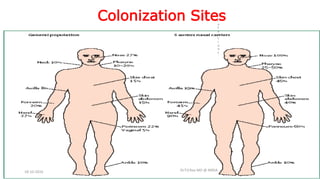
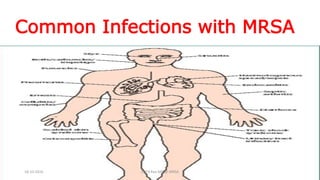
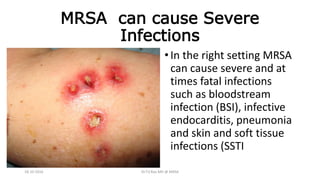
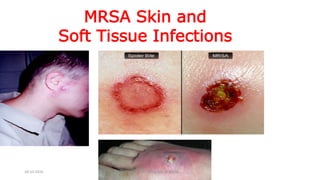
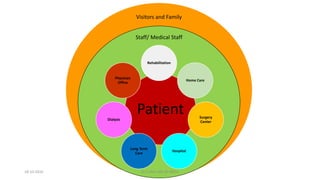
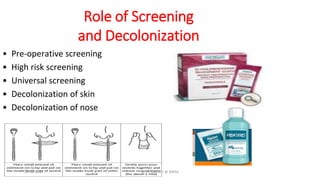
The document discusses MRSA infections, including their history, epidemiology, risk factors, management, and prevention. It provides definitions of MRSA and outlines strategies to prevent healthcare-associated transmission through practices like hand hygiene, contact precautions, appropriate antibiotic use, and environmental decontamination. Education of healthcare workers and patients is emphasized as a key prevention strategy.