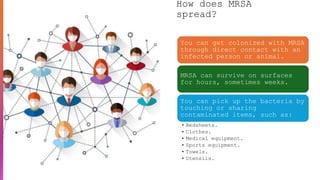
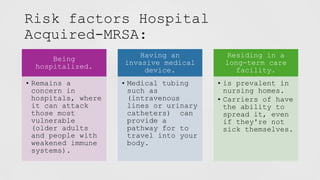
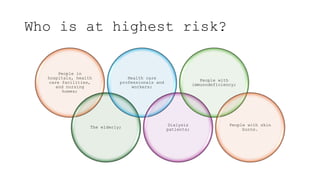
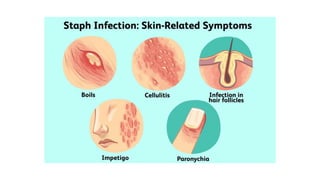
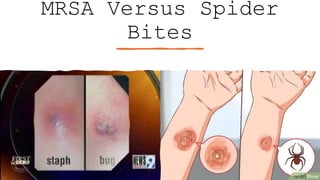
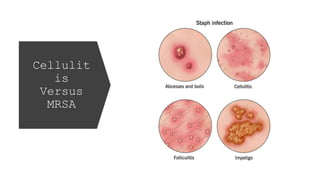
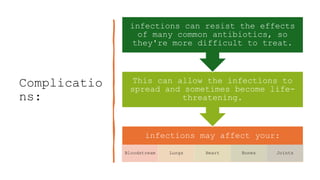
Methicillin-resistant Staphylococcus aureus (MRSA) is a type of staph bacteria resistant to many antibiotics, causing infections ranging from minor skin issues to severe organ complications. It can be categorized into hospital-associated (HA) MRSA and community-associated (CA) MRSA, with transmission occurring through contact with infected individuals, contaminated surfaces, or personal items. Prevention includes rigorous hand hygiene, proper wound care, and avoiding sharing personal items.