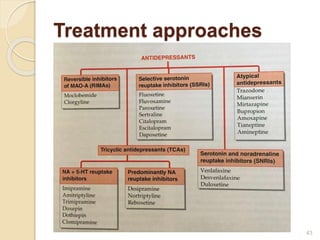
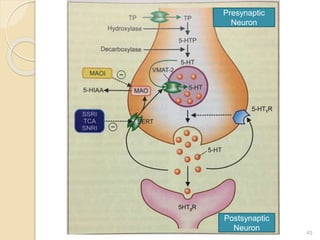
The document discusses various aspects of depression including its history, types, symptoms, diagnosis, prevalence, and treatment options. It highlights the significant impact of depression worldwide, noting that over 264 million people suffer from it, and details different forms such as Major Depressive Disorder and Bipolar Depression. Additionally, it addresses causes ranging from genetic to environmental factors, and emphasizes the importance of proper diagnosis and treatment to manage the disorder effectively.