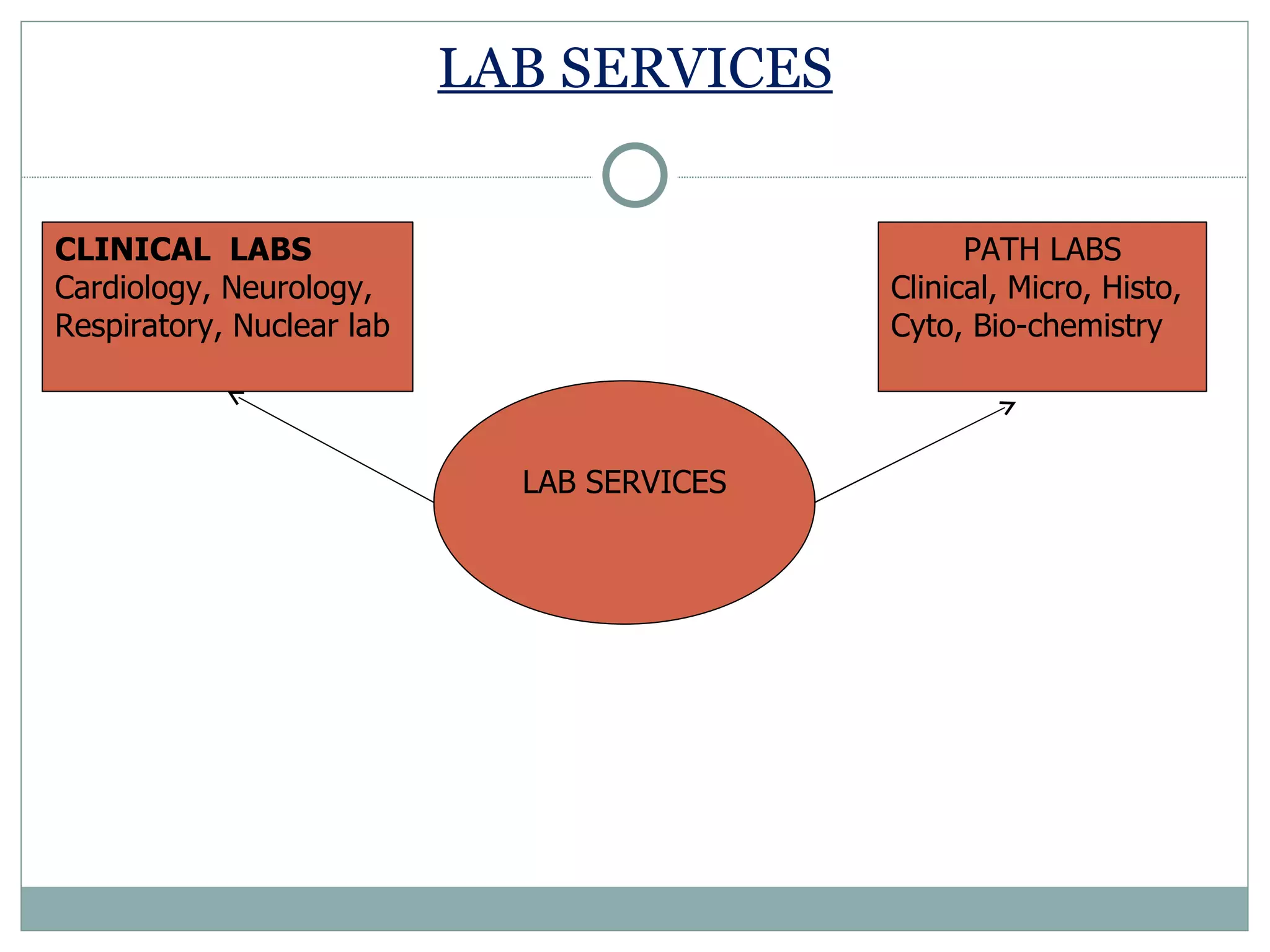
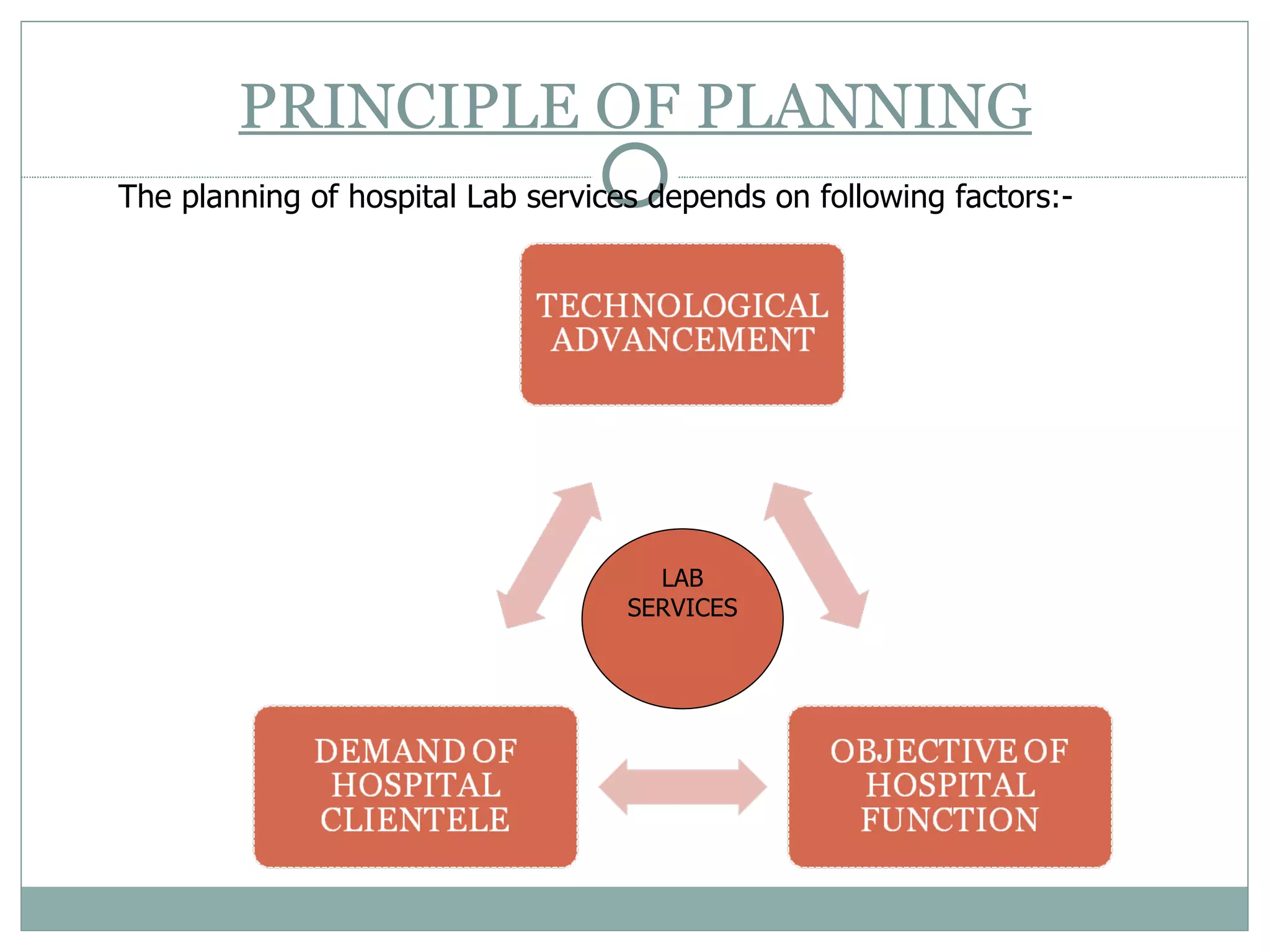
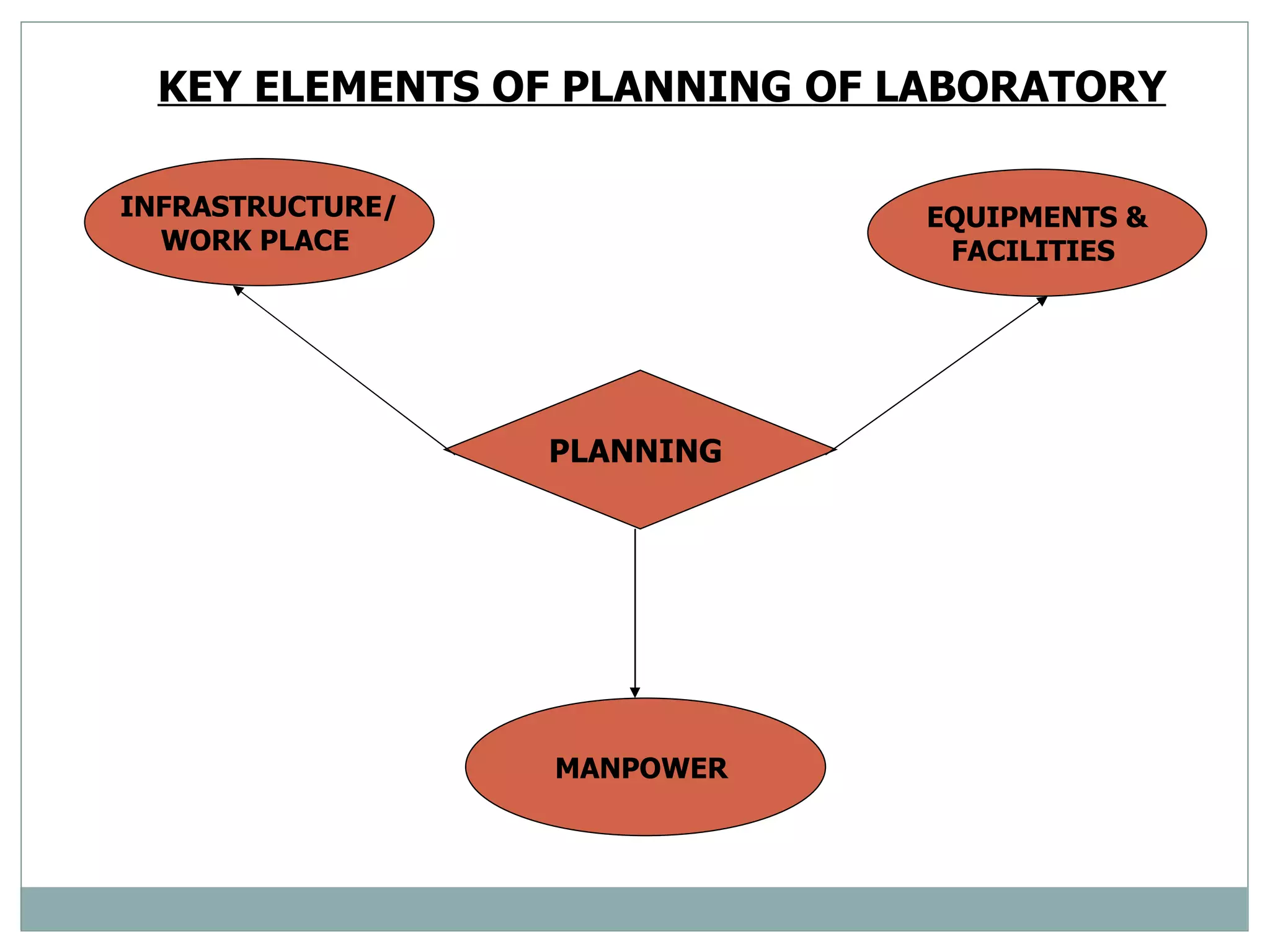
