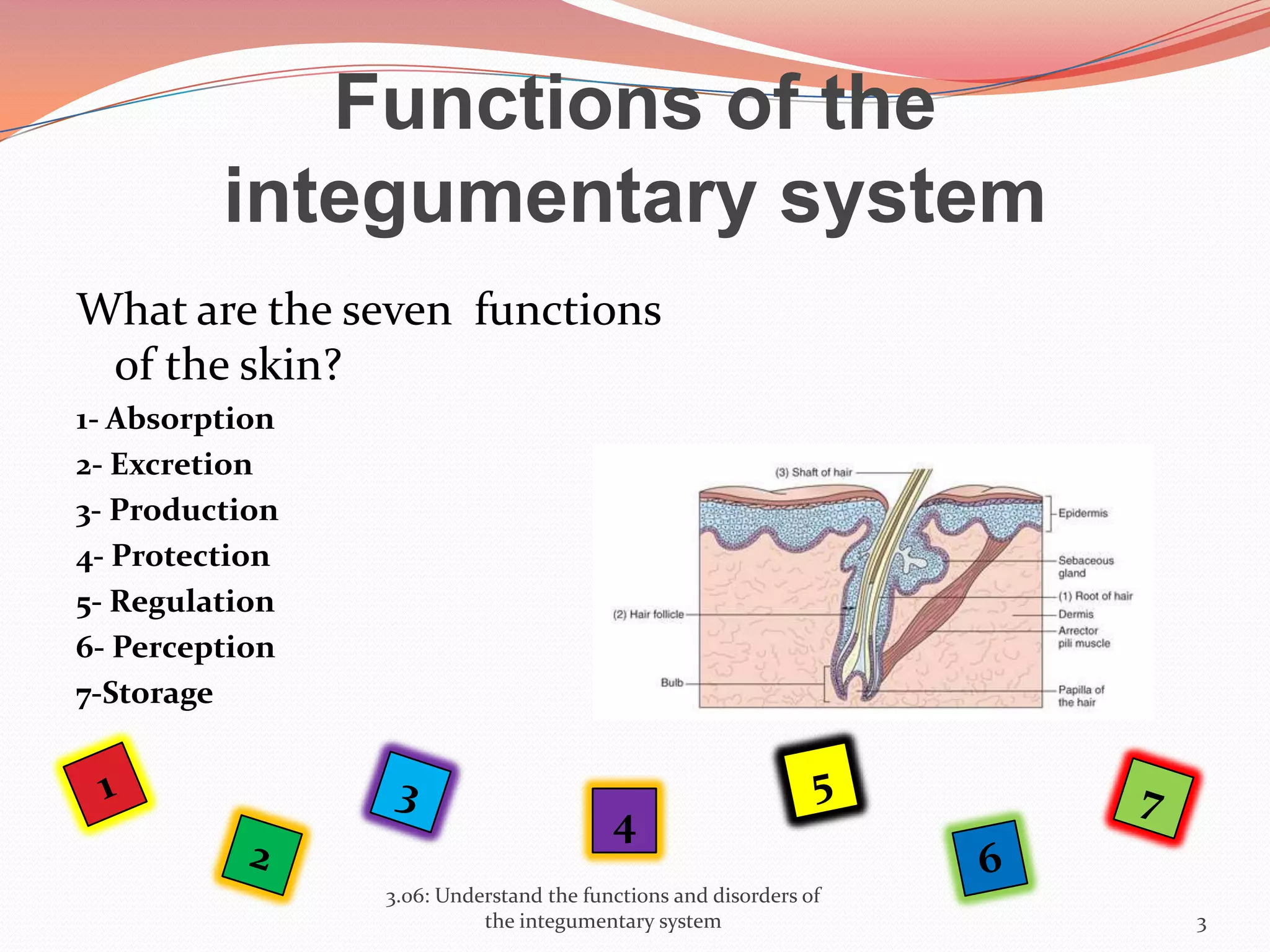
