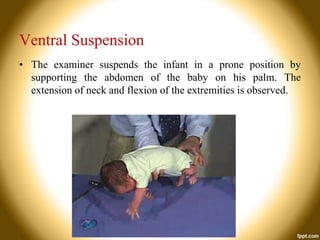
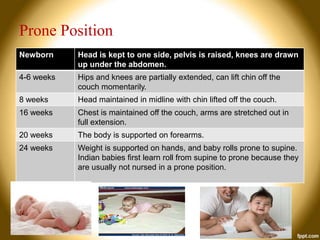
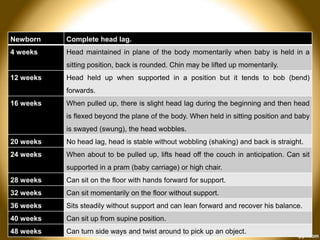
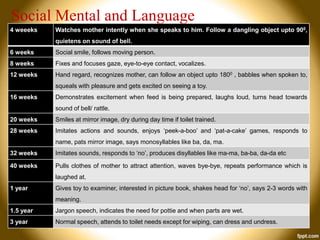
This document provides an overview of developmental assessment for children. It discusses the goal of developmental assessment as generating a diagnosis and analyzing strengths and weaknesses to direct treatment. It also covers principles of development, value of assessment, common assessment tools, domains of development, developmental milestones, and risk factors. The document aims to guide healthcare providers in conducting developmental assessments and identifying potential developmental delays.