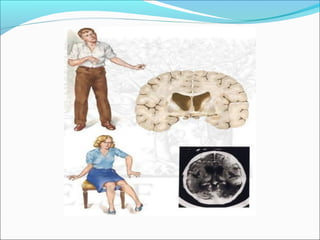
Huntington's disease is a progressive neurodegenerative disorder caused by a defective gene that results in the production of an abnormal protein called huntingtin. It affects movement, cognition, and personality. Symptoms include uncontrolled movements, impaired walking and talking, and mood and cognitive changes. There is currently no cure, but treatments can help manage symptoms. The disease is inherited in an autosomal dominant pattern and typically appears in middle adulthood.