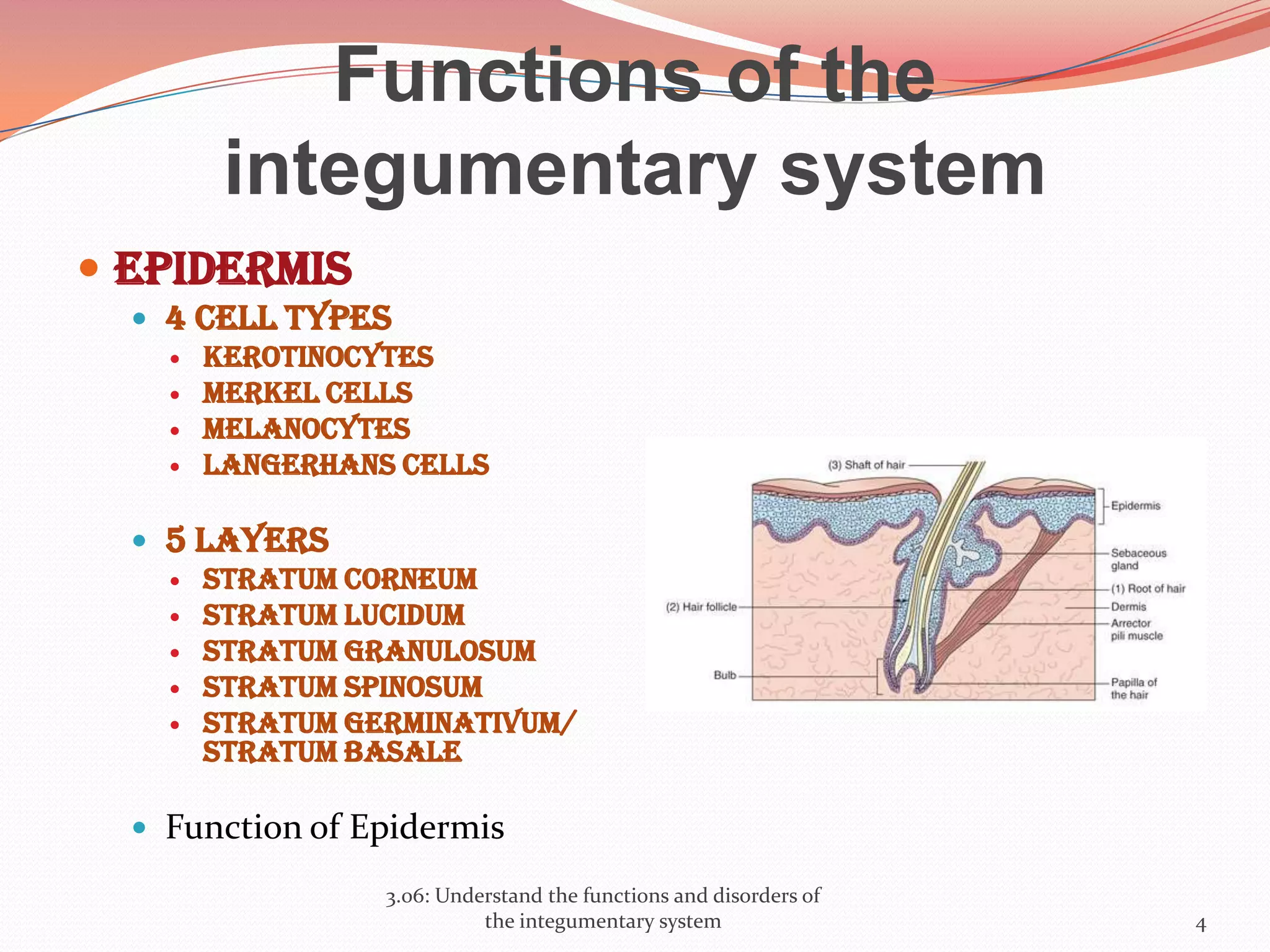
