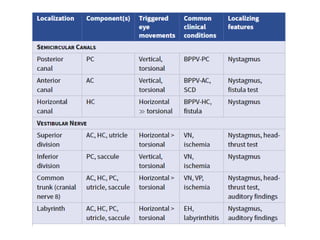
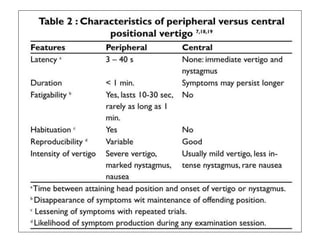
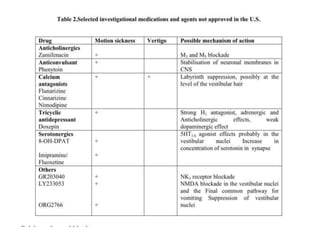
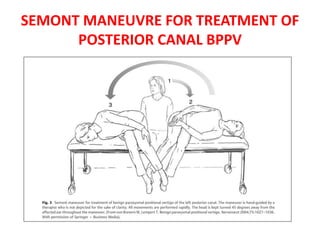
Vertigo is a common symptom that affects approximately 30% of people at some point in their life. There are many potential causes of vertigo, including benign paroxysmal positional vertigo (BPPV), vestibular neuritis, Meniere's disease, and less commonly central nervous system disorders. A thorough history, physical exam including tests of ocular motor function and positional maneuvers, and occasionally neuroimaging can help identify the underlying cause in most patients. The most common peripheral vestibular disorders like BPPV and vestibular neuritis are usually self-limited and the main treatment is symptomatic.