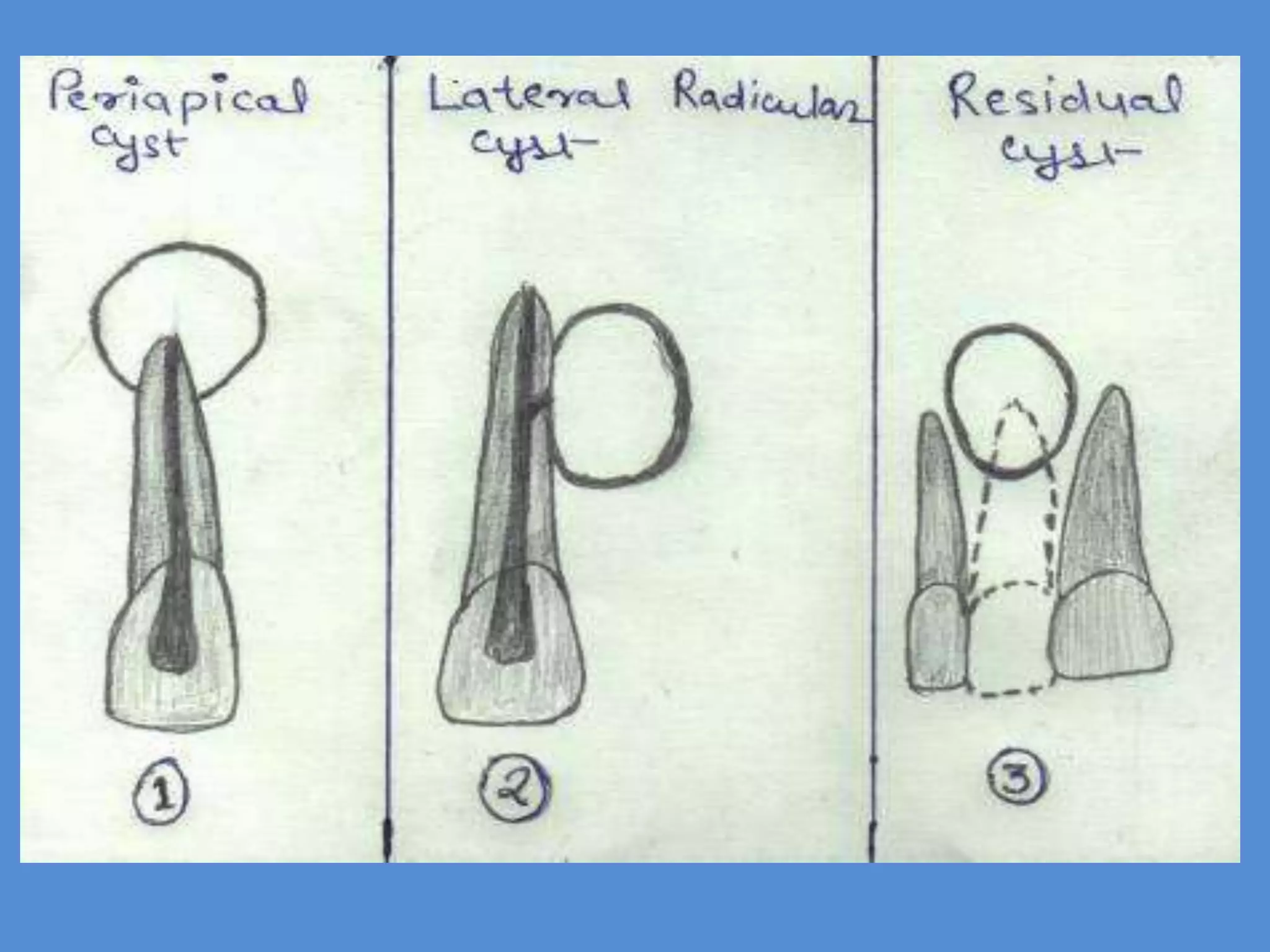
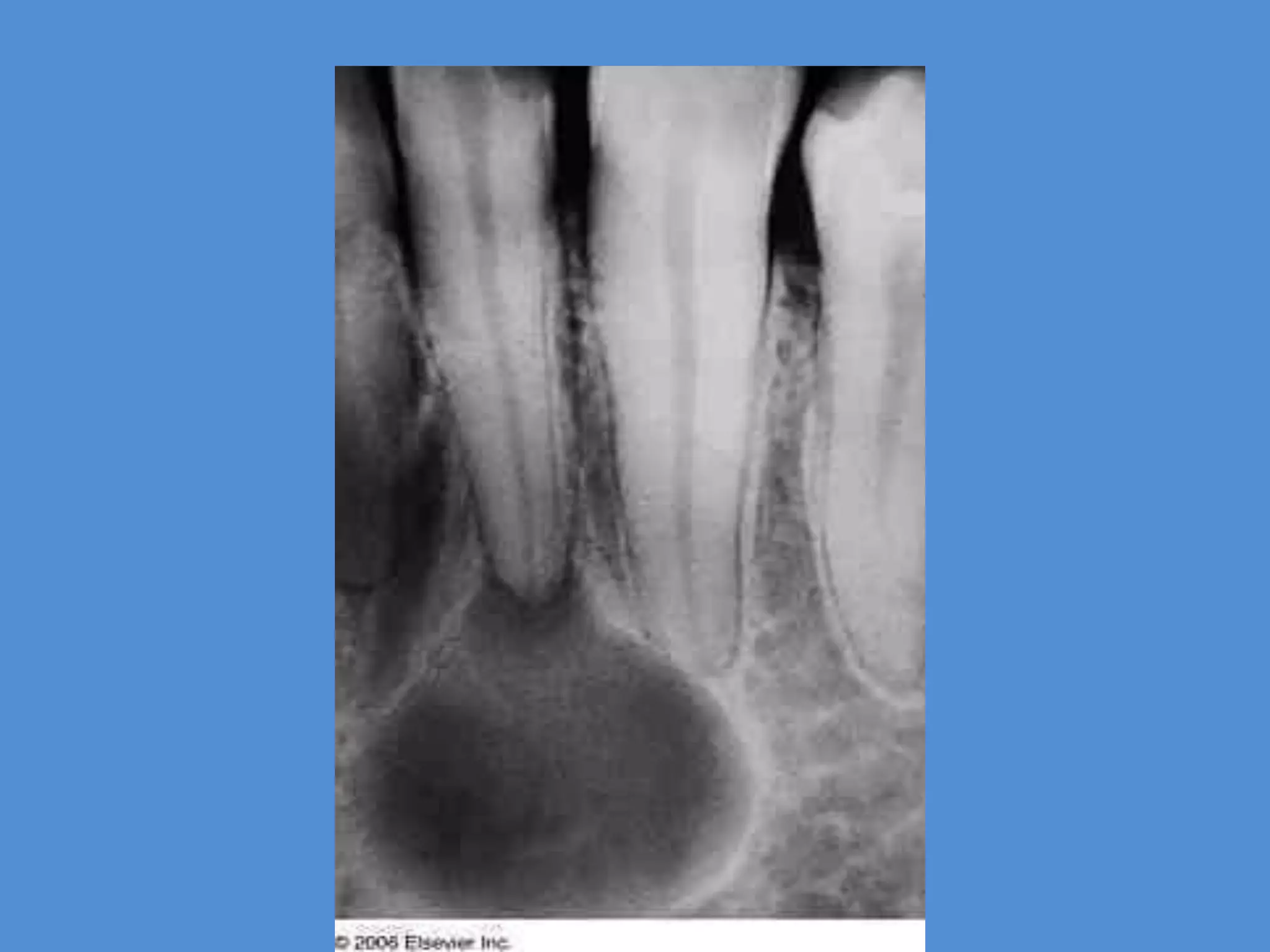
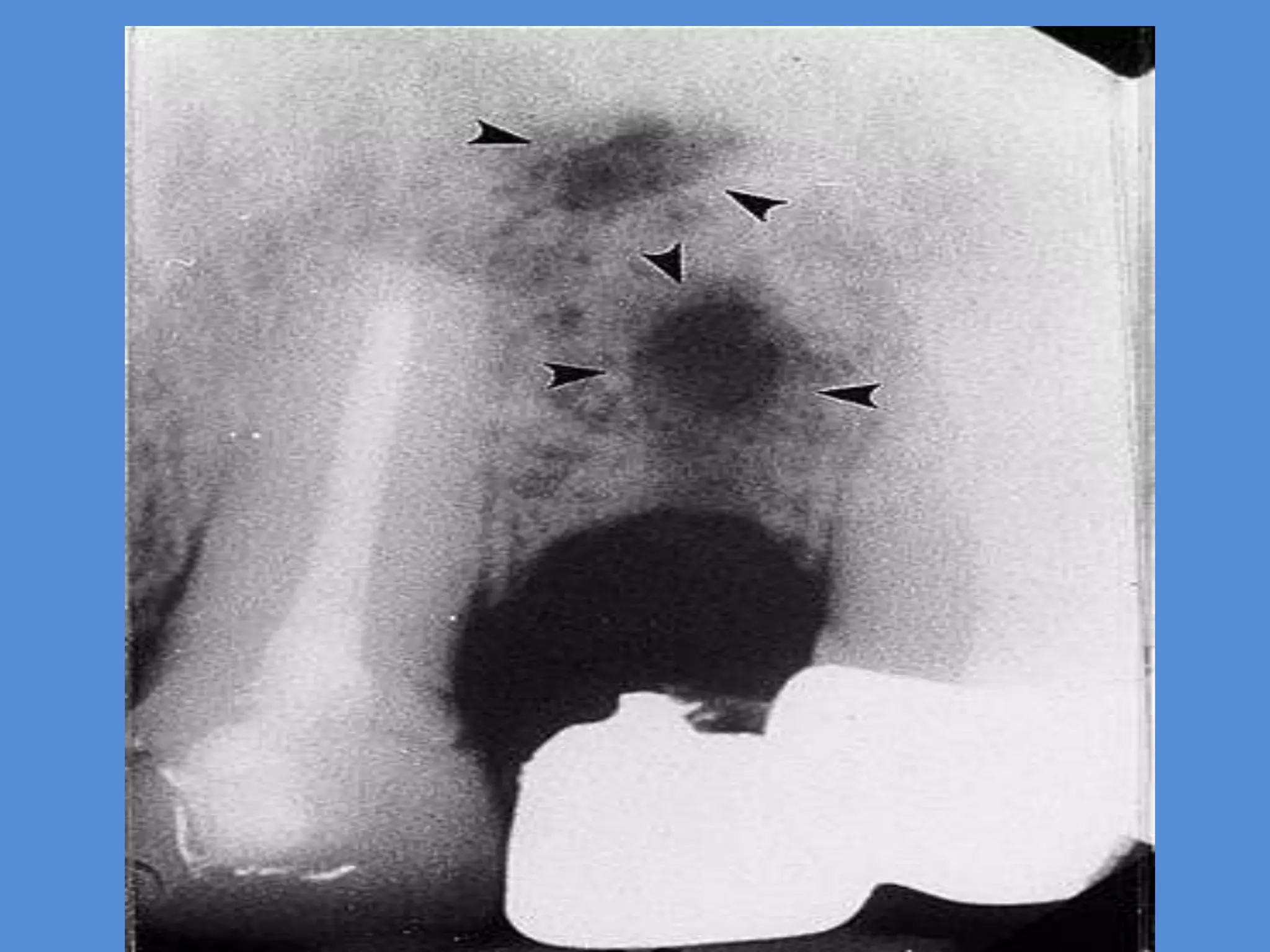
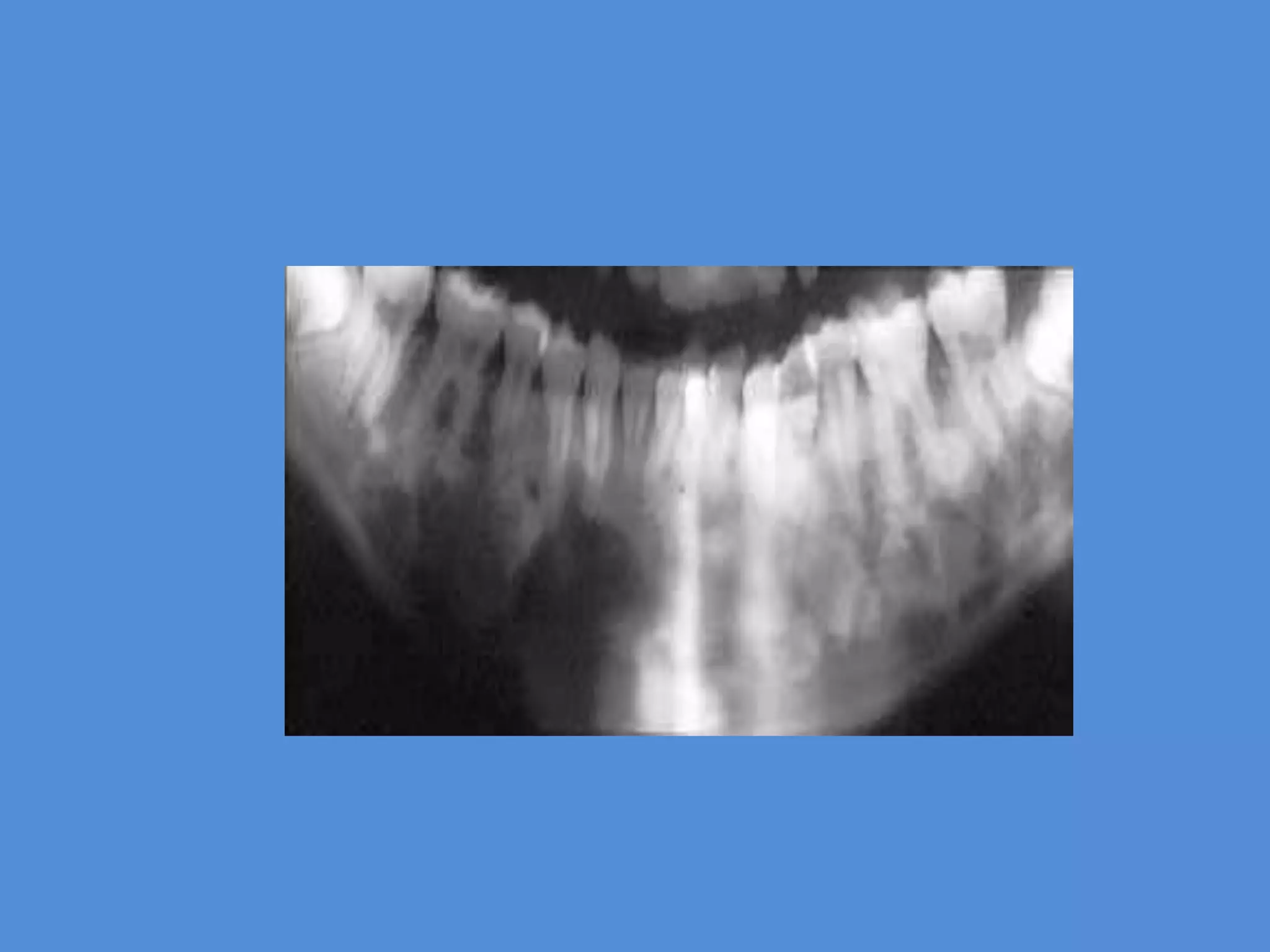
This document discusses the differential diagnosis of periapical radiolucencies. It describes true periapical radiolucencies such as pulpo-periapical radiolucencies, dentigerous cysts, periapical cemento-osseous dysplasias and malignant tumors. It also discusses pseudo-periapical radiolucencies caused by anatomical variations. Different pathological conditions are described including their etiology, clinical features, radiographic features, differential diagnosis and management.









