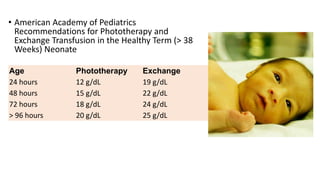
This document provides guidelines for the management of common neonatal emergencies encountered in the emergency department. It outlines the assessment steps, diagnostic workup and initial stabilization measures for respiratory distress, cardiac issues like cyanotic heart disease and supraventricular tachycardia, shock, decreased consciousness, apnea, and various endocrine emergencies including congenital adrenal hyperplasia and thyrotoxicosis. History taking, physical exam focusing on ABCDE, appropriate diagnostic tests and consultation with pediatric specialists are emphasized.


























![Sepsis
• It is standard of care to complete a full sepsis evaluation (CBC, blood culture,
urinalysis, urine culture, cerebral spinal fluid [CSF] culture and analysis, and
CXR) in any neonate with a rectal temperature of ≥ 100.4° F. = 38 C
• The symptoms are nonspecific : poor feeding, irritability, apnea, hypothermia, jaundice,
rashes, increased sleeping, seizures, or vomiting.
• A thorough maternal history and physical examination may be helpful.
• Initial laboratory :.
• WBC COUNT is not helpful to differentiate febrile neonates with a more serious bacterial
infection from those without a serious bacterial infection.
• One study demonstrated that a low WBC count increased the odds of bacterial
meningitis.
• In addition, the urinalysis may also be unremarkable in those neonates with a culture
positive UTI.
• 14% of febrile neonates will be diagnosed with a UTI](https://image.slidesharecdn.com/neonatalemergenciesguidelines-181113101542/85/Neonatal-emergencies-guidelines-28-320.jpg)