Paediatric resuscitation & choking
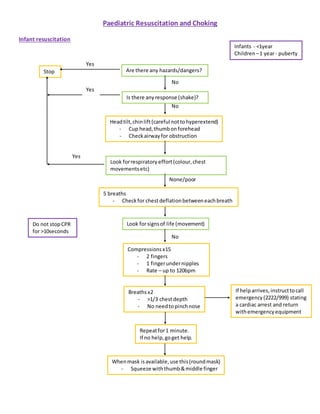
- 1. Paediatric Resuscitation and Choking Infant resuscitation Infants - <1year Children –1 year- puberty Yes Are there any hazards/dangers? Yes Stop Headtilt,chinlift(careful nottohyperextend) - Cup head,thumbonforehead - Checkairwayfor obstruction Compressionsx15 - 2 fingers - 1 fingerundernipples - Rate – up to 120bpm Whenmask isavailable,use this(roundmask) - Squeeze withthumb&middle finger Repeatfor1 minute. If no help,goget help. If helparrives,instructtocall emergency(2222/999) stating a cardiac arrest and return withemergencyequipment Breathsx2 - >1/3 chestdepth - No needtopinchnose Do not stopCPR for >10seconds No Yes Yes No None/poor No Look forrespiratory effort(colour,chest movementsetc) Look forsignsof life (movement) Is there anyresponse (shake)? 5 breaths - Checkfor chestdeflationbetweeneachbreath
- 2. Child resuscitation Are there any hazards/dangers? Yes Stop Headtilt,chinlift(careful nottohyperextend) - Holdheadbetween2fingers - Checkairwayfor obstruction Compressionsx15 - 1 hand(small child),2hands(large child) - Positionasinadults - Rate – up to 120bpm Whenmask isavailable,use this(shapedmask) - Squeeze withthumb&middle finger Repeatfor1 minute. If no help,goget help. If helparrives,instructtocall emergency(2222/999) stating a cardiac arrest and return withemergencyequipment Breathsx2 - >1/3 chestdepth - No needtopinchnose Do not stopCPR for >10seconds No Yes Yes No None/poor No Look forrespiratoryeffort(colour,chest movementsetc) Look forsignsof life (movement) Is there any response (shake)? 5 breaths - Checkfor chestdeflationbetweeneachbreath Yes
- 3. Infant choking Child choking Yes No Is there efforttocough?CPR (from5 rescue breaths) Holdmandible betweenthumb& forefinger,putyourarm across their chestand flipthemover. If obstructingobject isobviousinthe airwayremove it. Poor Good Is the effortpooror good? Administer5 backblows - Usingheel of hand - Between shoulderblades - Checkaftereach one for successful removal of object If childbecomesunconscious, performCPR.If effortbecomes poor,performthrusts. If infantisstill chokingafter5 back blows/thrusts,call forhelp Place infantacrossarm/lapin a head-downwardsupineposition Deliver5chestthrusts: - Like compressions,but harderand slower - Checkaftereach one for successful removal of object Yes No Is there efforttocough?CPR (from5 rescue breaths) Lean childforward,placingyourarm across theirchestto supportthem. If obstructingobject isobviousinthe airwayremove it. Poor Good Is the effortpooror good? Administer5 backblows - Usingheel of hand - Betweenshoulderblades - Checkaftereach one for successful removal of object If childbecomesunconscious, performCPR.If effortbecomes poor,performthrusts. If infantisstill chokingafter5 back blows/thrusts,call forhelp Lean child forward, standingbehindthem Deliver5abdominal thrusts: - One hand ina fist,sidewaysinto child’sabdomen,otherhandontop - Movement– up intodiaphragm, towardsyour chest Encourage coughing