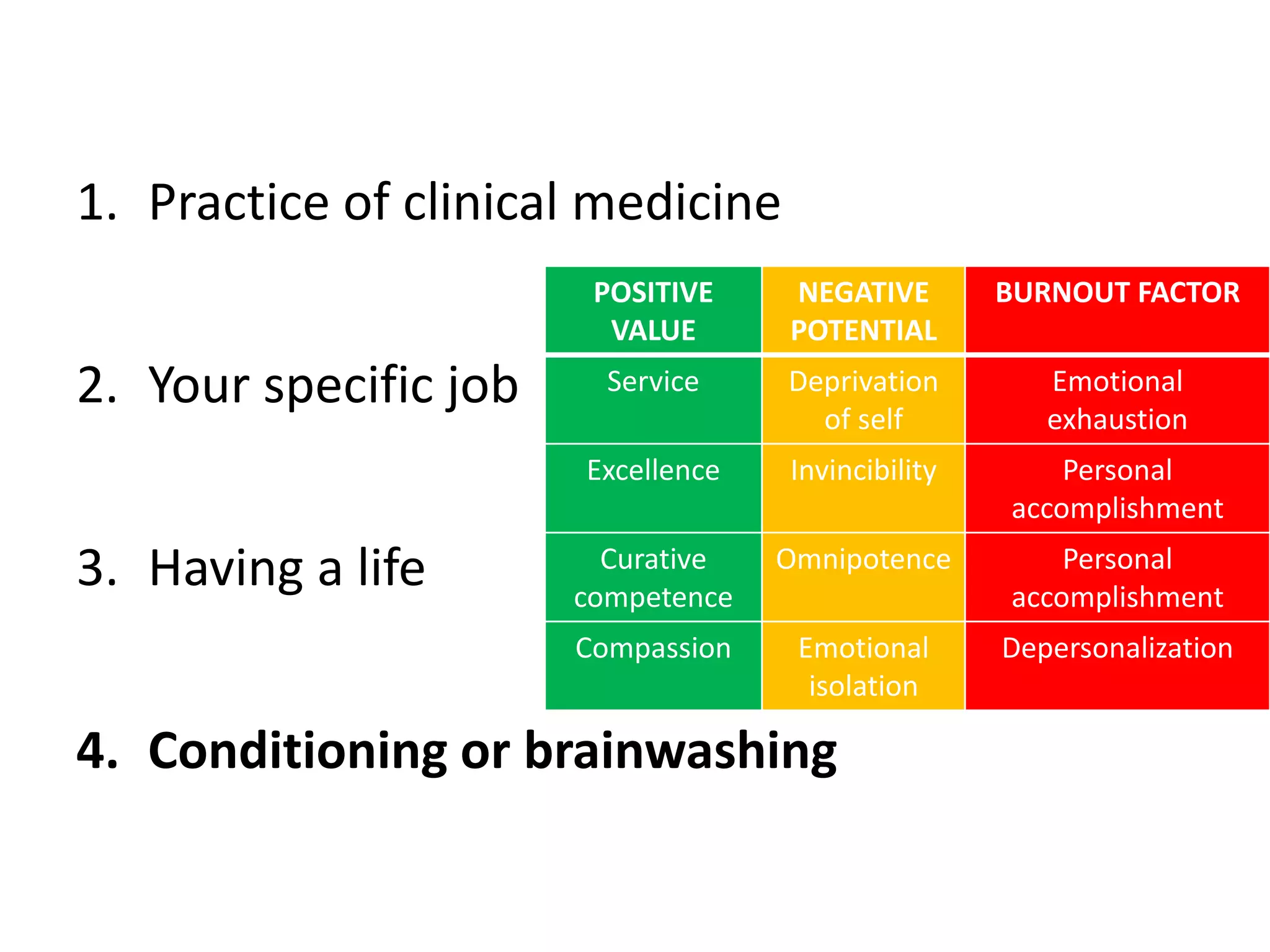
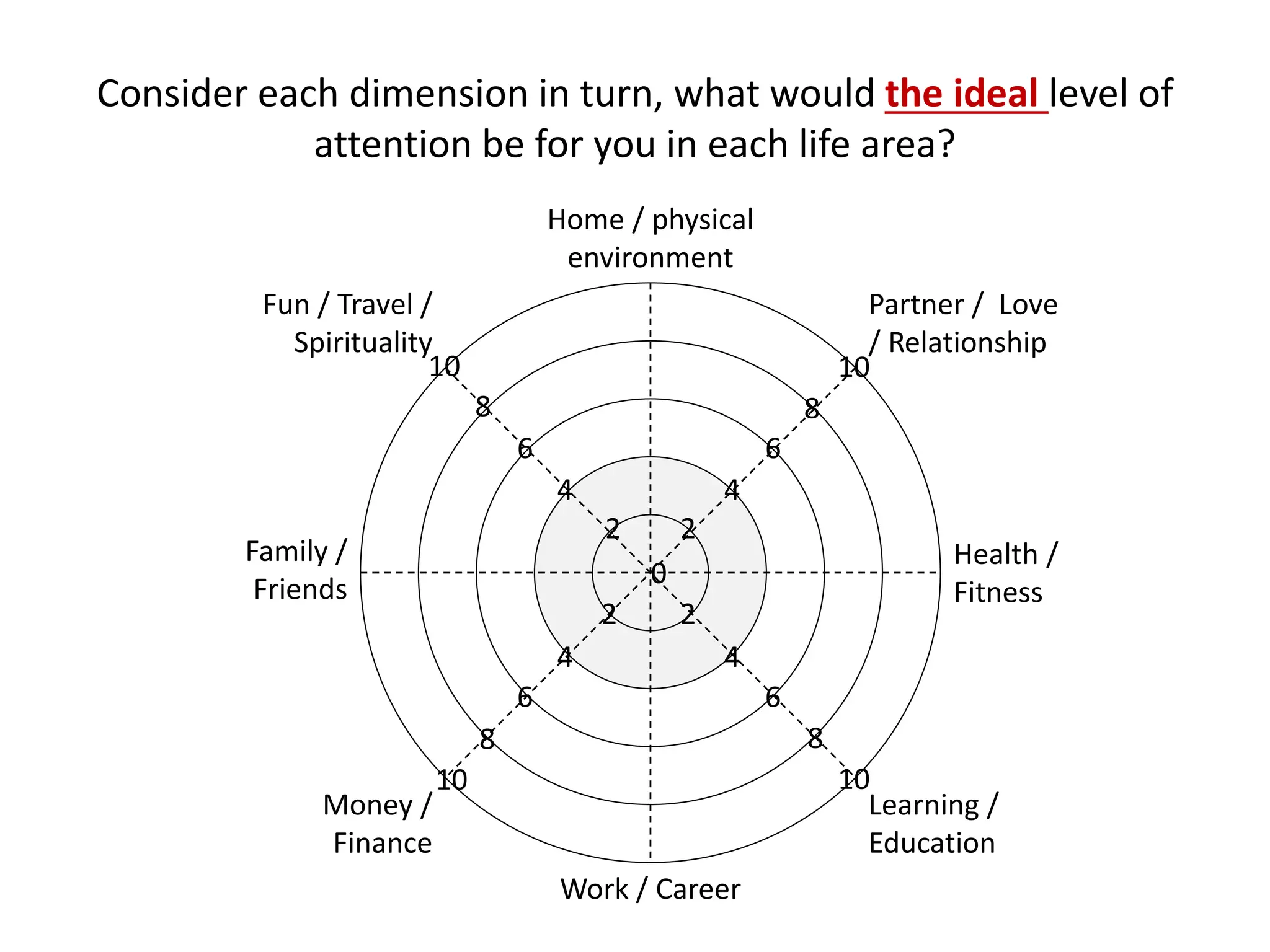
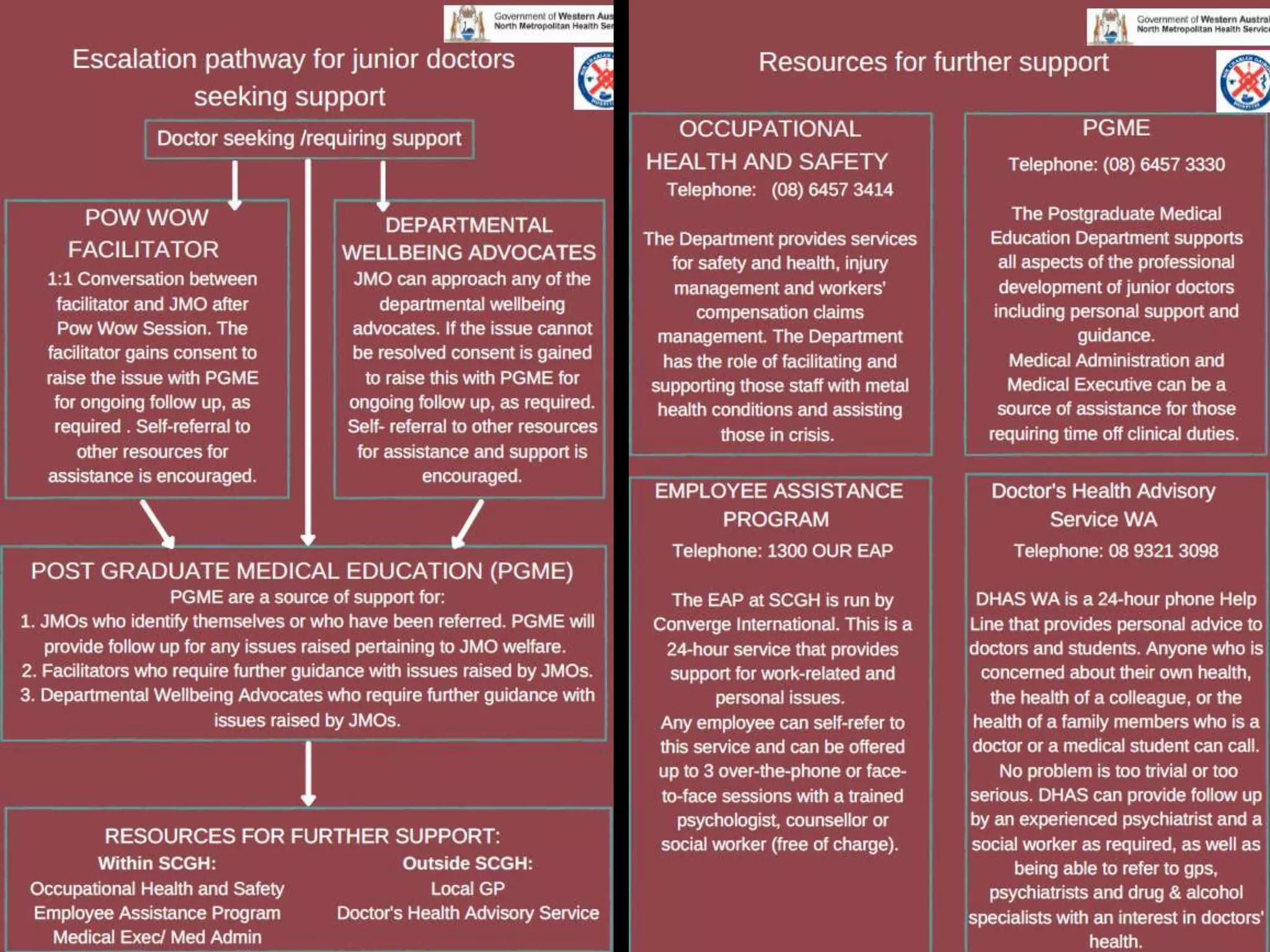
Burnout is a state of physical, emotional and mental exhaustion caused by prolonged stress and a lack of work-life balance. It is characterized by feelings of exhaustion, depersonalization, and a reduced sense of personal accomplishment. Burnout can lead to medical errors, reduced career satisfaction and longevity, physical and mental illness, and substance abuse. While there is overlap with depression, burnout is primarily caused by job-related stressors rather than personal issues. Strategies to prevent burnout include gaining insight into one's values, addressing feelings of isolation, building resilience through self-care, and reserving time for non-work activities and relationships.