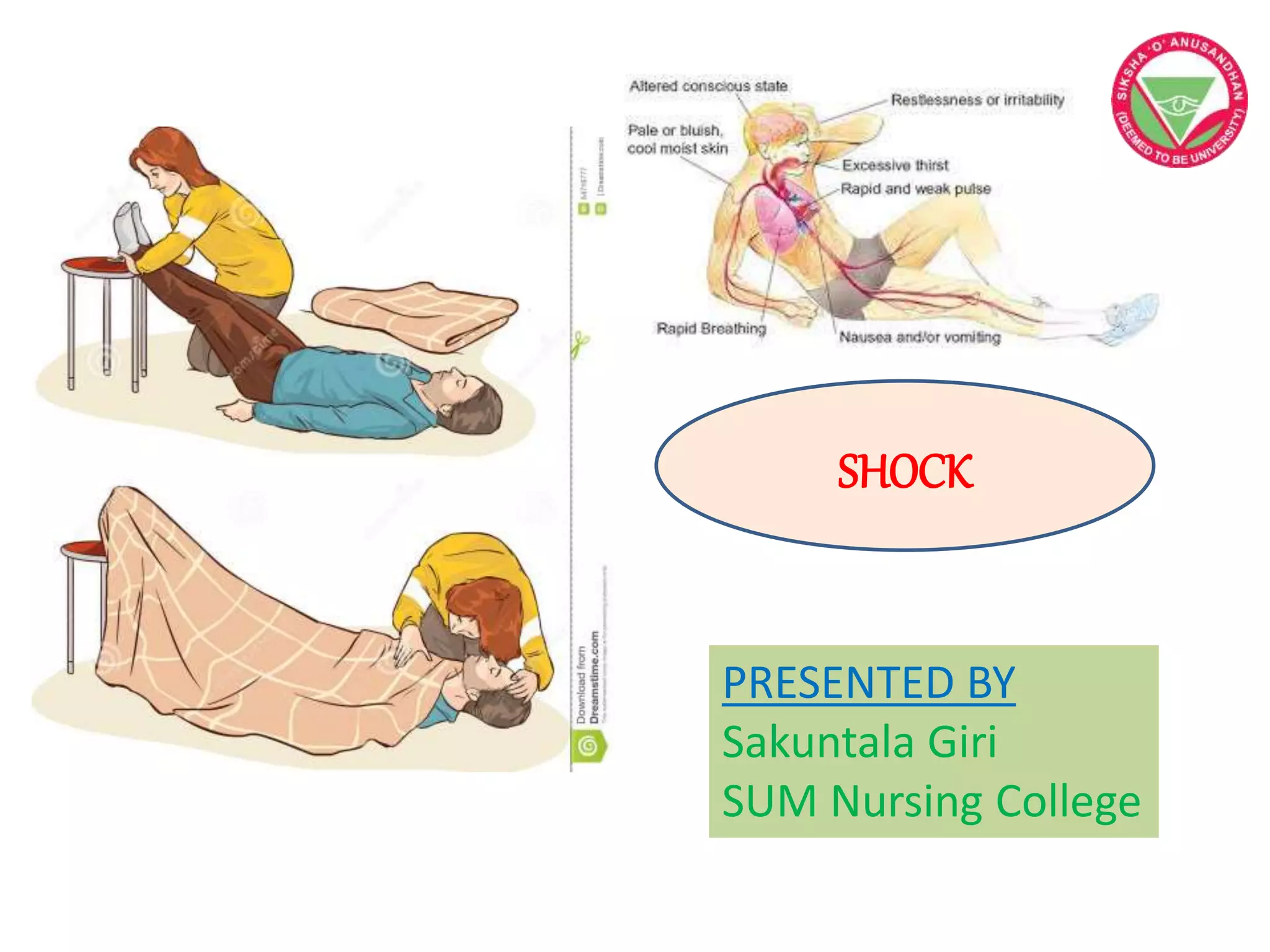
The document details the various types of shock, classified into hypovolemic, cardiogenic, septic, obstructive, neurogenic, and anaphylactic shocks, each with distinct etiologies, pathophysiology, and clinical manifestations. It explains the importance of timely diagnosis and management, including airway, breathing, circulation management, fluid replacement, and the use of vasoactive medication. Additionally, it covers hemorrhage definitions, types, clinical classifications, management strategies, and potential complications related to shock and bleeding.