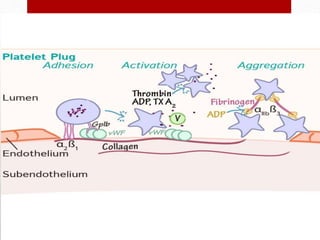
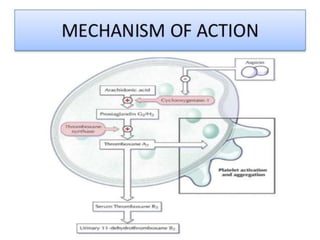
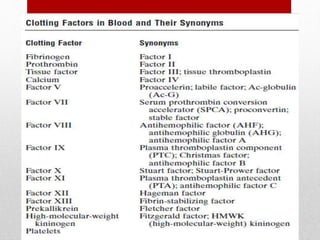
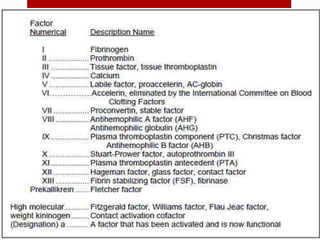
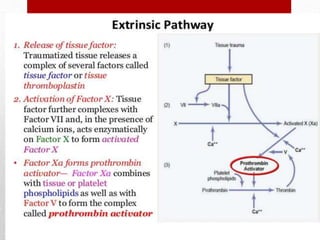
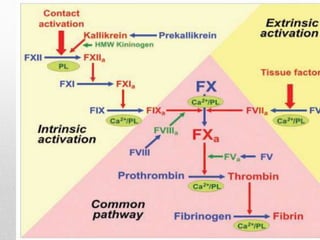
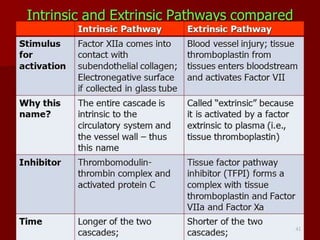
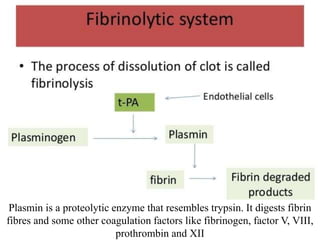
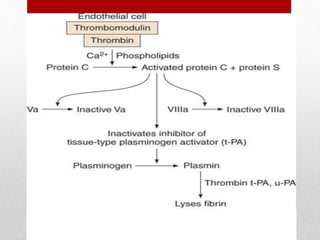
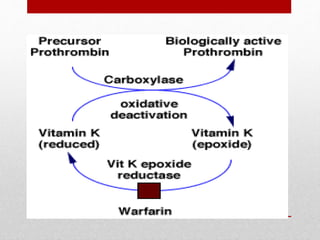
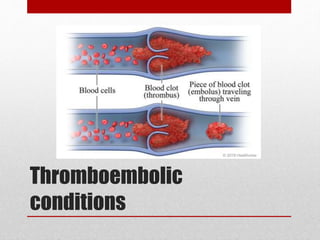
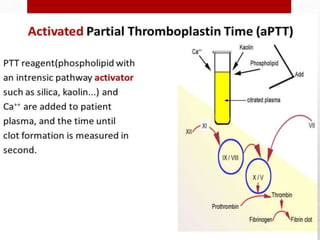
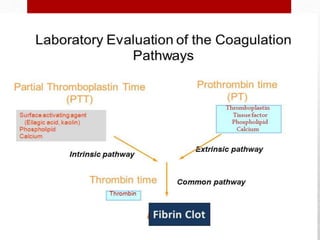
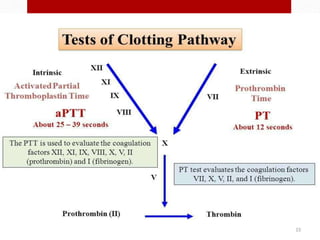
Hemostasis is the process by which bleeding is stopped. It involves four main steps: vascular constriction, formation of a platelet plug, formation of a blood clot, and fibrous organization of the clot. Platelets play a key role by adhering to damaged blood vessels, becoming activated, aggregating, and releasing chemicals that promote clot formation such as ADP and thromboxane A. Deficiencies in clotting factors such as vitamins K or factors VIII and IX can cause bleeding disorders. Thrombocytopenia is a low platelet count that increases bleeding risk. Thromboembolic conditions occur when clots form inside blood vessels and can cause issues like heart attacks, strokes,