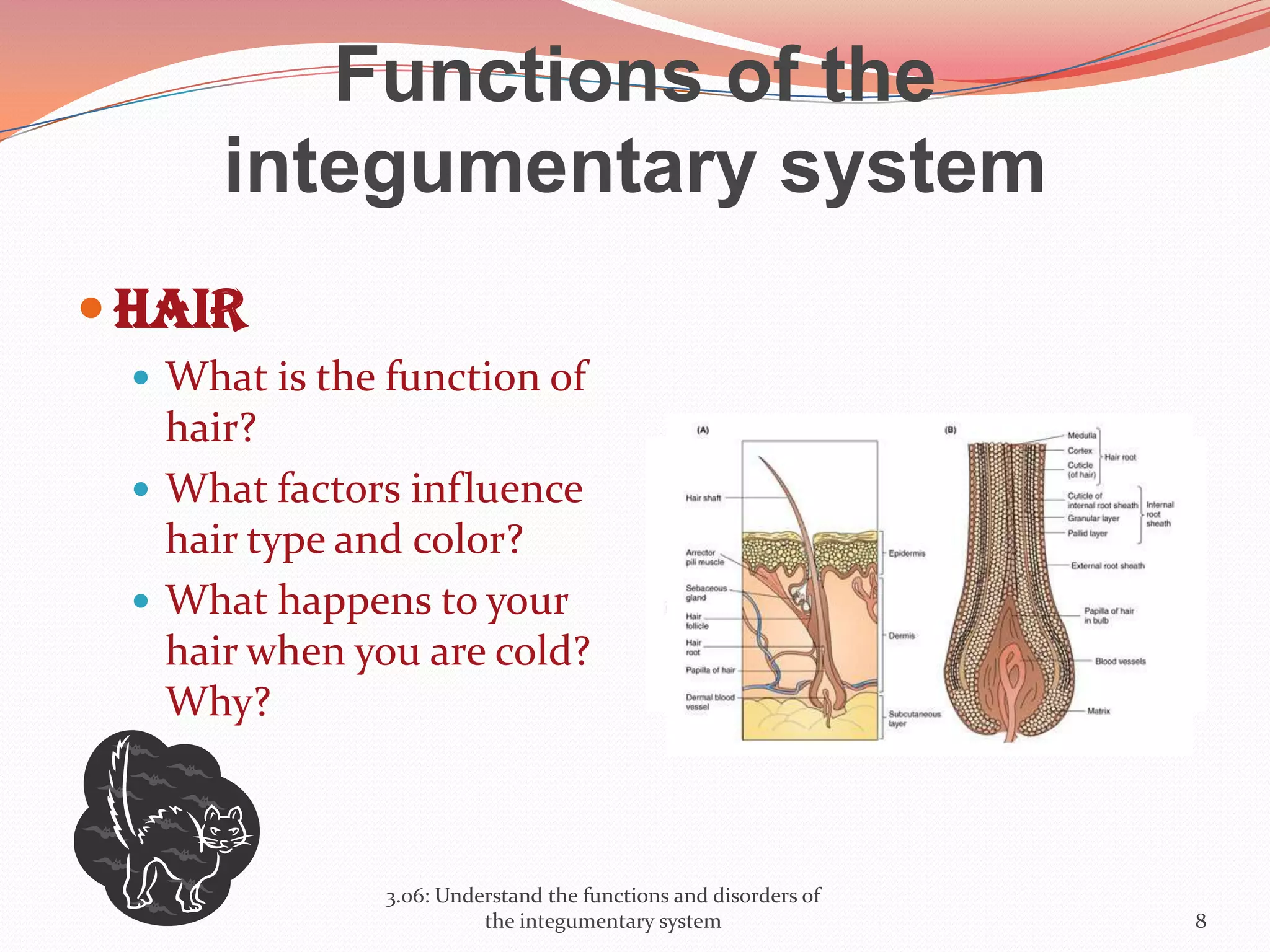
