiazideDichlothiazide)) Na+Na+ andand Water ExcretionWater Excretion =>=> Extracellular VolumeExtracellular Volume =>=> Cardiac OutputCardiac Output andand Renal Blood FlowerRenal Blood Flower Electrolyte disturbanceElectrolyte disturbance:: K+ ,K+ , Mg2+,Mg2+, Ca2+Ca2+ Thiazide diureticsThiazide diuretics counteract the Nacounteract the Na++ andand water retention observed with other agents usedwater retention observed with other agents used in the treatment of hypertension.in the treatment of hypertension. Thiazide diureticsThiazide diuretics are useful in combination therapy withare useful in combination therapy with a variety of other antihypertensive drugs includinga variety of other antihypertensive drugs including β-blockersβ-blockers andand ACE inhibitorsACE inhibitors.. Adverse effectsAdverse effects:: Hypokalemia and Hyperuricemia –Hypokalemia and Hyperuricemia – in 70% of patients,in 70% of patients, Hyperglycemia -Hyperglycemia - in 10% of patientsin 10% of patients
- 5. 55 II. Sympathoplegic AgentsII. Sympathoplegic Agents:: 1. Centrally-acting Adrenergic Drugs1. Centrally-acting Adrenergic Drugs:: αα22 AdrenomimeticsAdrenomimetics:: Clopheline (Clopheline (ClonidineClonidine) -) - Tab. 0.000 075 and 0.00015 gTab. 0.000 075 and 0.00015 g ampamp.. 0.01% - 1 ml0.01% - 1 ml MethyldopaMethyldopa TabTab.. 0.25 g0.25 g GuanfacineGuanfacine TabTab.. 0.0005, 0.001 and 0.002 g0.0005, 0.001 and 0.002 g MoxonidineMoxonidine Tab. 0.0002 and 0.0004 gTab. 0.0002 and 0.0004 g
- 6. 66
- 7. 77 Clopheline (Clonedine)Clopheline (Clonedine) –– CentralCentral AAdrenergicdrenergic Outflow.Outflow. To treat mild to moderate hypertension thatTo treat mild to moderate hypertension that has not responded adequately to the treatment withhas not responded adequately to the treatment with diuretics alone.diuretics alone. After IV injection, ClophelineAfter IV injection, Clopheline →→ a briefa brief BPBP followedfollowed by more prolonged hypotension.by more prolonged hypotension. The pressor response is due to direct stimulation ofThe pressor response is due to direct stimulation of presynaptic αpresynaptic α22 adrenoreceptors in arterioles.adrenoreceptors in arterioles.
- 8. 88 2. Centrally and Peripherally Acting Drugs2. Centrally and Peripherally Acting Drugs:: a)a) Sympatholytics:Sympatholytics: Reserpine – Tab. 0.1 mg and 0.25 mgReserpine – Tab. 0.1 mg and 0.25 mg Octadine (Guanethidine) – Tab. 0.025 g (25 mg)Octadine (Guanethidine) – Tab. 0.025 g (25 mg) b)b) Ganglioblockers:Ganglioblockers: Benzohexonium – Tab, 0.1 and 0.25 g, Amp. 2.5% - 1 mlBenzohexonium – Tab, 0.1 and 0.25 g, Amp. 2.5% - 1 ml Pentamine – amp. 5% - 1 mlPentamine – amp. 5% - 1 ml c)c) β-Blockers:β-Blockers: Propranolol (Anaprilin) – Tab. 10 and 40 mg; Amp. 0.1%-1 mlPropranolol (Anaprilin) – Tab. 10 and 40 mg; Amp. 0.1%-1 ml Atenolol –Tab. 50 and 100 mgAtenolol –Tab. 50 and 100 mg Metoprolol – Tab. 50 and 100 mgMetoprolol – Tab. 50 and 100 mg d)d) α – Blockers:α – Blockers: Phentolamine – Tab. 0.025 (25 mg)Phentolamine – Tab. 0.025 (25 mg) Tropaphen – (amp. 20 mg)Tropaphen – (amp. 20 mg)
- 9. 99