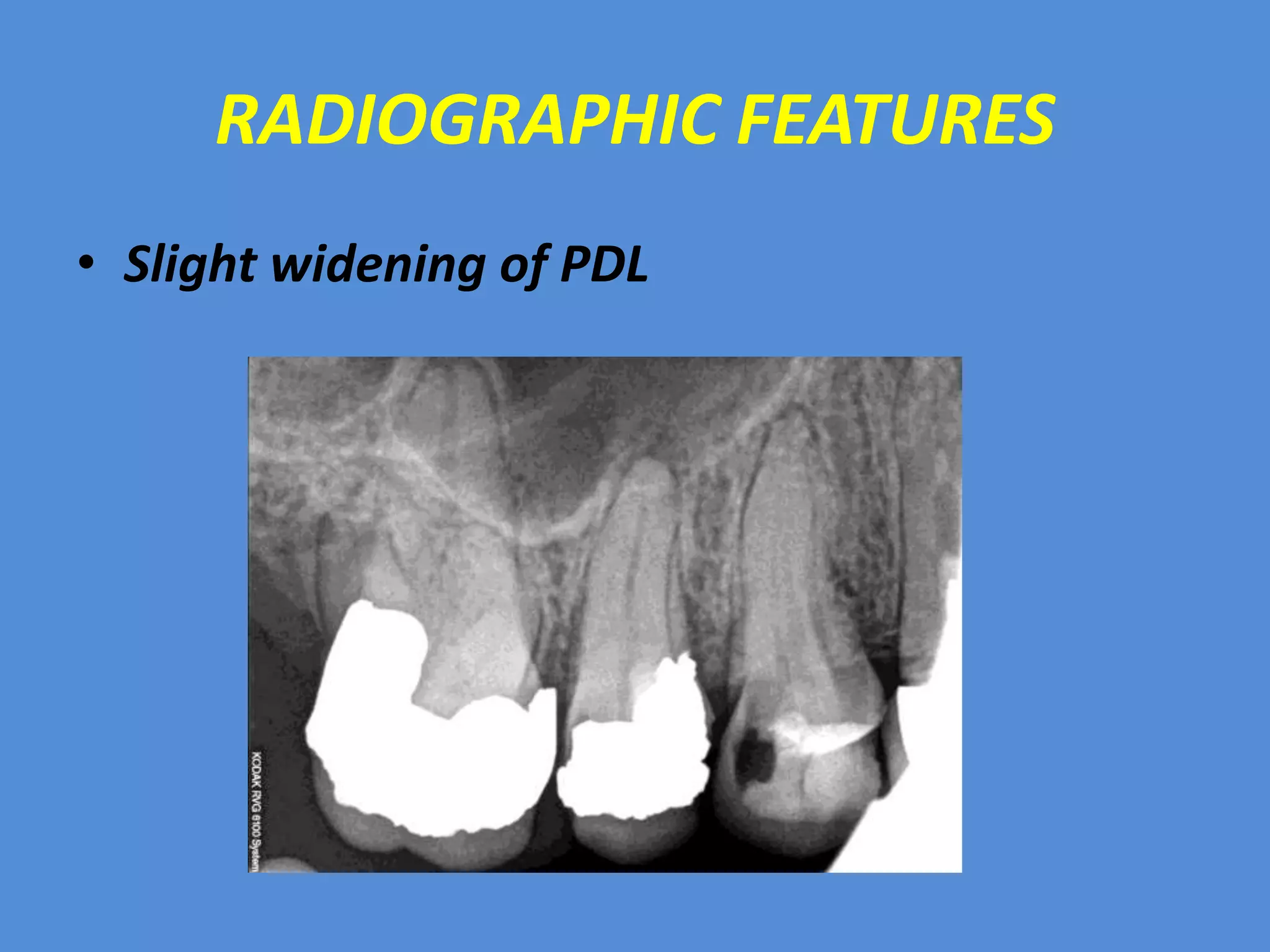
![ACUTE APICAL
PERIODONTITIS
• Definition:-Acute apical periodontitis is a painful inflammation of
periodontium as a result of trauma, irritation [or] infection through root
canal regardless of whether pulp is vital or non-vital.
• ETIOLOGY:-
In a vital tooth:
Occlusal trauma
Wedging of foreign object b/w the teeth
Blow to the teeth](https://image.slidesharecdn.com/differentialdiagnosisforperiapicalradiolucency-220812093807-3ac10d1f/75/DIFFERENTIAL-DIAGNOSIS-FOR-PERIAPICAL-RADIOLUCENCY-pptx-11-2048.jpg)