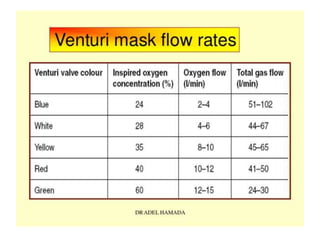
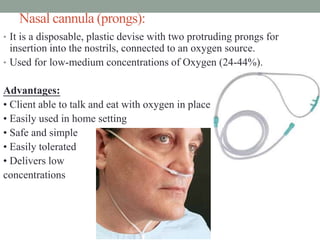
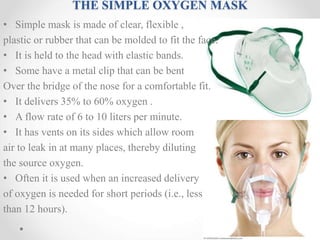
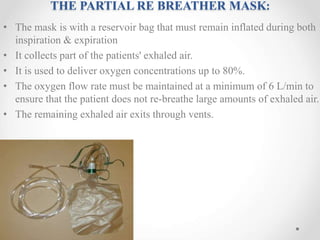
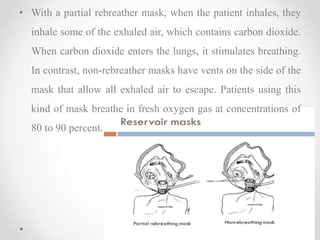
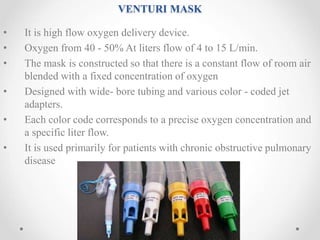
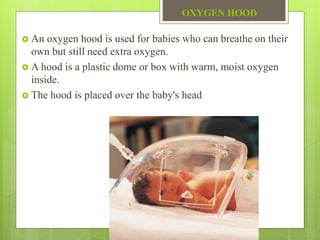
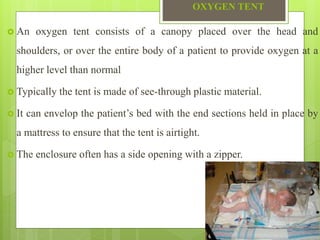
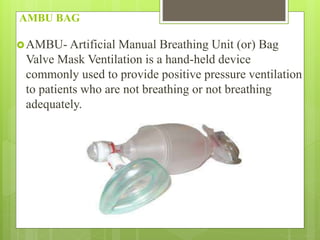
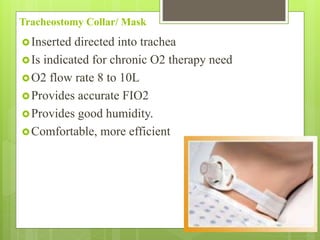
Oxygen therapy is the administration of oxygen at concentrations greater than 21% to treat conditions like hypoxia and respiratory failure. It can be delivered through nasal cannulas, masks, tents, or ventilators. Precise monitoring is needed to ensure safe and effective delivery while avoiding toxicity from high concentrations over long periods.