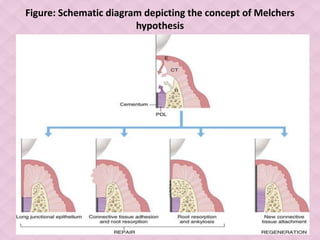
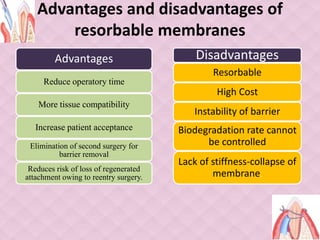
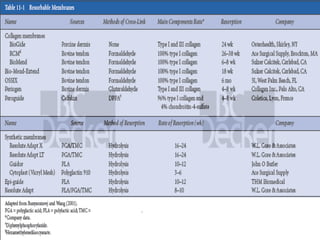
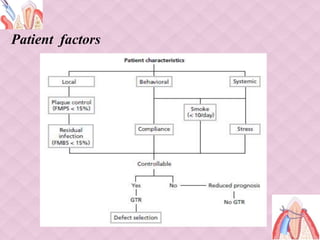
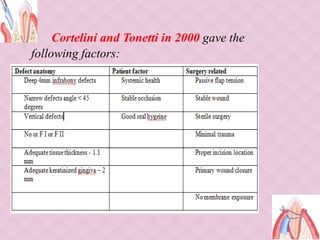
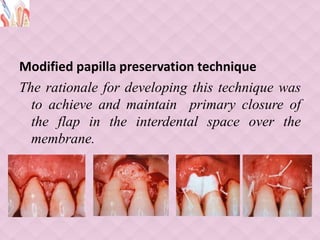
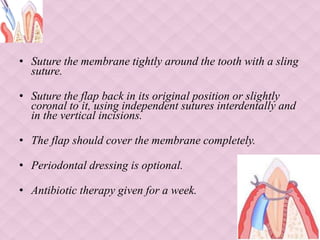
This document provides an overview of guided tissue regeneration (GTR). It begins with definitions of periodontal regeneration and GTR. It then discusses the history and development of GTR from the 1970s onwards. The core concept of GTR is explained, which is based on Melcher's hypothesis that only periodontal ligament cells can regenerate the periodontal attachment apparatus. Indications, contraindications, design criteria and objectives of GTR barriers are covered. The document classifies and compares advantages and disadvantages of absorbable versus non-absorbable membranes. Key factors affecting GTR outcomes are discussed. Surgical techniques and the healing of GTR-treated defects are described. The document concludes with additional considerations like complications and the