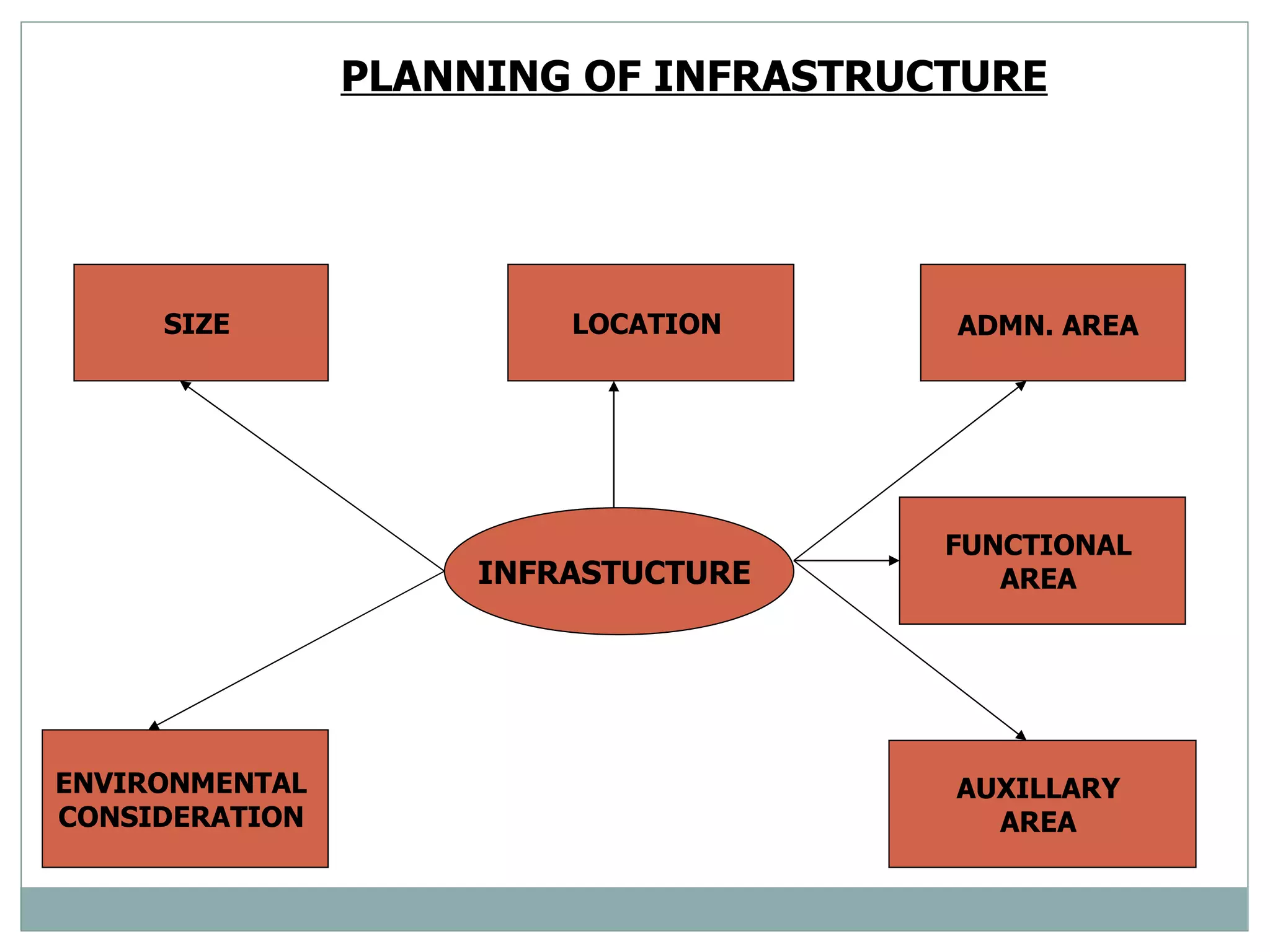
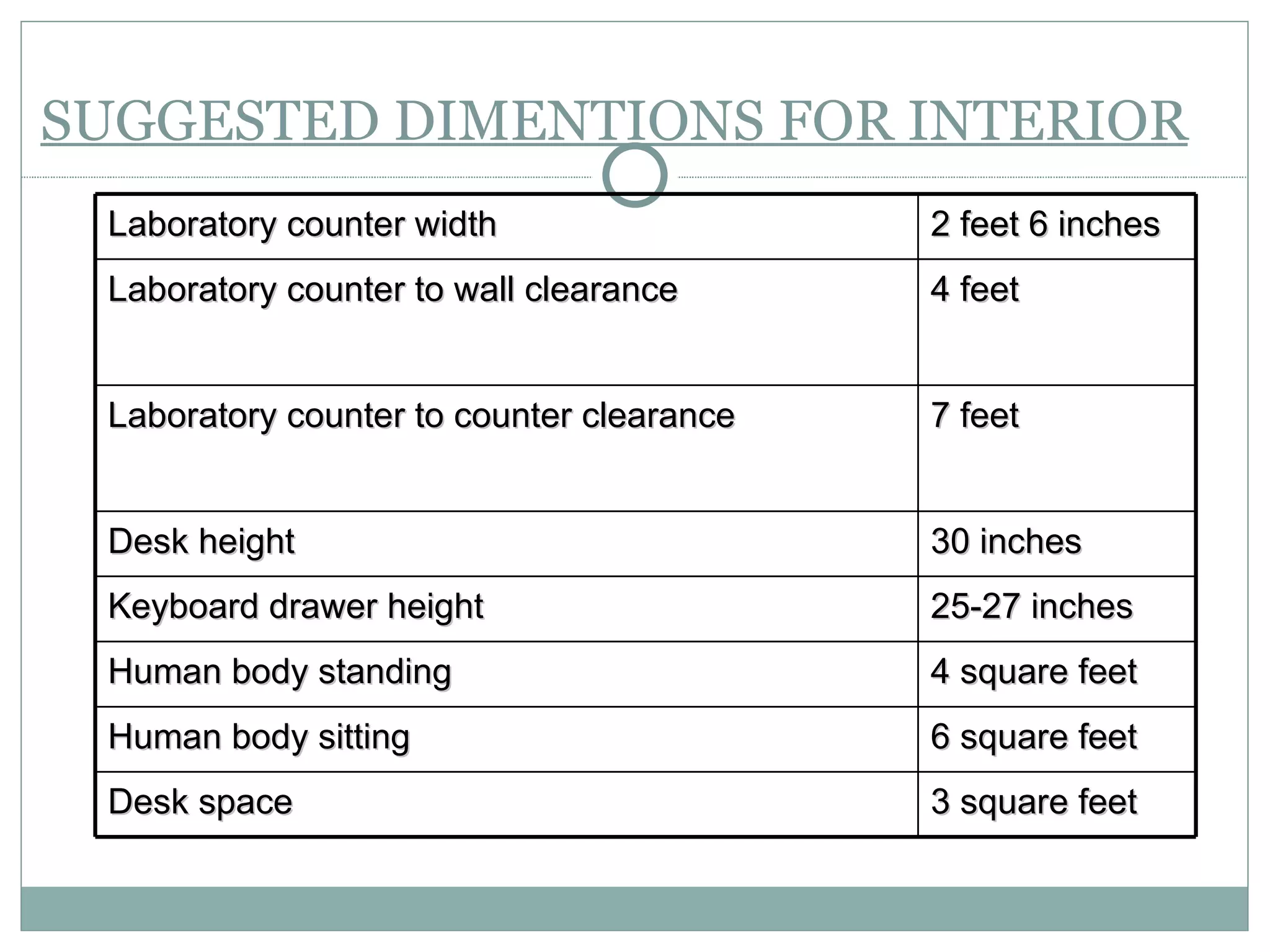
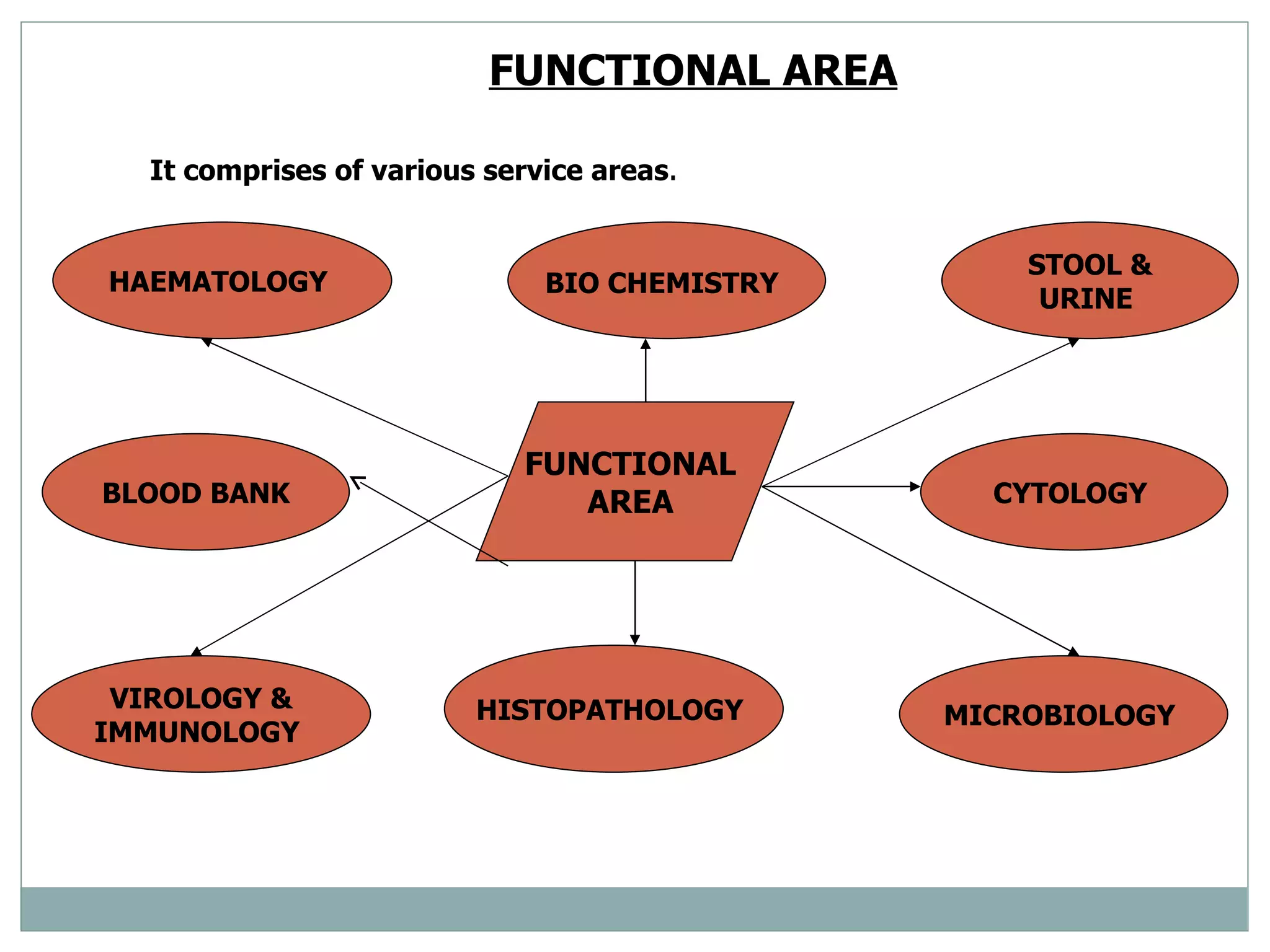
