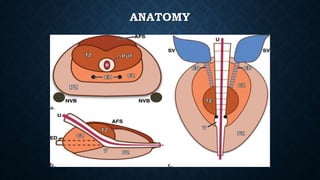
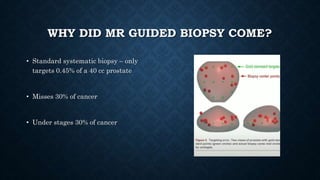
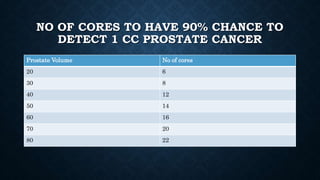
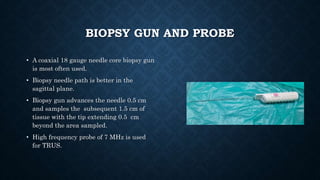
Prostate biopsy is commonly used to diagnose prostate cancer. Transrectal ultrasound guided biopsy is most common, but transperineal biopsy provides improved sampling. Extended biopsy schemes of 12 cores or more are now standard. Antibiotic prophylaxis and local anesthesia reduce risks of infection and pain. New techniques like MRI-fusion biopsy target suspected cancers more precisely. Overall, prostate biopsy remains a valuable tool but ongoing improvements aim to enhance safety, accuracy and ability to detect clinically significant cancers.