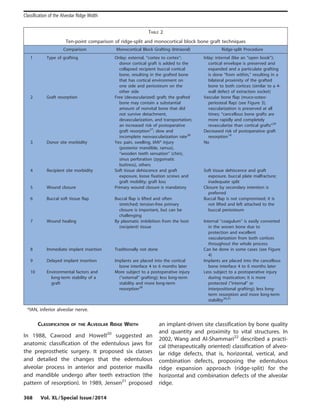
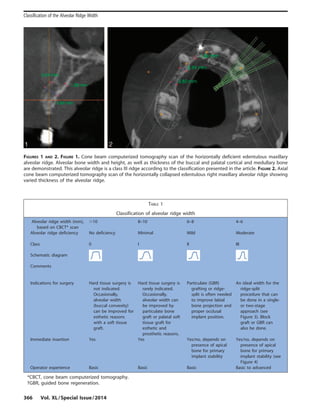
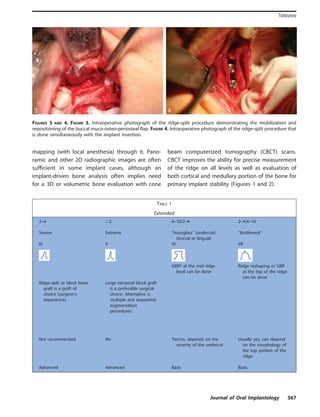
The document discusses treatment strategies for horizontally deficient alveolar ridges, focusing on the ridge-split approach and proposing a clinically relevant implant-driven classification system for alveolar ridge width. It compares the advantages of ridge-split and block bone graft techniques for addressing horizontal bone loss before or during dental implant placement. The classification aims to guide practitioners in selecting appropriate surgical methods based on the specific ridge morphology and operator experience.