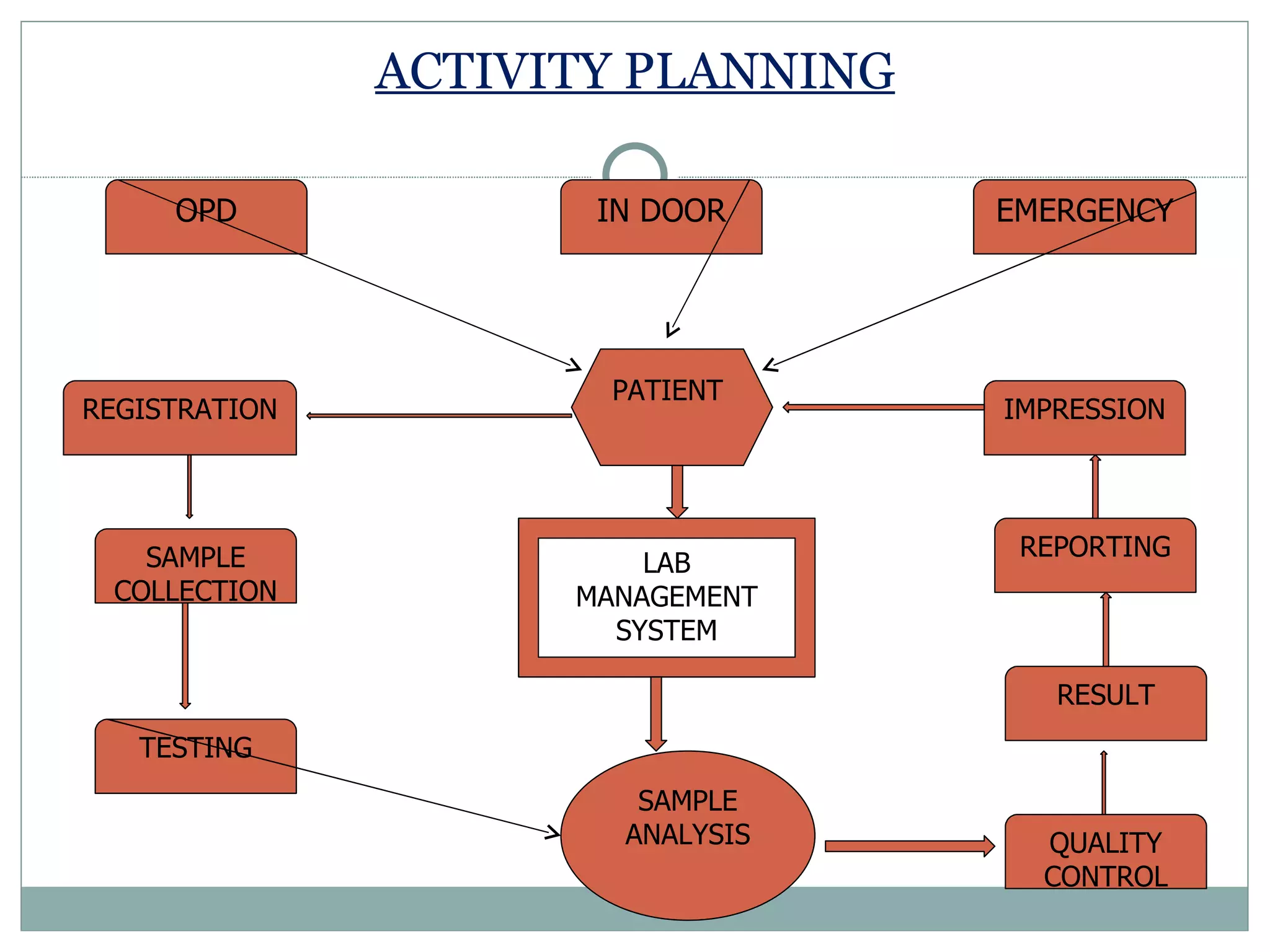
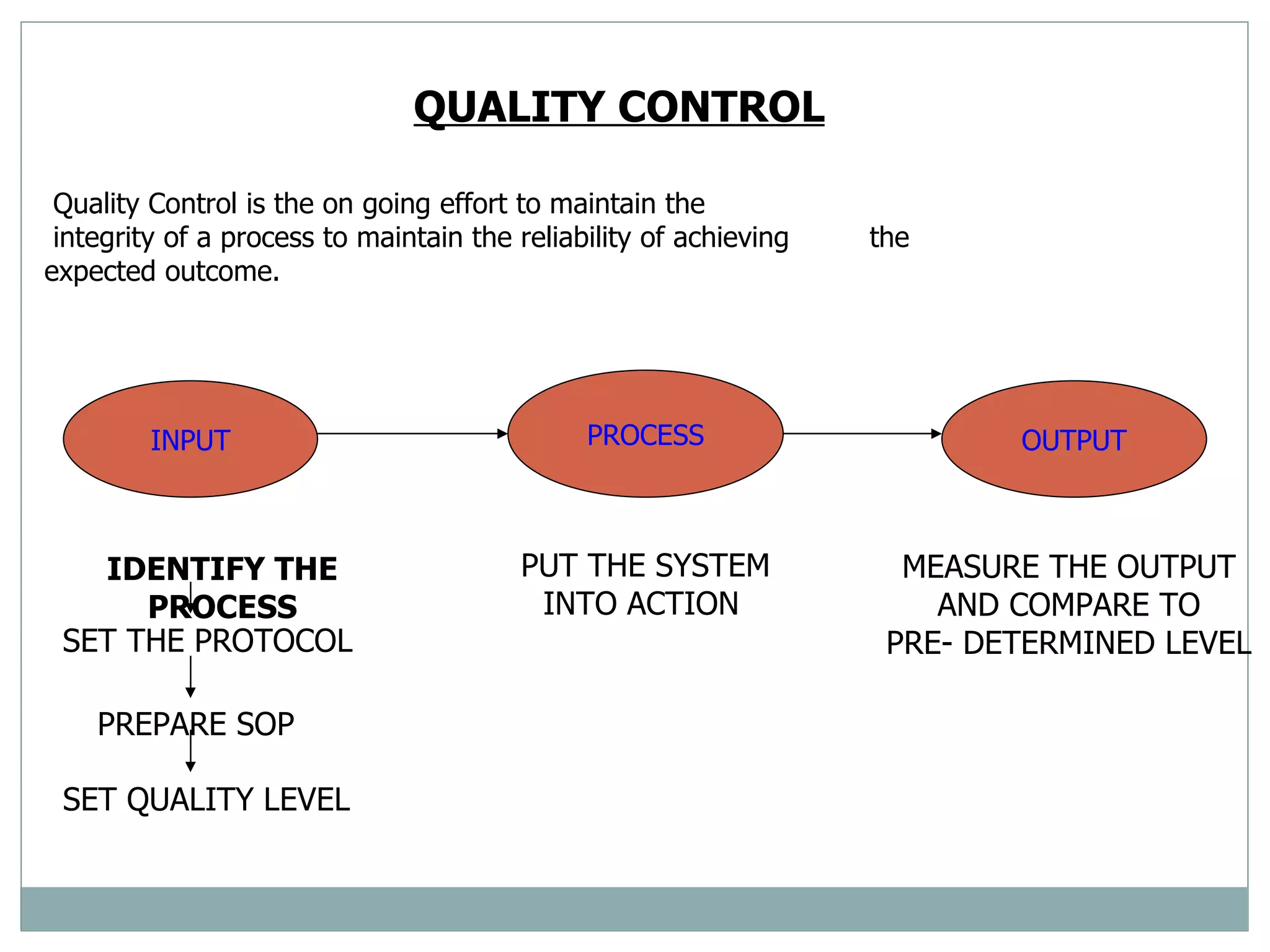