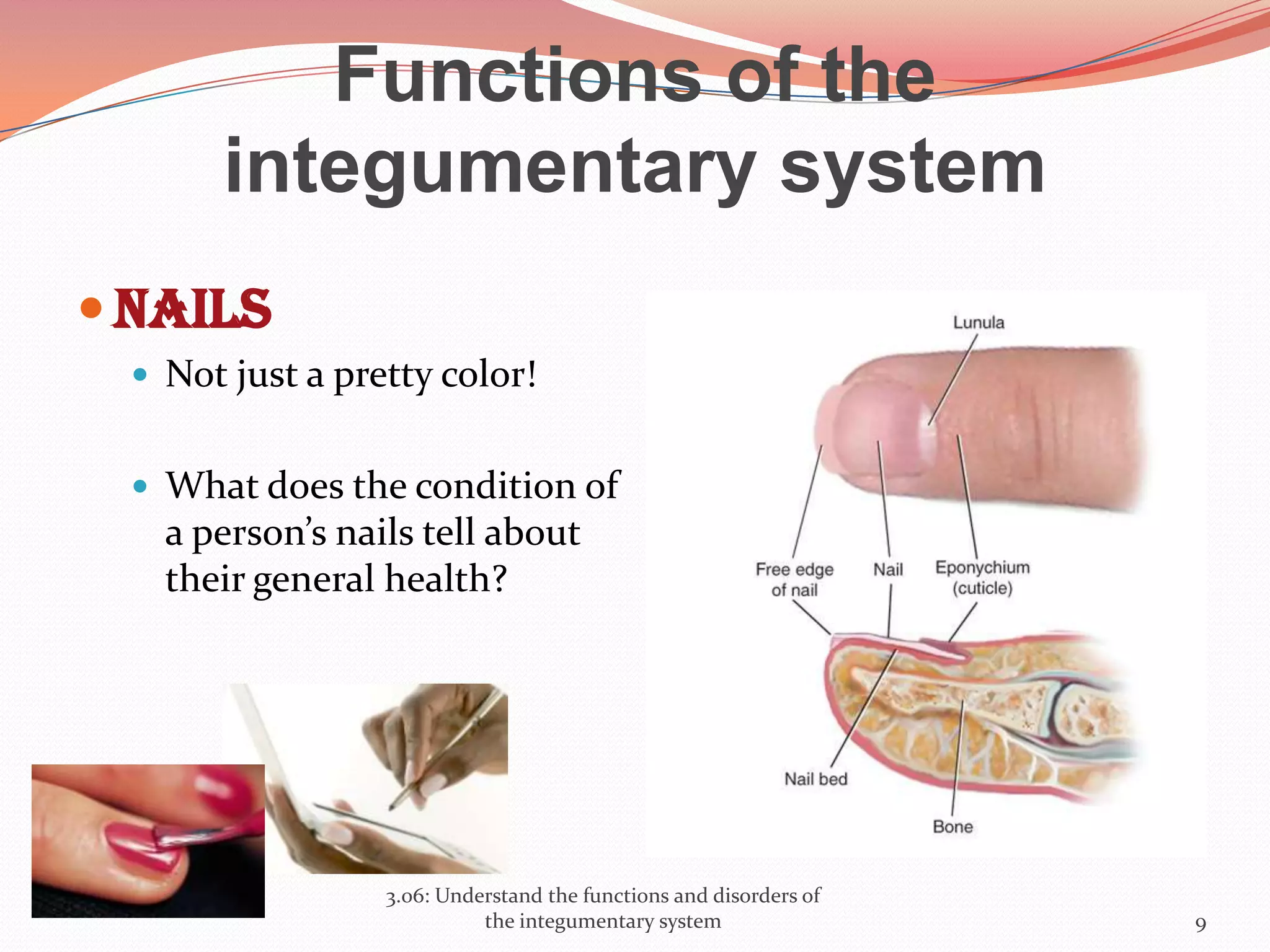
