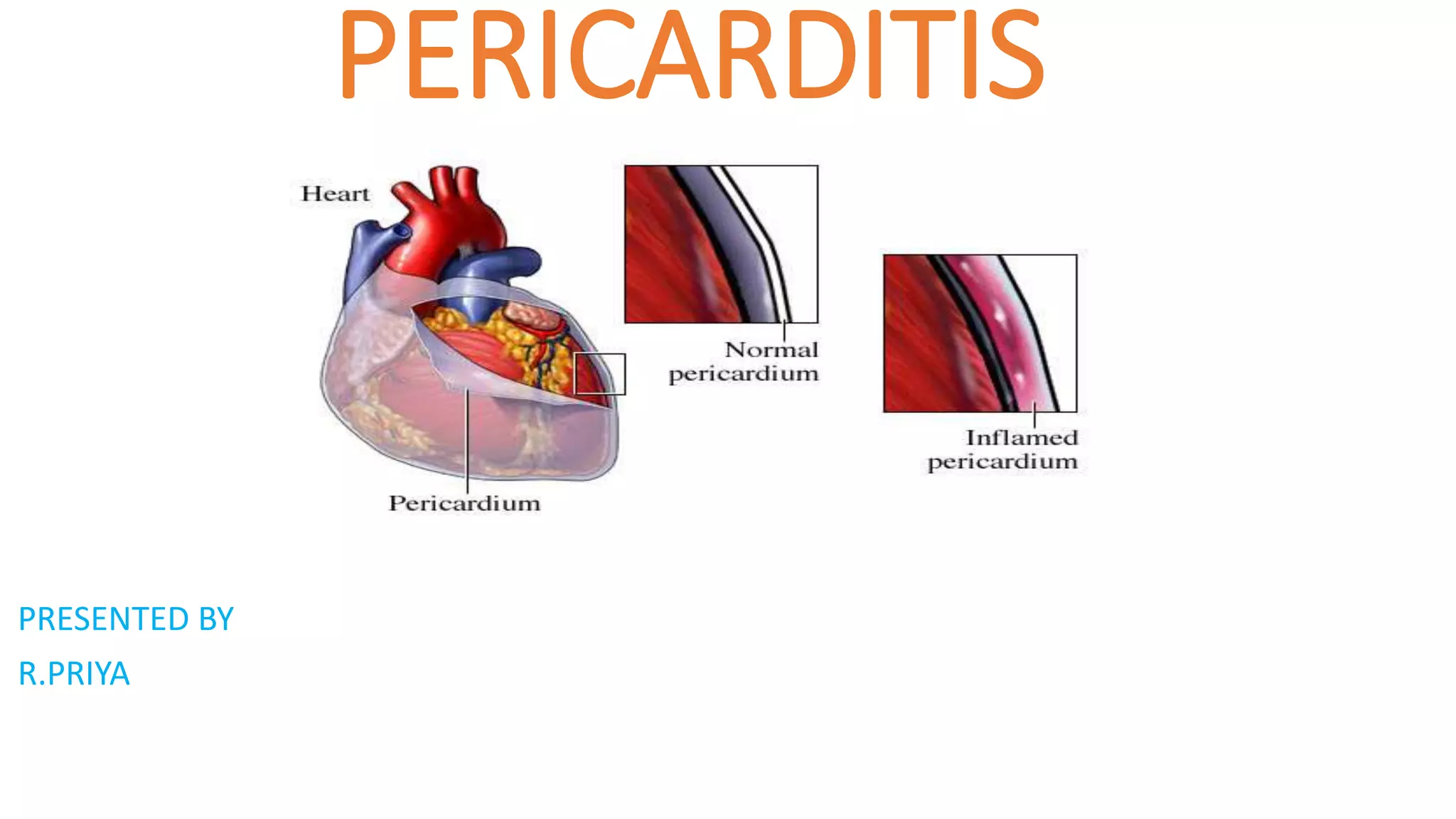
Pericarditis is an inflammation of the pericardium that commonly affects men aged 20-50. It has several causes including viral or bacterial infections, certain cancers, autoimmune diseases, or physical trauma. Symptoms include chest pain that increases with deep breathing or lying flat. Diagnosis involves electrocardiograms, echocardiograms, and blood tests. Treatment focuses on reducing inflammation with medications like aspirin, ibuprofen, or colchicine. Surgery may be required in severe cases to drain fluid or remove the pericardium.