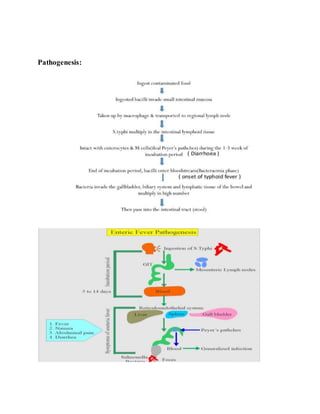
Typhoid fever is caused by the bacterium Salmonella typhi. It spreads through contaminated food, water, or close contact with infected carriers. Symptoms include sustained high fever, headaches, abdominal pain and constipation or diarrhea. It is diagnosed through blood or stool cultures and treated with antibiotics, though some chronic carriers still exist. Proper sanitation, hygiene and water treatment are crucial to prevent the spread of typhoid.