- 10. 1010 RESERPINERESERPINE blocks theblocks the MgMg 2+2+ / ATP/ ATP – dependent transport of– dependent transport of aminesamines -- NoradrenalineNoradrenaline ,, DopamineDopamine andand SerotoninSerotonin from the cytoplasm intofrom the cytoplasm into storage vesiclesstorage vesicles in the adrenergic nerves of all body tissuesin the adrenergic nerves of all body tissues ⇒depletion ofdepletion of noradrenalinenoradrenaline levelslevels in the adrenergic neuron, sincein the adrenergic neuron, since MAOMAO degrades thedegrades the NoradrenalineNoradrenaline (NA)(NA) ⇒Sympathetic functionSympathetic function is impaired because ofis impaired because of Release of NARelease of NA ReserpineReserpine Blood PressureBlood Pressure by a combination of :by a combination of : Cardiac Output andCardiac Output and Peripheral Vascular ResistancePeripheral Vascular Resistance Adverse effect:Adverse effect: Sedation, Lassitude, Nightmares, Mental Depression,Sedation, Lassitude, Nightmares, Mental Depression, Extrapyramidal Effects resembling Parkinson's diseaseExtrapyramidal Effects resembling Parkinson's disease as a result ofas a result of dopamine depletiondopamine depletion in thein the corpus striatumcorpus striatum GIT abnormalitiesGIT abnormalities - diarrhea, gastrointestinal cramps,- diarrhea, gastrointestinal cramps, increase of gastric acid secretion, ulcerincrease of gastric acid secretion, ulcer
- 11. 1111
- 12. 1212 PropranololPropranolol - a β-adrenoblocker, is useful for- a β-adrenoblocker, is useful for BPBP inin mild to moderatemild to moderate hypertensionhypertension InIn Severe HypertensionSevere Hypertension, it is especially useful in preventing the, it is especially useful in preventing the reflex tachycardia that results from treatment with directreflex tachycardia that results from treatment with direct vasodilatorsvasodilators PropranololPropranolol BP by:BP by: Cardiac OutputCardiac Output Sympathetic outflow from the CNSSympathetic outflow from the CNS Renin ReleaseRenin Release andand Renin-Angiotensin-Aldosteron systemRenin-Angiotensin-Aldosteron system Adverse effectAdverse effect:: Bradycardia, Bronchospasm, CHF,Bradycardia, Bronchospasm, CHF, Vasoconstriction, Cold Extremities,Vasoconstriction, Cold Extremities, Intermittent Claudication, Fatigue, Lethargy,Intermittent Claudication, Fatigue, Lethargy, Mental Depression, Memory Loss, Hallucination, ImpotenceMental Depression, Memory Loss, Hallucination, Impotence CholesterolCholesterol TriglyceridesTriglycerides HDL-cholesterolHDL-cholesterol
- 13. 1313 III. PERIPHERAL VASODILATORSIII. PERIPHERAL VASODILATORS:: 1. Direct Vasodilators: Apressine (Hydralasine) – Tab. 0.01 and 0.025 g MgSO4 – amp. 25% – 10 ml IM Dibazole (Bendazole) – amp. 1% - 1 and 5 ml, Tab. 2 and 4 mg No-spa - (Drotaverine) – amp. 2%-2 ml, Tab. 0.04 g Papaverine hydrochloride – amp. 2%-2 ml, Tab. 0.04 g Nanipruss (Na+ Nitroprusside) – amp. 25 and 50 mg Euphylline (Aminophylline) – Tab. 0.15 g, amp. 2.4% - 10 ml, 24% - 1 ml
- 14. 1414 2. Calcium Channel Blockers – block high-threshold Ca2+ channels of L-type A. Diphenylalkylamines: VerapamilVerapamil ((IsoptinIsoptin)) – Tab. 40, 80 mg– Tab. 40, 80 mg B. Dihydropyridines: 1st Generation: Nifedipine (Adalat, Procardia) – Tab. 10 and– Tab. 10 and 2nd Generation: Amlodipine ((NorvascNorvasc)) –– Tab. 2.5, 5, and 10 mgTab. 2.5, 5, and 10 mg Isradipine – Caps. 2.5 and 5 mg– Caps. 2.5 and 5 mg Nicardipine C. Benzothiazepines: Diltiazem – Tab. 30, 60, 120 mg– Tab. 30, 60, 120 mg
- 15. 1515 3.3. αα11 – Blockers: -– Blockers: - PrazosinPrazosin – Tab. 1, 3, 5 mg– Tab. 1, 3, 5 mg DoxazosinDoxazosin – Tab. 2 and 4 mg– Tab. 2 and 4 mg TerazosinTerazosin – Tab. 2 and 5 mg– Tab. 2 and 5 mg 4. K4. K++ Channel ActivatorChannel Activator:: DiazoxideDiazoxide –– amp. 1.5% - 20 ml IV infusionamp. 1.5% - 20 ml IV infusion MinoxidilMinoxidil –– Tab. 5 mgTab. 5 mg Vial - 2%-10 ml IV infusionVial - 2%-10 ml IV infusion