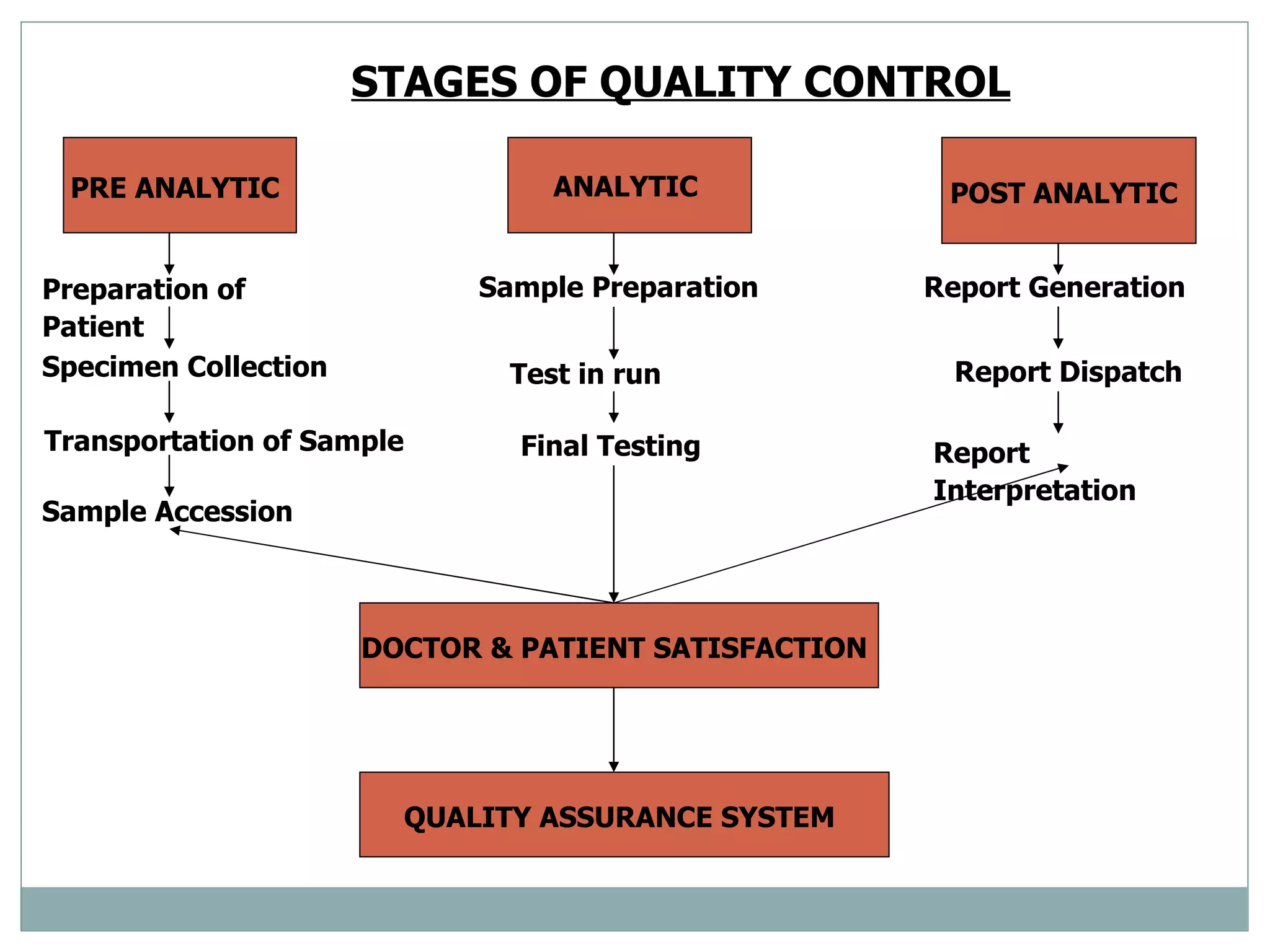
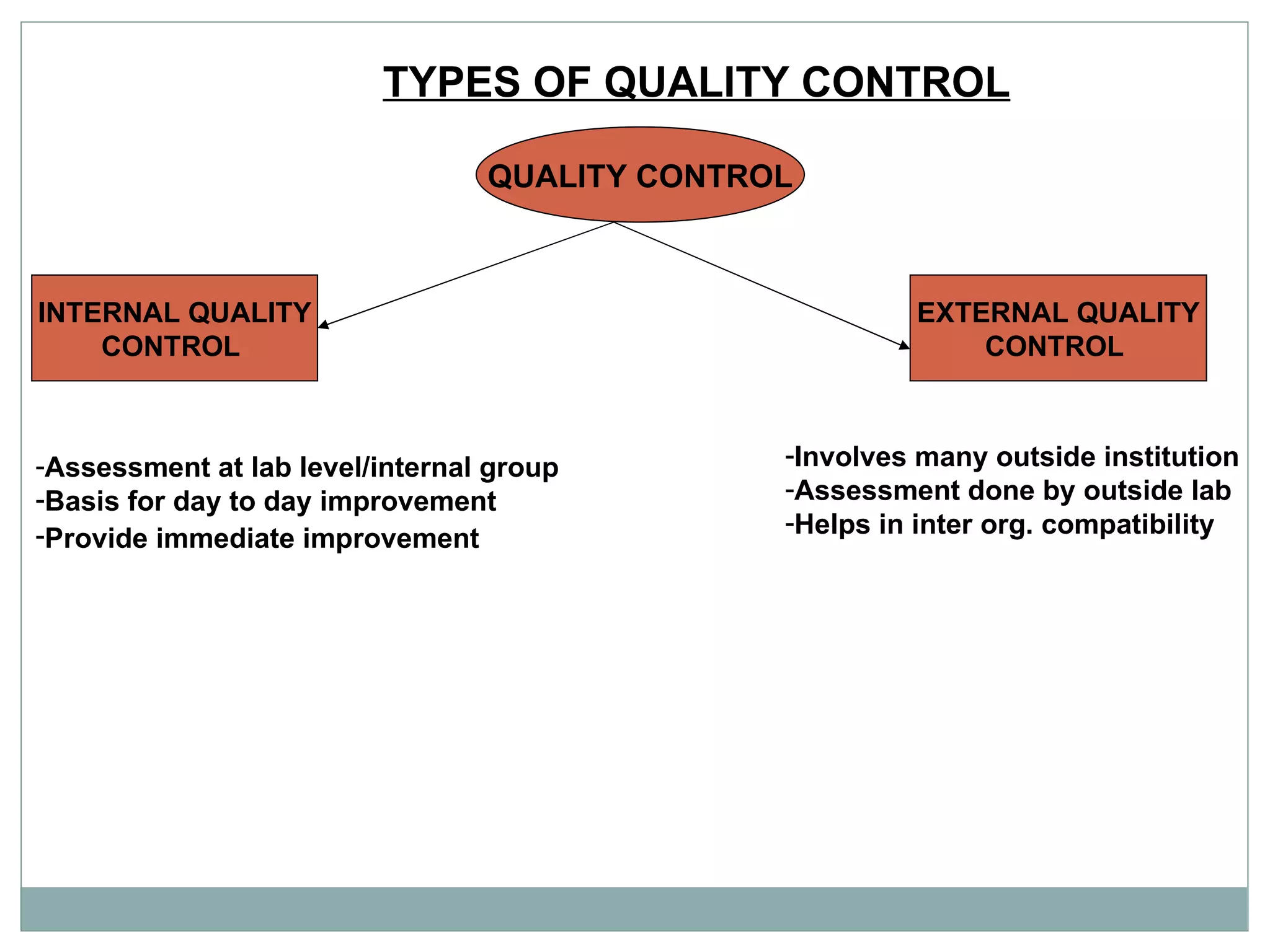
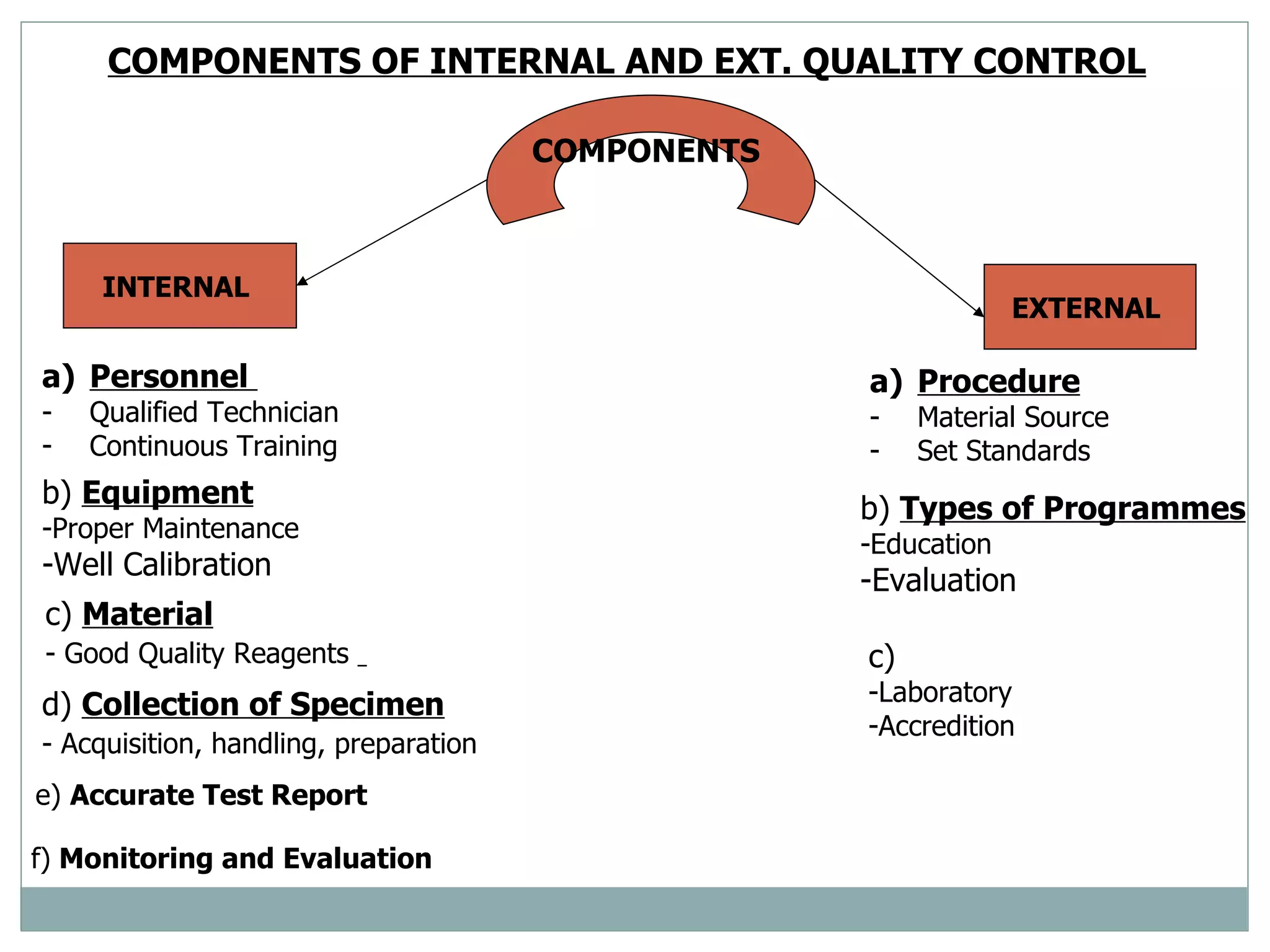