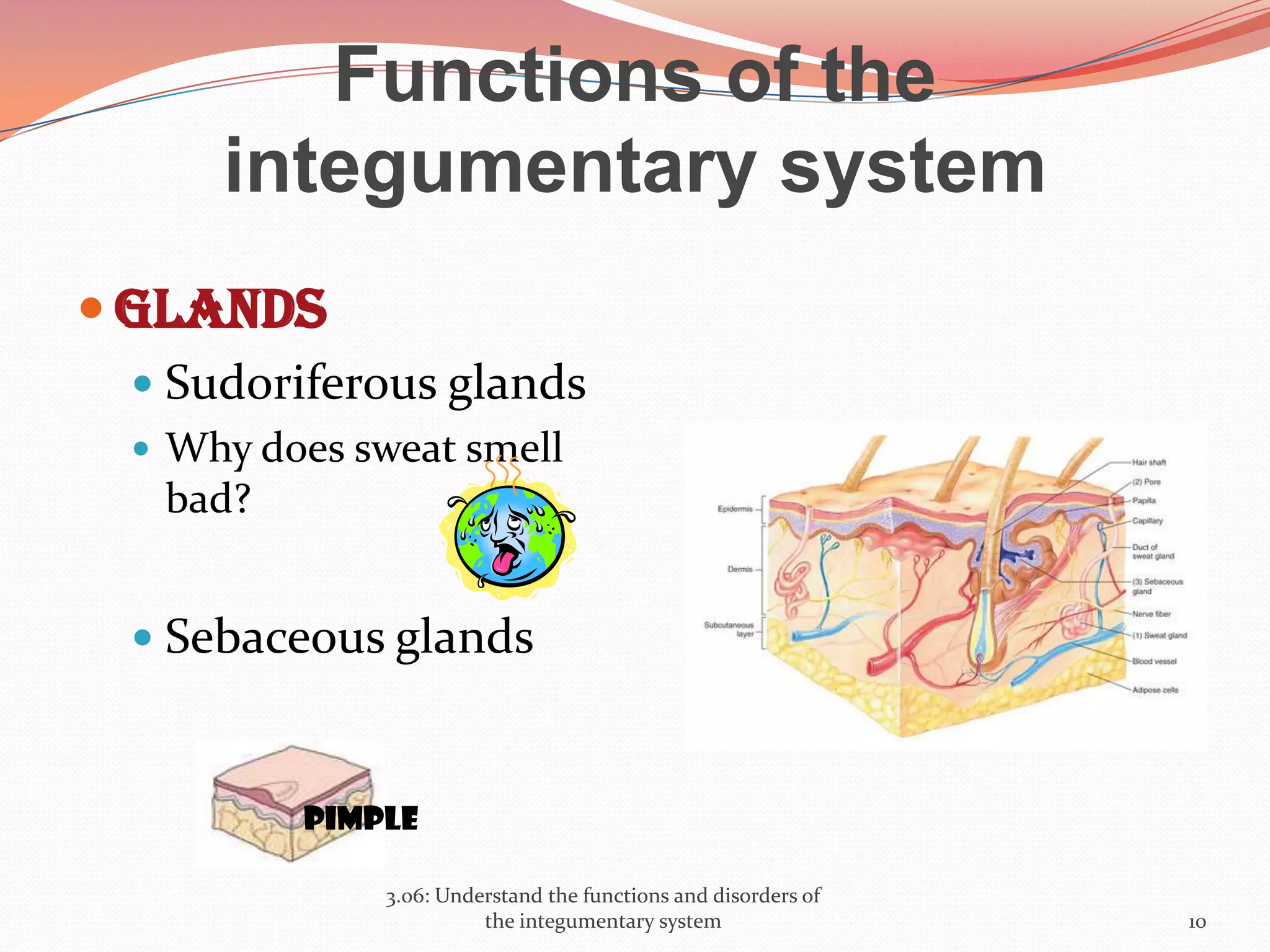
