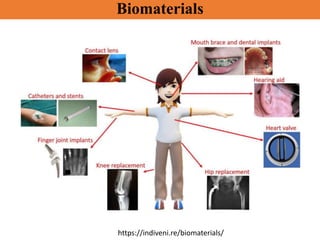
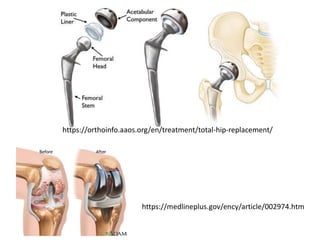
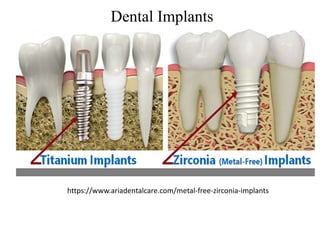
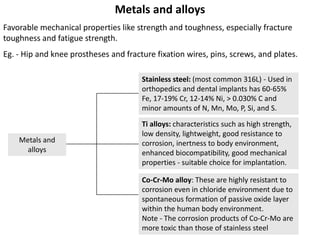
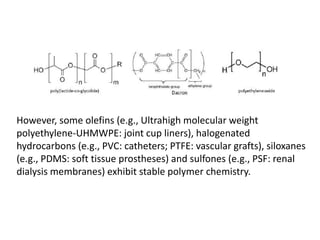
Biomaterials are any materials used in medical devices and implants that interact with biological systems. They include metals, ceramics, polymers, and composites. Key requirements for biomaterials are biocompatibility, mechanical stability, and manufacturability. Metals are used for implants requiring strength while ceramics provide hardness and corrosion resistance but are brittle. Polymers are flexible with customizable properties but degrade over time. Composites mimic natural materials by combining materials like calcium phosphate ceramics and collagen to achieve optimized properties. Selection of biomaterials depends on the application and desired mechanical and biological interactions.