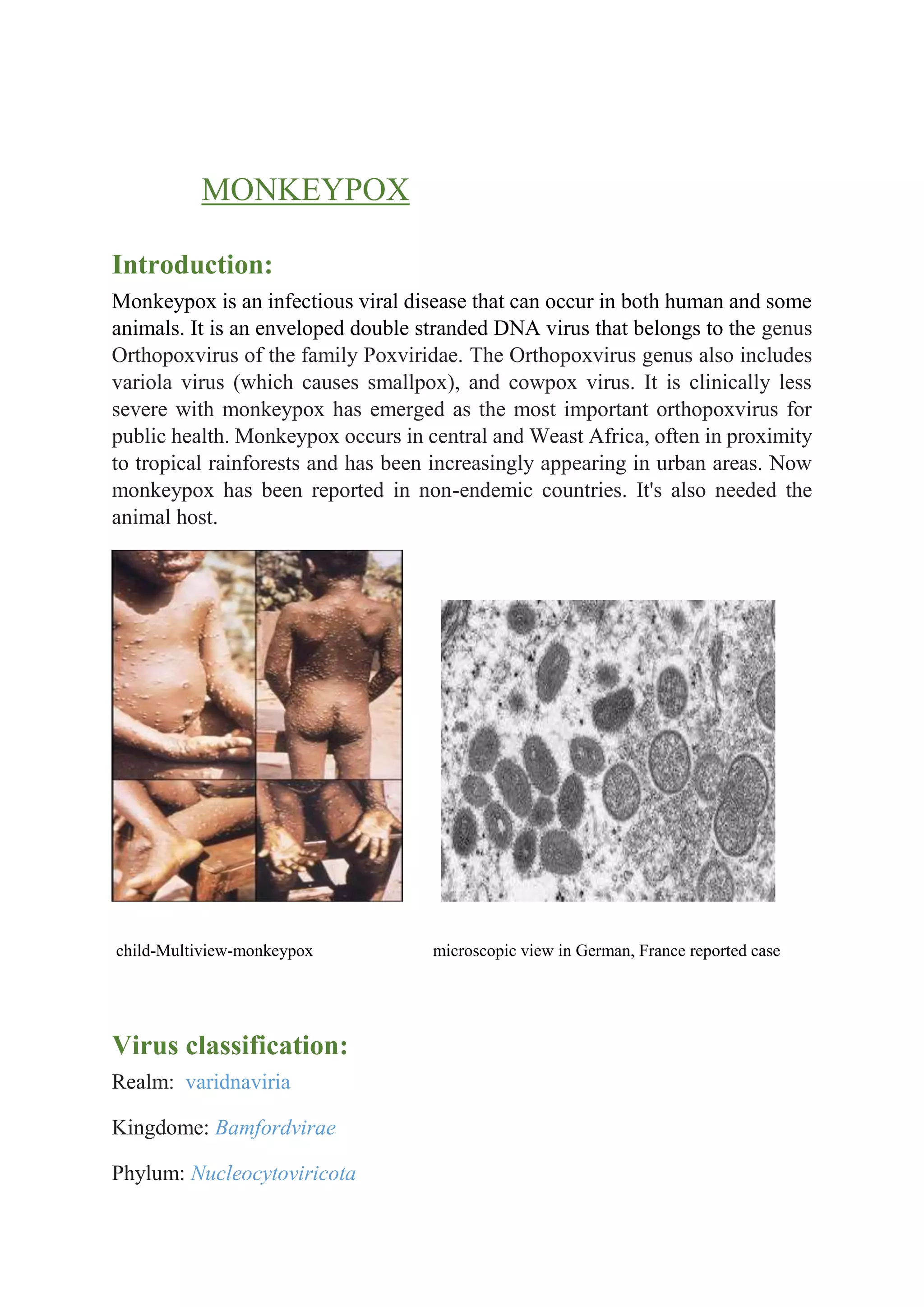
Monkeypox is a viral disease that occurs in humans and some animals. It is caused by the monkeypox virus, which belongs to the same family of viruses as smallpox. Monkeypox most commonly spreads through direct contact with infected animals or humans. Initial symptoms include fever, headache, muscle aches, and swollen lymph nodes. Within a few days, a rash develops on the face and spreads to other parts of the body. While monkeypox is generally mild, it can cause severe illness and has a fatality rate of around 1 in 10 people in parts of Africa. There are vaccines and treatments available to prevent and treat monkeypox infections.