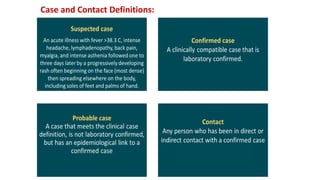
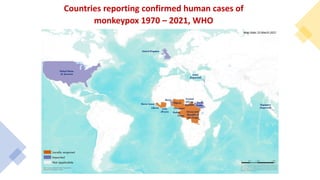
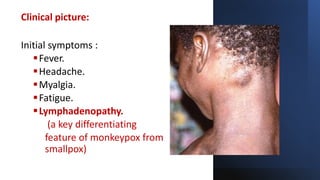
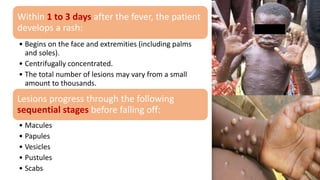
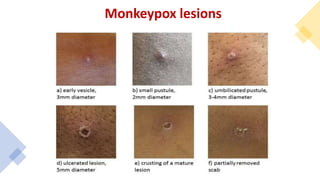
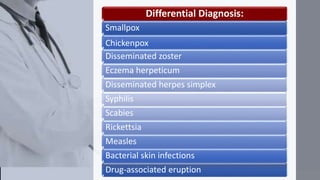
The document discusses the monkeypox virus, its epidemiology, transmission modes, and outbreaks, including significant events from 2003 to 2022. It emphasizes the importance of prevention, vaccination, diagnosis, and treatment approaches, as well as the role of family physicians in case management. Additionally, the document outlines the public health response to outbreaks, contact tracing protocols, and patient isolation measures.





















































![References:
• CDC. About Monkeypox | Monkeypox| Poxvirus | CDC [Internet]. 2018 [cited 2019 Oct
19]. Available from: https://www.cdc.gov/poxvirus/monkeypox/about.html
• WHO. Monkeypox [Internet]. WHO. 2016 [cited 2019 Oct 19]. Available from:
https://www.who.int/news-room/fact-sheets/detail/monkeypox
• "Monkeypox," UK Health Security Agency, 18 May 2022. [Online]. Available:
https://www.gov.uk/guidance/monkeypox#transmission.
• https://www.gov.uk/government/news/monkeypox-cases-confirmed-in-england-latest-
updates
• Durski KN, McCollum AM, Nakazawa Y, Petersen BW, Reynolds MG, Briand S, et al.
Emergence of monkeypox – West and Central Africa, 1970–2017. Morb Mortal Wkly Rep.
2018 Mar 16;67(10):306–10.
• NCDC. Nigeria Centre for Disease Control: Weekly Epidemiological Report [Internet].
2017 [cited 2019 Oct 19]. Available from: https://ncdc.gov.ng/reports/101/2017-december-
week-52](https://image.slidesharecdn.com/monkeypoxoutbreak-220531191744-c1338cfa/85/Monkeypox-Outbreak-2022-pptx-67-320.jpg)
![• "Epidemiological update: Monkeypox outbreak," European Centre for Disease Prevention
and Control, 20 May 2022. [Online]
• Placide K Mbala, John W Huggins, Therese Riu-Rovira, Steve M Ahuka, Prime
Mulembakani, Anne W Rimoin, James W Martin, Jean-Jacques T Muyembe, Maternal and
Fetal Outcomes Among Pregnant Women With Human Monkeypox Infection in the
Democratic Republic of Congo, The Journal of Infectious Diseases, Volume 216, Issue 7, 1
October 2017, Pages 824–828, https://doi.org/10.1093/infdis/jix260
• https://www.nature.com/articles/d41586-022-
014218?utm_source=Nature+Briefing&utm_campaign=722ea2a64d-briefing-wk-
20220520&utm_medium=email&utm_term=0_c9dfd39373-722ea2a64d-42456515
• https://www.who.int/publications/i/item/WHO-MPX-laboratory-2022.1](https://image.slidesharecdn.com/monkeypoxoutbreak-220531191744-c1338cfa/85/Monkeypox-Outbreak-2022-pptx-68-320.jpg)
