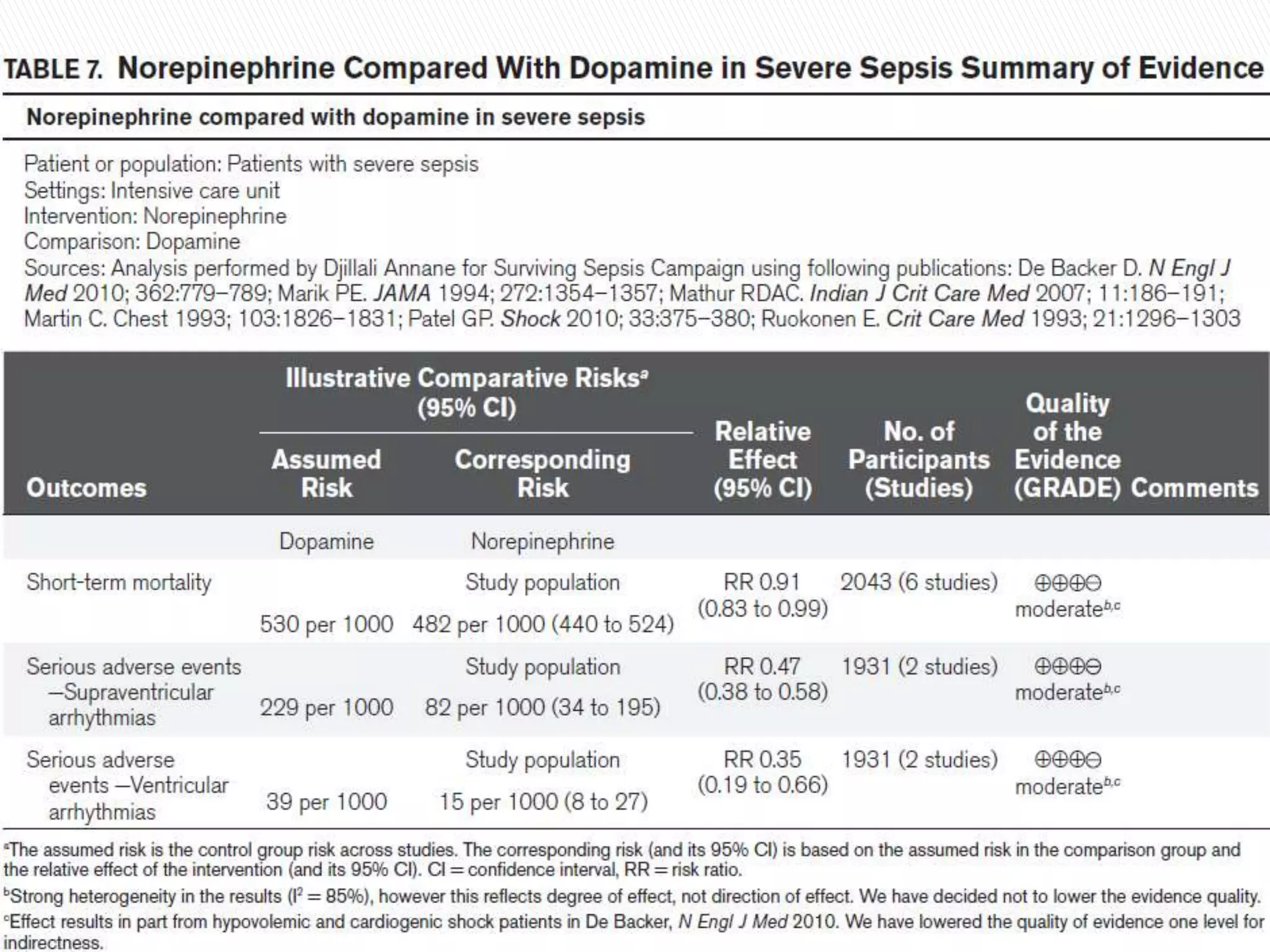
This document provides guidelines for the management of sepsis and septic shock. It defines key terms like sepsis, severe sepsis, septic shock, and systemic inflammatory response syndrome. It outlines variables for diagnosis and assessing organ dysfunction. It recommends initial resuscitation goals within 3-6 hours including measuring lactate, administering antibiotics and fluids, and applying vasopressors if needed. It provides guidelines for diagnosis, source control, antibiotic therapy, fluid therapy, vasopressor use, and other supportive treatments. Recommendations are evidence-based with assigned grade levels.