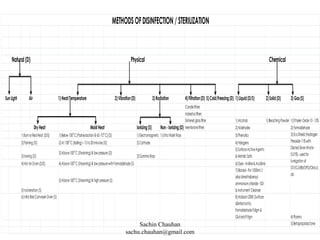
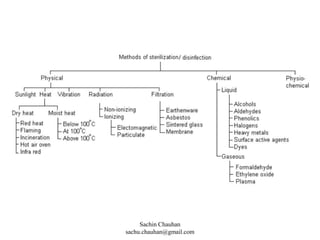
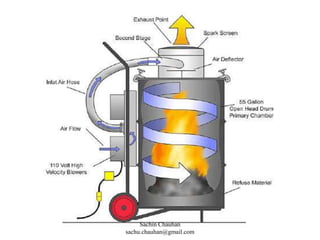
The document discusses various methods of disinfection and sterilization. It describes physical methods like dry heat which uses techniques like hot air ovens at 160°C for 1 hour to sterilize items. Moist heat methods are also discussed, which use steam under pressure to sterilize at temperatures above 100°C. Chemical methods involve the use of liquid disinfectants like alcohols, aldehydes and halogens or gaseous agents like ethylene oxide and formaldehyde. The different classifications of items based on sterility requirements - critical, semi-critical and non-critical are also mentioned.