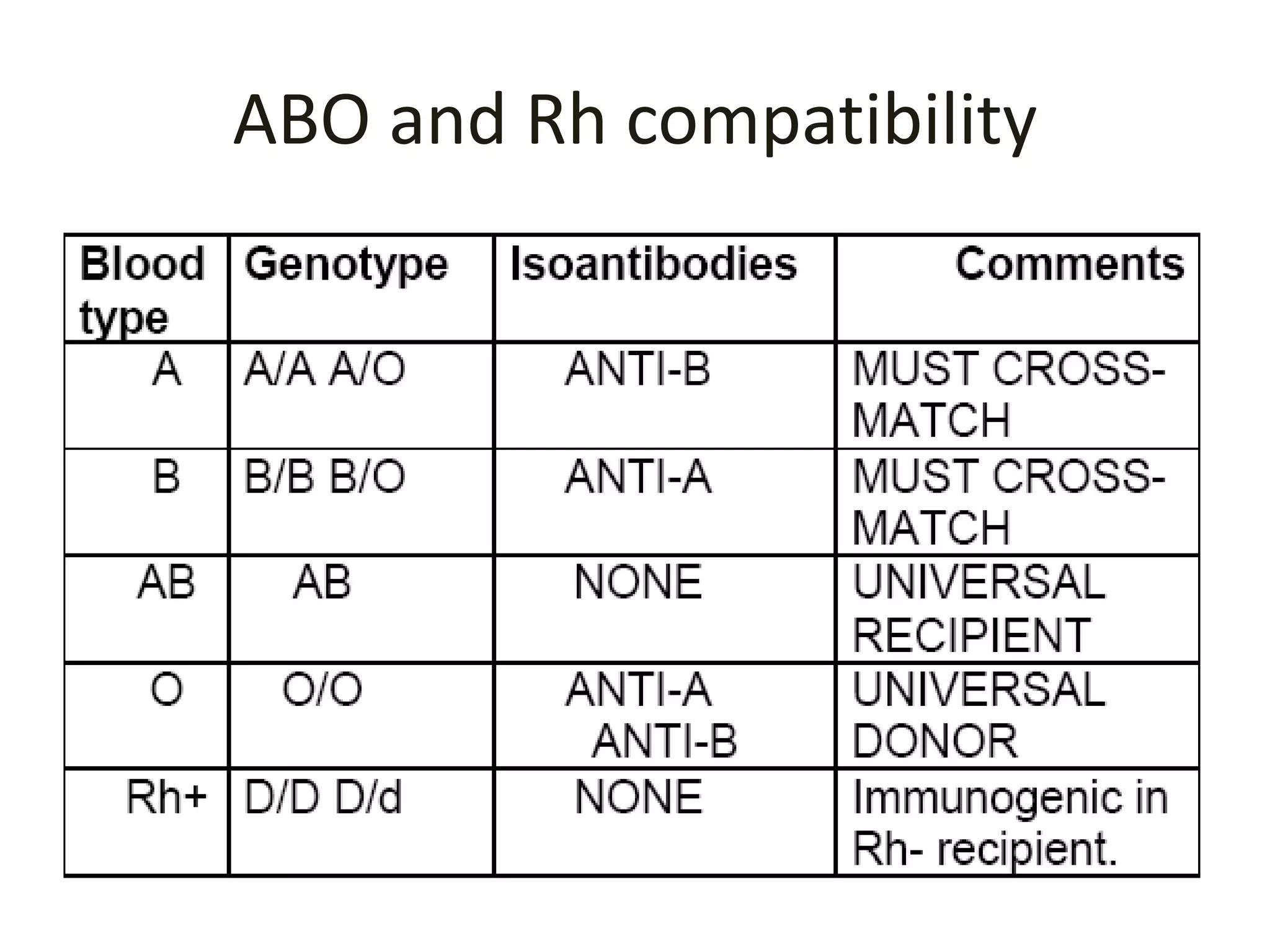
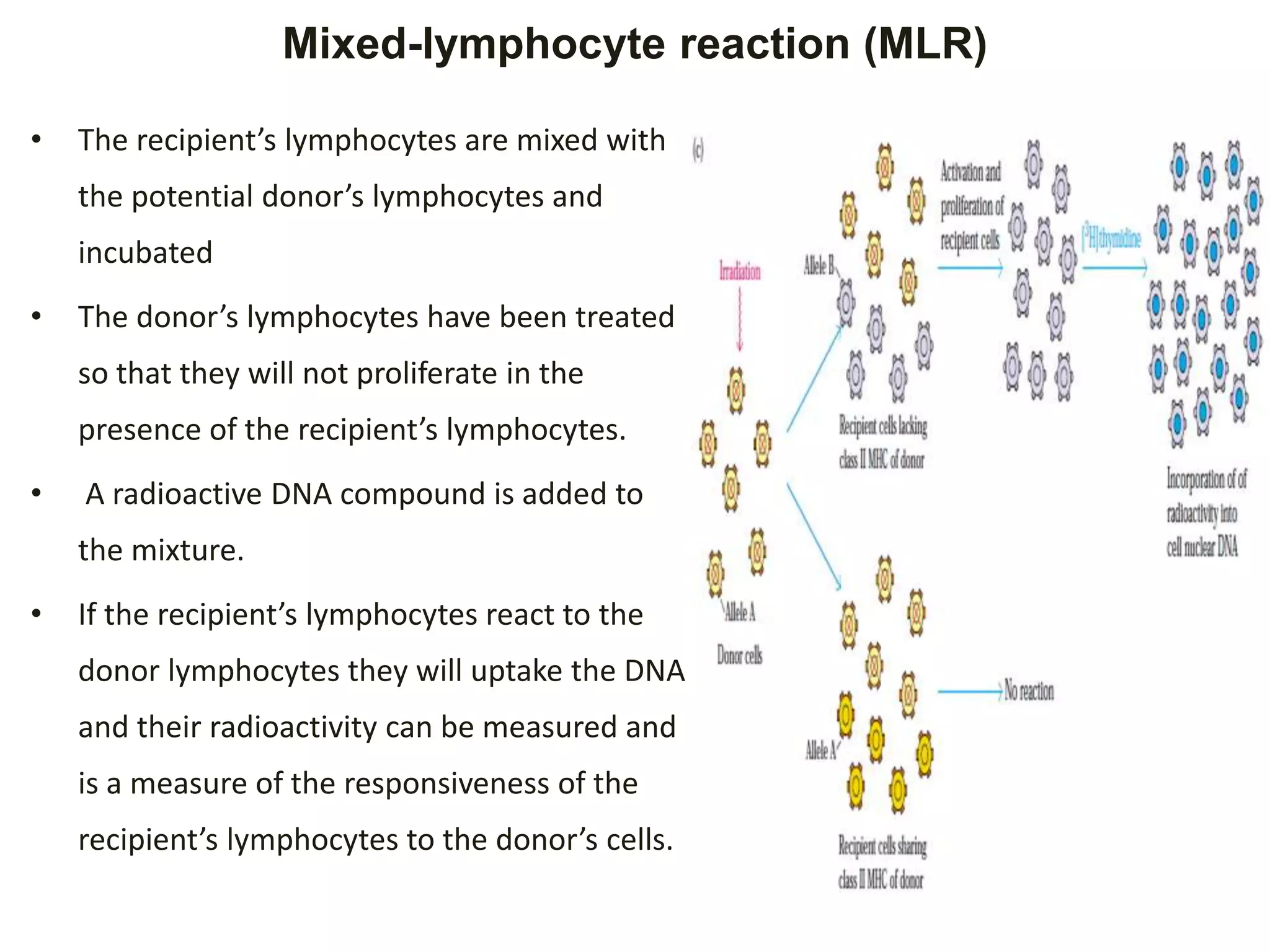
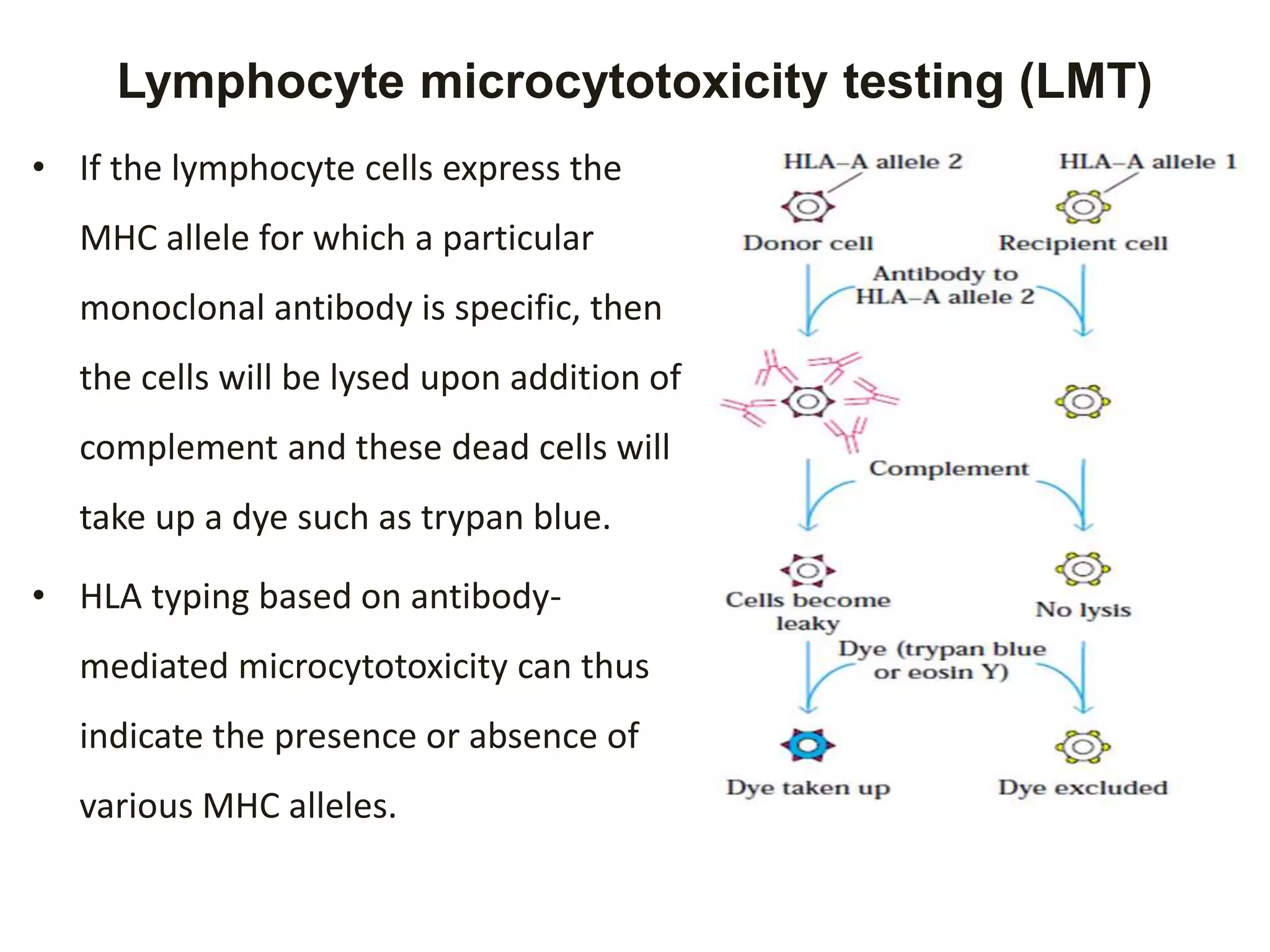
The adaptive immune system recognizes MHC molecules on donor tissues and organs, inducing rejection. HLA typing and matching is important for transplantation. Methods for HLA typing include serological and molecular techniques. HLA is classified into class I (HLA-A, -B, -Cw) and class II (HLA-DR, -DQ, -DP, -DM, -DO). High resolution HLA typing is important for donor selection to minimize mismatches and rejection. Additional compatibility testing includes ABO blood grouping and cross-matching.