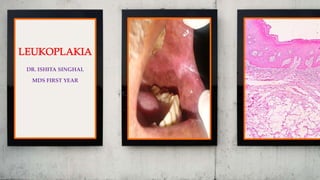
The document presents a clinical case of a 73-year-old male patient with complaints of pain and sensitivity in the lower left back tooth region, along with an intraoral examination revealing a speckled leukoplakia in the left retro-commissural area of the lip. A punch biopsy indicated mild dysplasia, suggesting potential precancerous changes associated with leukoplakia, which can arise from factors like tobacco use and chronic irritation. The document includes details about the diagnostic criteria, differential diagnosis, and histological features relevant to leukoplakia.