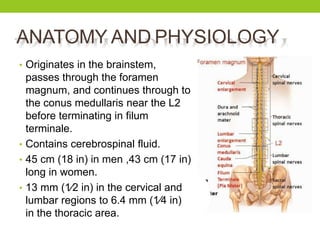
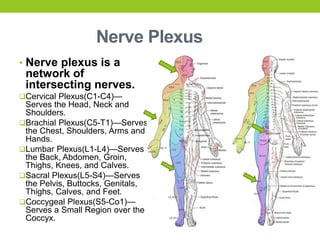
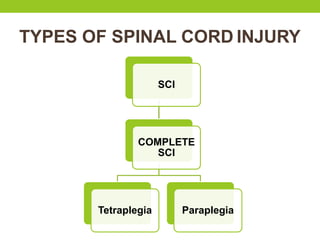
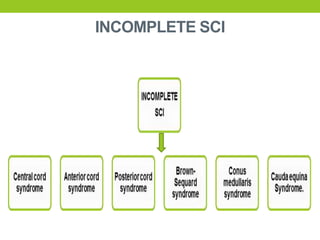
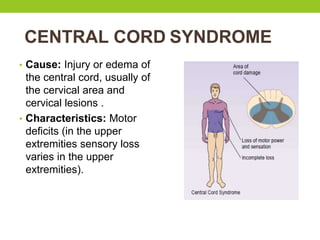
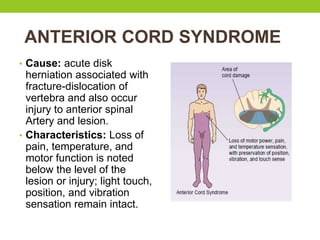
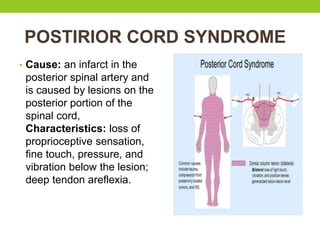
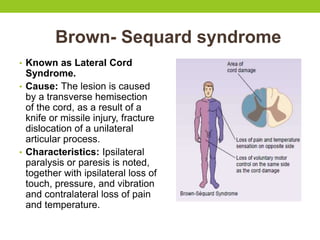
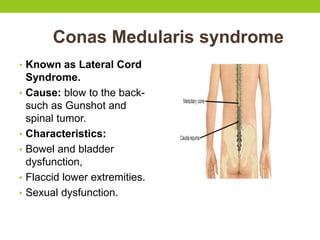
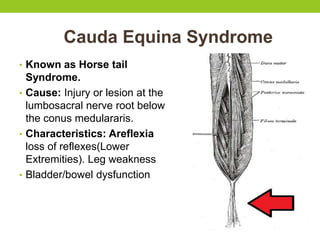
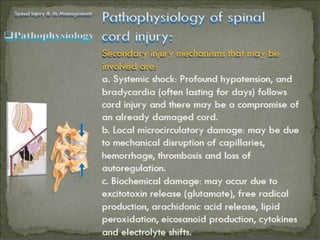
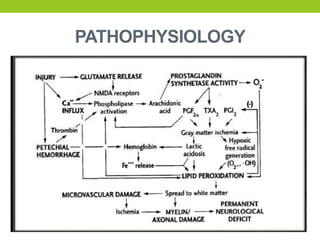
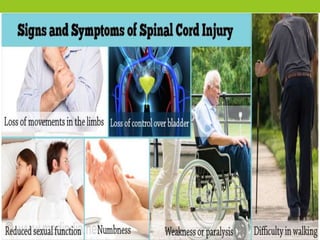
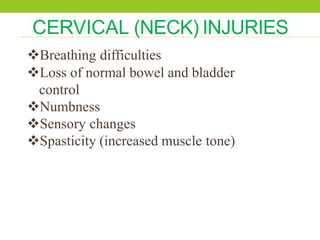
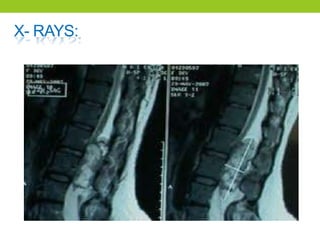
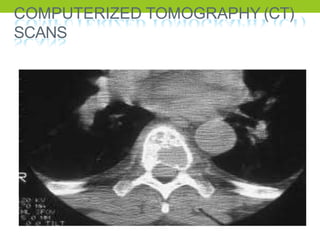
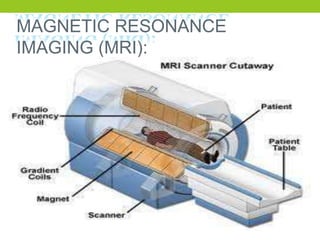
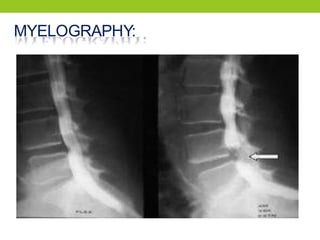
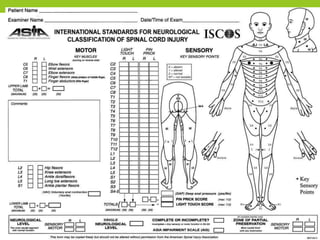
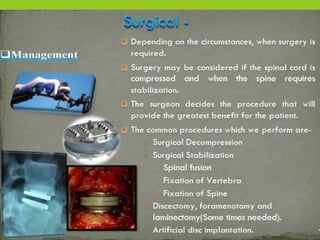
The document provides a comprehensive overview of spinal cord anatomy, types of injuries, their causes, symptoms, and management strategies. It details spinal cord injuries (SCI), including complete and incomplete classifications, as well as specific syndromes like Brown-Sequard and cauda equina syndromes. Additionally, it addresses diagnosis, treatment protocols, complications, and nursing management to optimize patient outcomes.