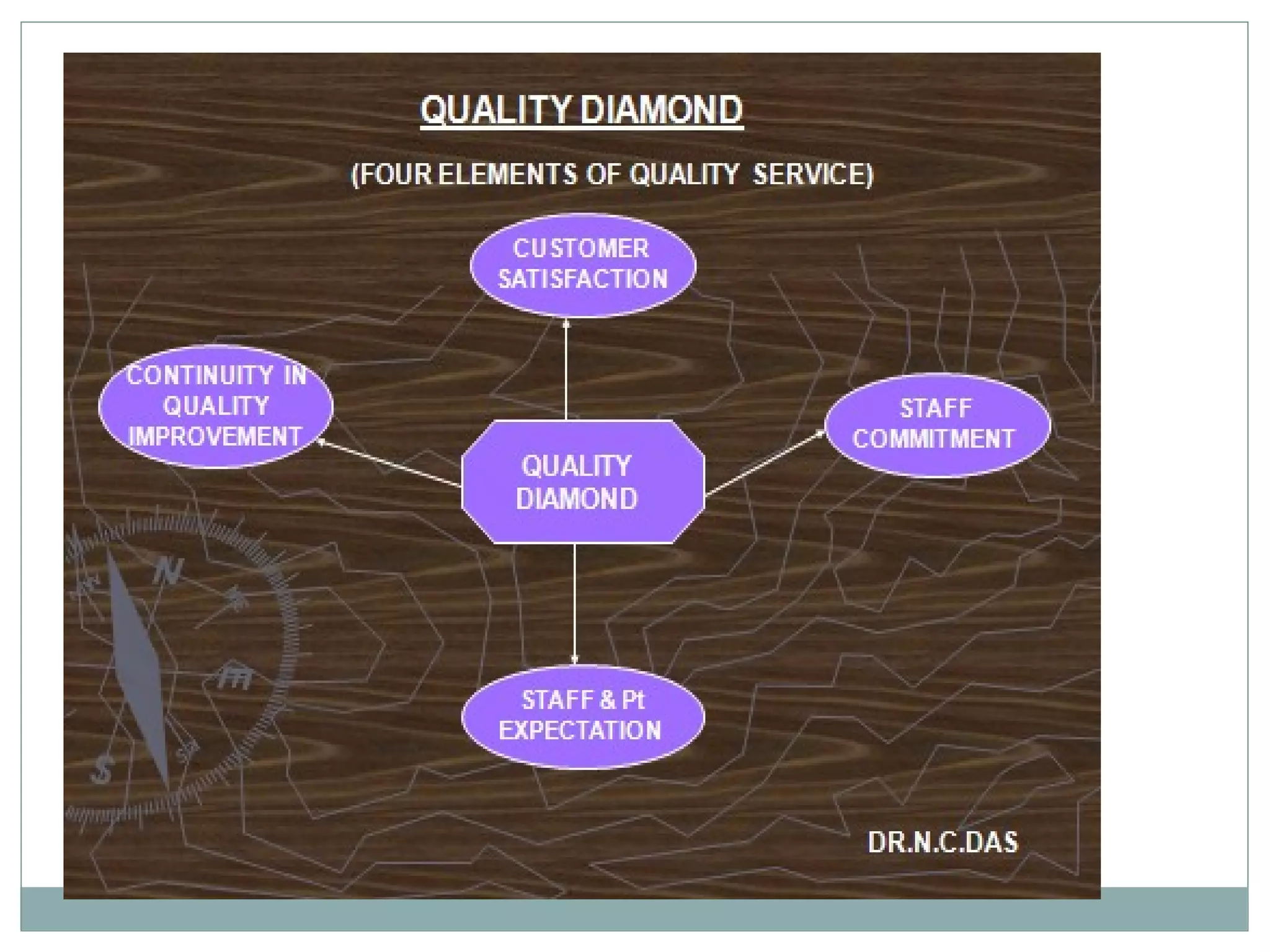
The document discusses the organization and planning of laboratory services in a hospital. It covers key aspects like types of clinical and pathology labs, changing role of labs, importance of labs, principles of planning, infrastructure planning considering size, location, functional areas, quality control and quality assurance. The goal is to provide accurate and timely diagnostic support through well-planned lab services.