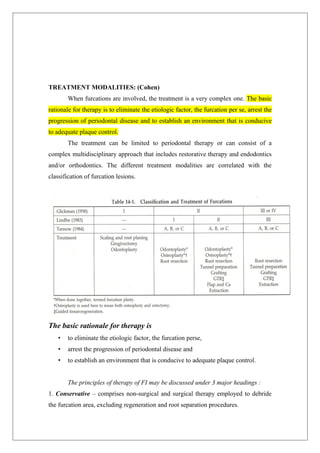
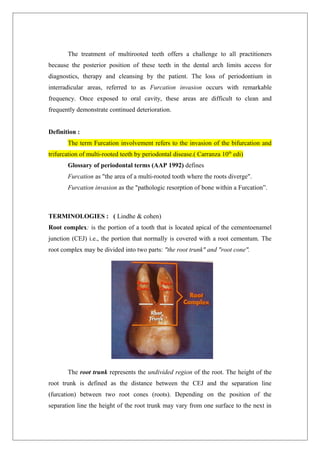
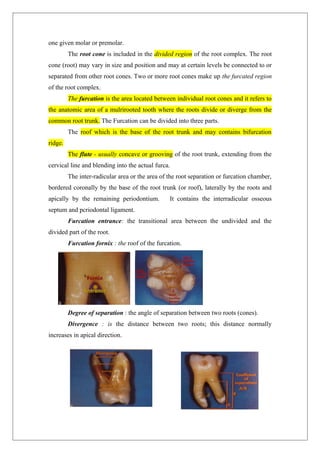
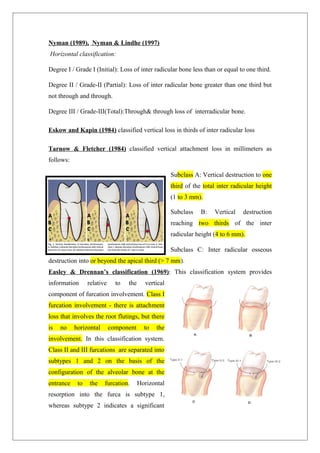
This document provides information about furcation involvement, which refers to the invasion of the bifurcation or trifurcation areas of multi-rooted teeth by periodontal disease. It discusses the anatomy and morphology of root complexes, classifications of furcation involvement, and methods for diagnosis, including clinical examination, radiographic examination, and intraoperative measurements. The document also covers etiology, pathogenesis, differential diagnosis, treatment modalities, and prognosis.