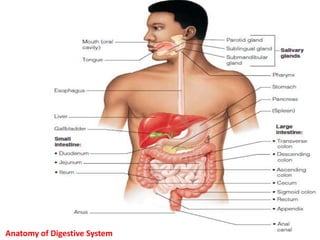
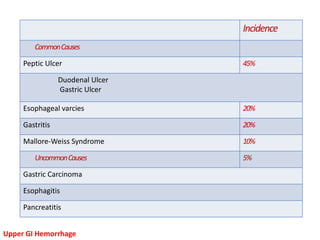
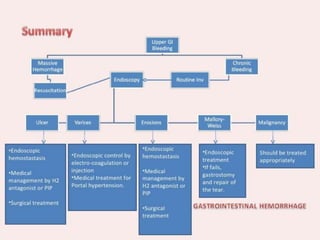
This document provides an overview of upper gastrointestinal hemorrhage. It defines upper GI hemorrhage as bleeding in the upper gastrointestinal tract below the ligament of Treitz. The most common causes are listed as peptic ulcer, portal hypertension, gastritis, and esophageal varices. Patients typically present with hematemesis, melena, or hematochezia. Diagnosis involves physical examination, lab tests, and endoscopic evaluation. Initial management focuses on stabilizing the patient and determining the source and rate of bleeding in order to guide specific treatment.