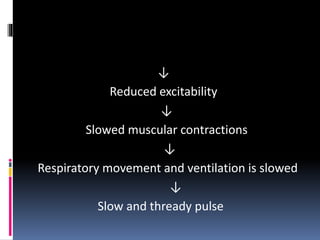
Hypokalemia is a low serum potassium level defined as less than 3.5 mEq/L. It can be caused by gastrointestinal losses from vomiting, diarrhea, or medications like diuretics. Symptoms include muscle weakness, paralysis, cardiac arrhythmias, respiratory issues, and neurological effects. Treatment involves oral or IV potassium supplementation depending on severity while monitoring for hyperkalemia. Dietary sources of potassium like fruits and vegetables can help correct hypokalemia.