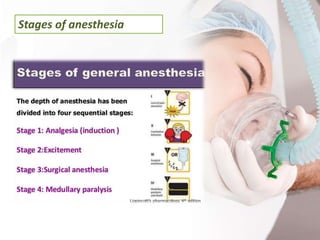
Anesthesia is utilized to manage pain during surgical procedures through various types such as general, regional, and local anesthesia. While risks exist, they are generally low for healthy individuals; complications can arise particularly from certain health conditions or factors like smoking and medication use. Stages of anesthesia progress from induction to surgical anesthesia, with potential severe outcomes in case of overdose.