- 16. Ca2+ CCa2+ Channelhannel BBlockerslockers are useful inare useful in thethe TTreatment ofreatment of PPatientsatients with:with: AsthmaAsthma DiabetesDiabetes Peripheral Vascular DiseasePeripheral Vascular Diseasess
- 17. 1717 VerapamilVerapamil :: AntianginalAntianginal AntihypertensiveAntihypertensive Antiarrhythmic actionsAntiarrhythmic actions AfterloadAfterload =>=> O2 consumption HR: itHR: it slows Cardiac Conduction directlyslows Cardiac Conduction directly Coronary Artery and Peripheral VesselsCoronary Artery and Peripheral Vessels VasodilationVasodilation Prinzmetal’s Variant Angina:Prinzmetal’s Variant Angina: it Inhibits Coronary Artery Spasm =>it Inhibits Coronary Artery Spasm => =>=> MYOCARDIAL OMYOCARDIAL O22 DELIVERYDELIVERY Adverse EffectsAdverse Effects:: Myocardial Depression, Including CardiacMyocardial Depression, Including Cardiac Arrest, Bradycardia, AV Block, Heart Failure,Arrest, Bradycardia, AV Block, Heart Failure, Constipation, Peripheral Edema.Constipation, Peripheral Edema.
- 18. 1818 NifedipineNifedipine –– is anis an Arteriolar Vasodilator.Arteriolar Vasodilator. It dilates Systemic Arteries, resulting in:It dilates Systemic Arteries, resulting in: Total Peripheral ResistanceTotal Peripheral Resistance ((TPRTPR)) SystemicSystemic BPBP with slightlywith slightly HRHR AfterloadAfterload andand Cardiac IndexCardiac Index The vasodilation effect is useful in the treatment ofThe vasodilation effect is useful in the treatment of Prinzmetal’sPrinzmetal’s VARIANT ANGINAVARIANT ANGINA Adverse effectsAdverse effects:: Flushing, Headache, Tachycardia,Flushing, Headache, Tachycardia, Dizziness, Nausea, Constipation,Dizziness, Nausea, Constipation, Peripheral EdemaPeripheral Edema due to itsdue to its Vasodilation ActivityVasodilation Activity
- 19. 1919 AmlodipineAmlodipine is ais a dihydropyridinedihydropyridine compound –compound – the 2the 2ndnd generation long-acting Cageneration long-acting Ca2+2+ antagonistantagonist It blocks the inward movement of CaIt blocks the inward movement of Ca2+2+ by binding toby binding to L-typeL-type CaCa2+2+ channelschannels in the heart and in smooth muscle of thein the heart and in smooth muscle of the coronary and peripheral vasculaturecoronary and peripheral vasculature Dilating MainlyDilating Mainly ARTERIOLESARTERIOLES The drug has anThe drug has an Intrinsic Natriuretic EffectIntrinsic Natriuretic Effect Antianginal,Antianginal, Hypotensive, VasodilativeHypotensive, Vasodilative andand Spasmolytic actionSpasmolytic action Clinical Use:Clinical Use: Arterial HypertensionArterial Hypertension Stable and Unstable anginaStable and Unstable angina Prinzmetal’s or Variant Angina PectorisPrinzmetal’s or Variant Angina Pectoris Peak effects occur within 1-2 hours and persist forPeak effects occur within 1-2 hours and persist for 24 hours24 hours Adverse effectsAdverse effects:: Headache, Peripheral EdemaHeadache, Peripheral Edema
- 20. 2020 MinoxidilMinoxidil –– Tab. 5 mg, vial - 2%-10 ml –Tab. 5 mg, vial - 2%-10 ml – KK++ Channel Activator.Channel Activator. The effect results fromThe effect results from the opening of Kthe opening of K++ channelschannels in smooth muscle membranesin smooth muscle membranes This action stabilizes the membrane at itsThis action stabilizes the membrane at its Resting PotentialResting Potential andand makes contraction less likely.makes contraction less likely. LikeLike HydralazineHydralazine,, Minoxidil dilates Arterioles but not VeinsMinoxidil