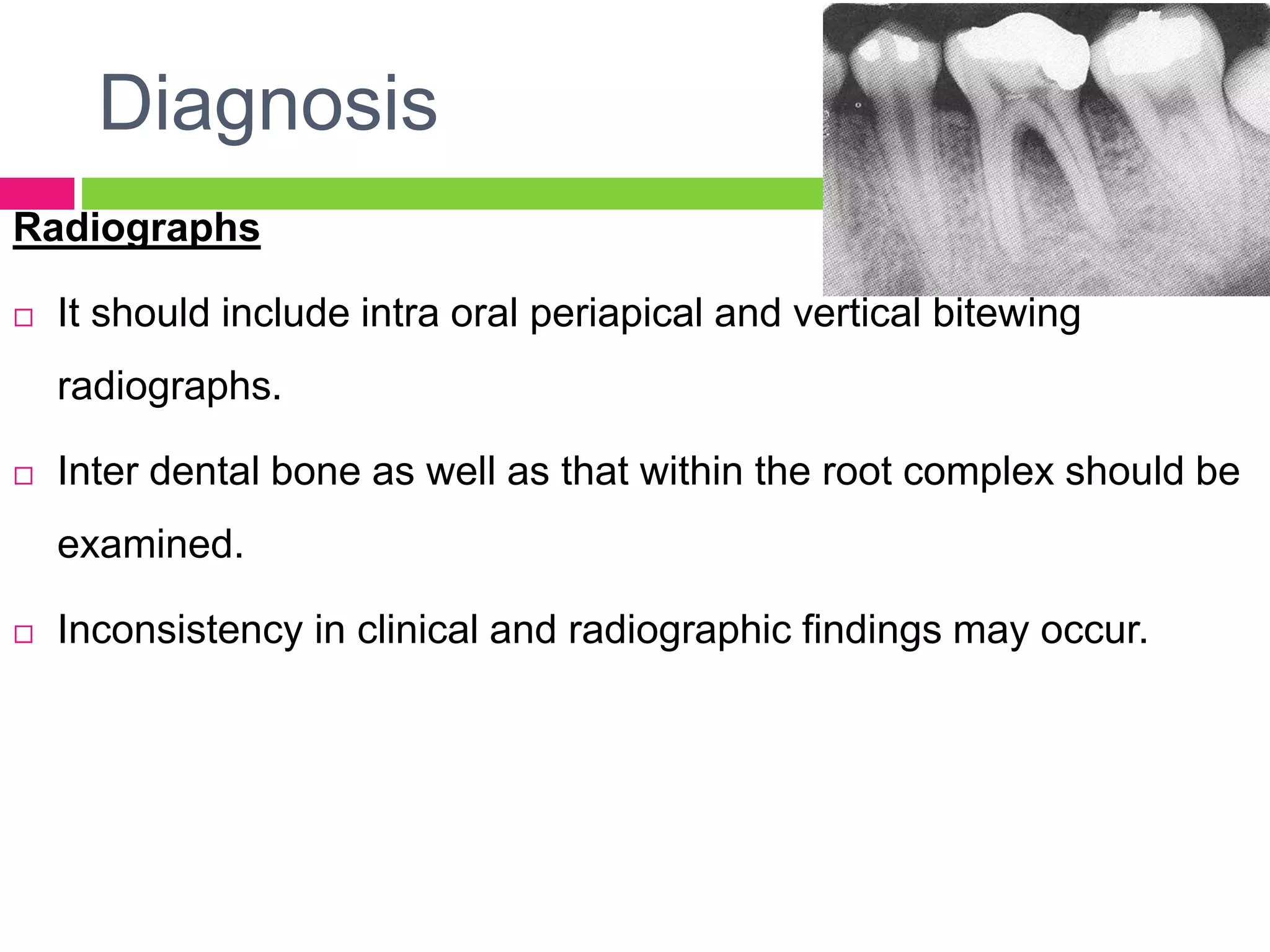
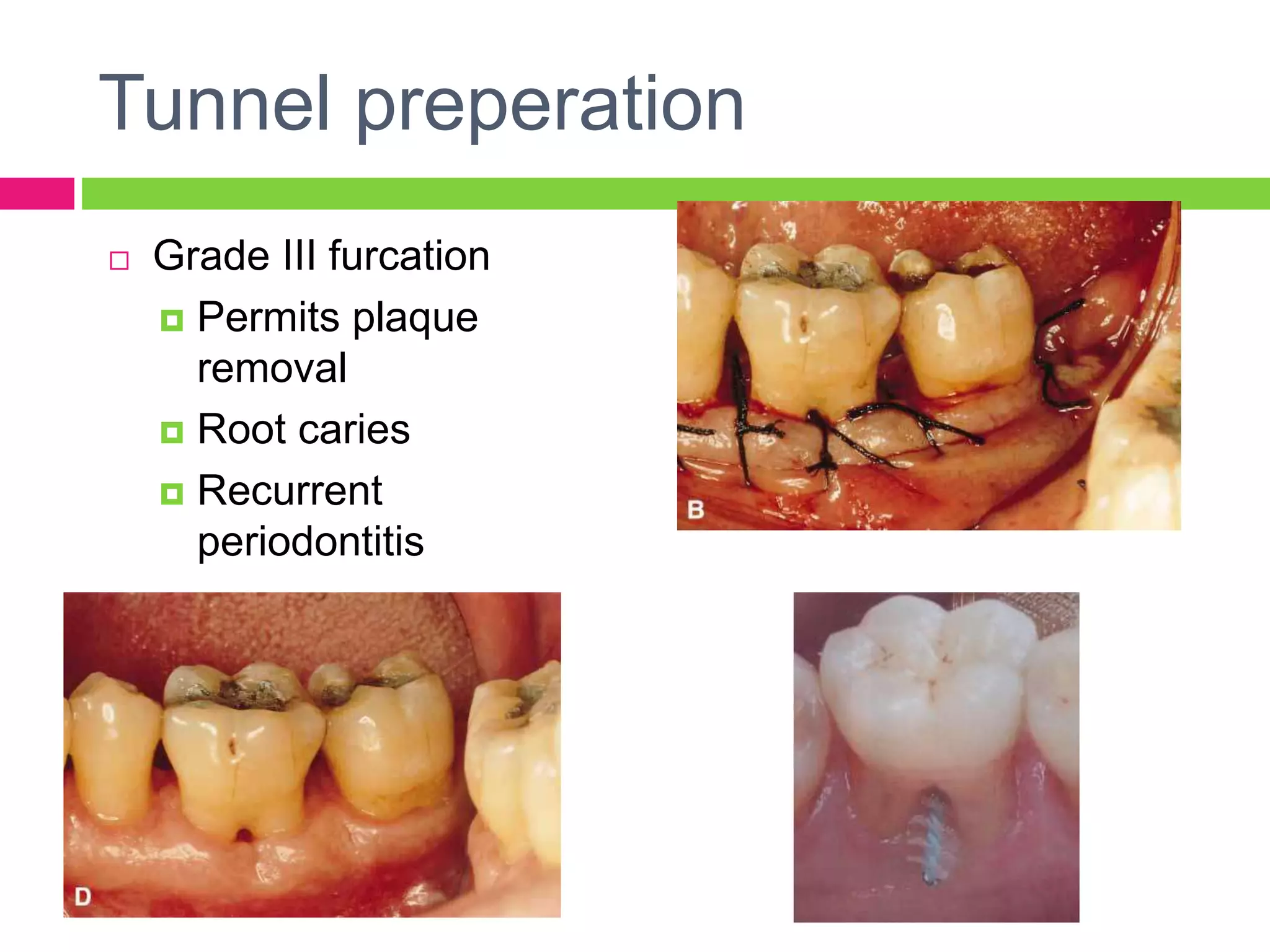
This document discusses furcation involvement in multi-rooted teeth. It begins with definitions of anatomical terms related to furcations. It then discusses various classifications of furcation involvement, ranging from initial/incipient involvement to more advanced through-and-through defects. Epidemiology, etiology, diagnosis and factors affecting treatment outcomes are also covered. The document concludes with an overview of management approaches, which include maintaining the furcation, increasing access, removing the furcation, or closing it with new attachment.