The document provides information on chemotherapy administration including:
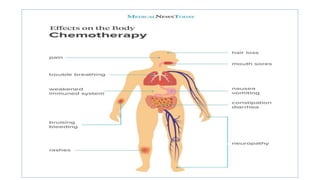
1. Chemotherapy involves using drugs to destroy cancer cells by interfering with cellular functions and reproduction.
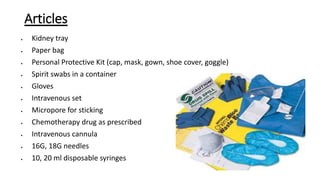
2. Personal protective equipment like gloves, gowns, and masks should be worn when handling chemotherapeutic agents.
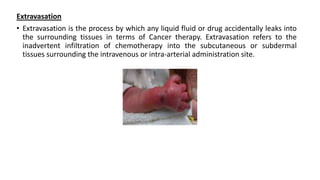
3. The administration process involves preparing medications, inserting IV lines, monitoring for side effects like extravasation during infusion, and documenting the procedure. Management of extravasation or spills should also be followed.