dilates Arterioles but not Veins.. MinoxidilMinoxidil is well absorbed from the GIT and is metabolized,is well absorbed from the GIT and is metabolized, primarily by conjugation, in the liver.primarily by conjugation, in the liver. Clinical useClinical use:: treatment of severe to malignant hypertensiontreatment of severe to malignant hypertension that is refractory to other drugs.that is refractory to other drugs. Reflex tachycardiaReflex tachycardia may be severe and may require themay be severe and may require the concomitant use of aconcomitant use of a β-blocker.β-blocker. Adverse effectsAdverse effects:: seriousserious NaNa++ andand water retentionwater retention, leading to, leading to volume overload, edema, and CHF.volume overload, edema, and CHF. HYPERTRICHOSISHYPERTRICHOSIS –– the Growth of Body Hairthe Growth of Body Hair MinoxidilMinoxidil is used topically to treatis used topically to treat Male Pattern BALDNESSMale Pattern BALDNESS
- 21. 2121 IV. Agents affecting Renin-Angiotensin SystemIV. Agents affecting Renin-Angiotensin System:: 1).1). ACE Inhibitors:ACE Inhibitors: CaptoprilCaptopril – Tab. 25 and 50 mg– Tab. 25 and 50 mg EnalaprilEnalapril – Tab. 5; 10 and 20 mg– Tab. 5; 10 and 20 mg LisinoprilLisinopril – Tab. 10; 20 and 40 mg– Tab. 10; 20 and 40 mg 2)2) Angiotensine II AntagonistsAngiotensine II Antagonists:: LosartanLosartan ((CozaarCozaar) – Tab. 50 mg) – Tab. 50 mg ValsartanValsartan – Tab. 80 mg– Tab. 80 mg
- 22. 2222
- 23. 2323 Angiotensin-Converting Enzyme (ACE) inhibitorsAngiotensin-Converting Enzyme (ACE) inhibitors –– CCaptoprilaptopril EnalaprilEnalapril LisinoprilLisinopril block theblock the ACEACE that cleavesthat cleaves Angiotensin IAngiotensin I =>=> Angiotensin IIAngiotensin II ACEIACEI =>=> Bradykinin InactivationBradykinin Inactivation Adverse effectsAdverse effects:: Dry Cough, Rashes, Fever, Angioedema,Dry Cough, Rashes, Fever, Angioedema, Altered Taste, Hypotension,Altered Taste, Hypotension, HYPERKALEMIA.HYPERKALEMIA. K+ levelsK+ levels must be monitored, andmust be monitored, and K+ supplementsK+ supplements oror K+ sparing diuretis such asK+ sparing diuretis such as SSpironolactonepironolactone are contraindicatedare contraindicated!!!!!! ACEIACEI areare FetotoxicFetotoxic andand should not be usedshould not be used inin Pregnant WomenPregnant Women !!
- 24. 2424 LIPID-LOWERING DRUGSLIPID-LOWERING DRUGS 1. Hydroxy-Methyl-Glutaryl-CoA Reductase1. Hydroxy-Methyl-Glutaryl-CoA Reductase (HMG-CoA reductase)(HMG-CoA reductase) InhibitorsInhibitors:: LovastatinLovastatin – tab. 20 and 40 mg– tab. 20 and 40 mg PravastatinPravastatin – tab. 10 and 20 mg– tab. 10 and 20 mg SimvastatinSimvastatin – tab. 20 and 40 mg– tab. 20 and 40 mg FluvastatinFluvastatin - tab. 20 and 40 mg- tab. 20 and 40 mg AtorvastatinAtorvastatin 2. Fibrates2. Fibrates:: ССlofibratelofibrate – caps. 0.25 g– caps. 0.25 g FenofibrateFenofibrate GemfibrozilGemfibrozil – caps. 0.3 g, tab. 0.6 g– caps. 0.3 g, tab. 0.6 g
- 25. 2525 3). Group of Nicotinic Acid3). Group of Nicotinic Acid :: Nicotinic acid (Nicotinic acid (NiacinNiacin)) Tab. 0.05 gTab. 0.05 g;; 0.1 g and 0.5 g;0.1 g and 0.5 g; amp. 10% - 1 mlamp. 10% - 1 ml NicotinamidNicotinamid Tab.Tab. 50 mg, amp 1% - 1 ml50 mg, amp 1% - 1 ml Xantinol nicotinate (Complamin)Xantinol nicotinate (Complamin) 4). Bile Acid Binding Resinse4). Bile Acid Binding Resinse:: CholestyramineCholestyramine – pulv. 16.0-18.0 g PO– pulv. 16.0-18.0 g PO ColestipolColestipol – pulv. 5.0-10.0 g PO– pulv. 5.0-10.0 g PO 5). Antioxidants:5). Antioxidants: ProbucolProbucol – Tab. 0.5 g– Tab. 0.5 g 6). The others:6). The others: Lipostabil, PentoxiphyllineLipostabil, Pentoxiphylline
- 26. 2626 Hydroxy-methylglutaryl-CoA reductase inhibitorsHydroxy-methylglutaryl-CoA reductase inhibitors ((StatinsStatins ):): Lovastatin, Simvastatin, PravastatinLovastatin, Simvastatin, Pravastatin Fluvastatin,Fluvastatin, andand AtorvastatinAtorvastatin –– inhibit the 1inhibit the 1stst enzymatic step ofenzymatic step of STEROL SYNTHESISSTEROL SYNTHESIS -- as structural analogs of the natural substrate,as structural analogs of the natural substrate, 3-hydroxy-3-methylglutaric acid3-hydroxy-3-methylglutaric acid (HMG),(HMG), they compete to block hydroxymethylglutaryl-CoAthey compete to block hydroxymethylglutaryl-CoA reductase (HMG-CoA reductase).reductase (HMG-CoA reductase). Adverse effectsAdverse effects:: Liver Failure, MyopathyLiver Failure, Myopathy andand RhabdomyolysisRhabdomyolysis (disintegration and purulent melting(disintegration and purulent melting of skeletal muscles).of skeletal muscles).
- 27. 2727 FibratesFibrates ClofibrateClofibrate,, FenofibrateFenofibrate andand GemfibrozilGemfibrozil areare derivatives of fibric acid and are similar toderivatives of fibric acid and are similar to Endogenous Fatty Acids.Endogenous Fatty Acids. MECHANISM OF ACTIONMECHANISM OF ACTION.. the activitythe activity ofof Lipoprotein LipaseLipoprotein Lipase, hydrolyzing, hydrolyzing triglyceridestriglycerides inin chylomicronschylomicrons andand VLDLVLDL =>=> =>=> the removal of these particles from the plasma.the removal of these particles from the plasma. In contrast,In contrast, HDL levelsHDL levels moderately.moderately. Adverse EffectsAdverse Effects:: LithiasisLithiasis:: because these drugsbecause these drugs Biliary CholesterolBiliary Cholesterol excretion, there is a predisposition toexcretion, there is a predisposition to the formation ofthe formation of gallstonesgallstones MalignancyMalignancy:: Treatment withTreatment with ClofibrateClofibrate has resulted inhas resulted in a significant number of malignancy-related deathsa significant number of malignancy-related deaths MyositisMyositis
- 28. 2828 Nicotinic acidNicotinic acid -- inhibitsinhibits lipolysislipolysis inin adipose tissueadipose tissue –– the producer of circulatingthe producer of circulating Free Fatty AcidsFree Fatty Acids ⇒Eliminates the building blocks needed by the liverEliminates the building blocks needed by the liver to produceto produce triglyceridestriglycerides andand VLDLVLDL .. Adverse effectsAdverse effects. P. Pruritus, gastric irritation,ruritus, gastric irritation, hyperglycemia, hyperuricemia, elevated hepatichyperglycemia, hyperuricemia, elevated hepatic aminotransferase enzymes, and hepatitis.aminotransferase enzymes, and hepatitis. Food sources of nicotinic acid, such as avocadoes and bananas, pose no health dangers.
- 29. 2929 CholestyramineCholestyramine andand CholestipolCholestipol areare Anion Exchange ResinsAnion Exchange Resins that bindthat bind Negatively Charged Bile Acid and Bile SaltsNegatively Charged Bile Acid and Bile Salts in the small intestinein the small intestine =>=> =>=> thethe BILE ACIDSBILE ACIDS are excreted in faeces andare excreted in faeces and are not recirculated to the liver.are not recirculated to the liver. Adverse effectsAdverse effects:: Abdominal FullnessAbdominal Fullness FlatulenceFlatulence ConstipationConstipation
- 30. 3030 THANK YOU FORTHANK YOU FOR ATTENTIONATTENTION