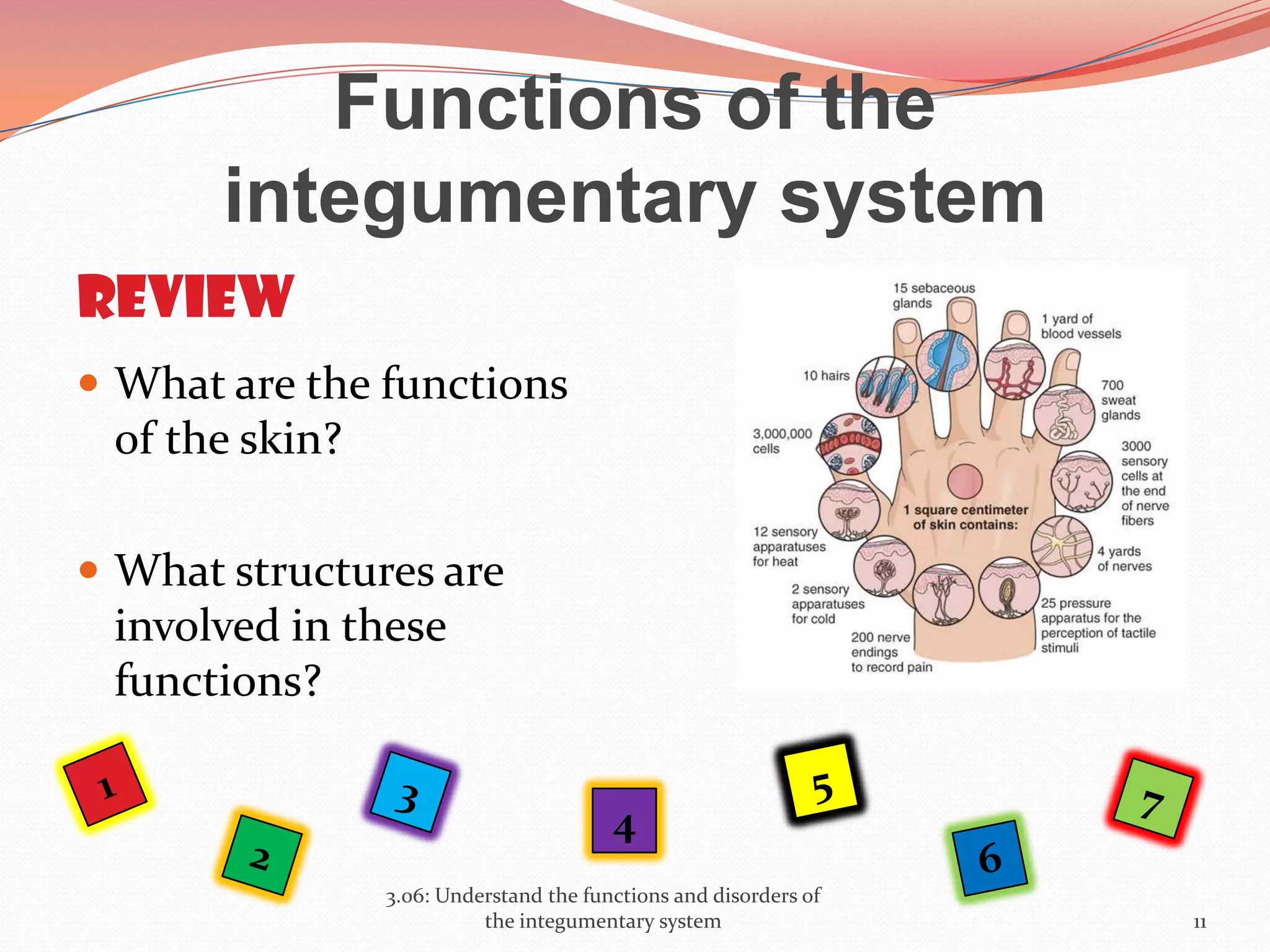
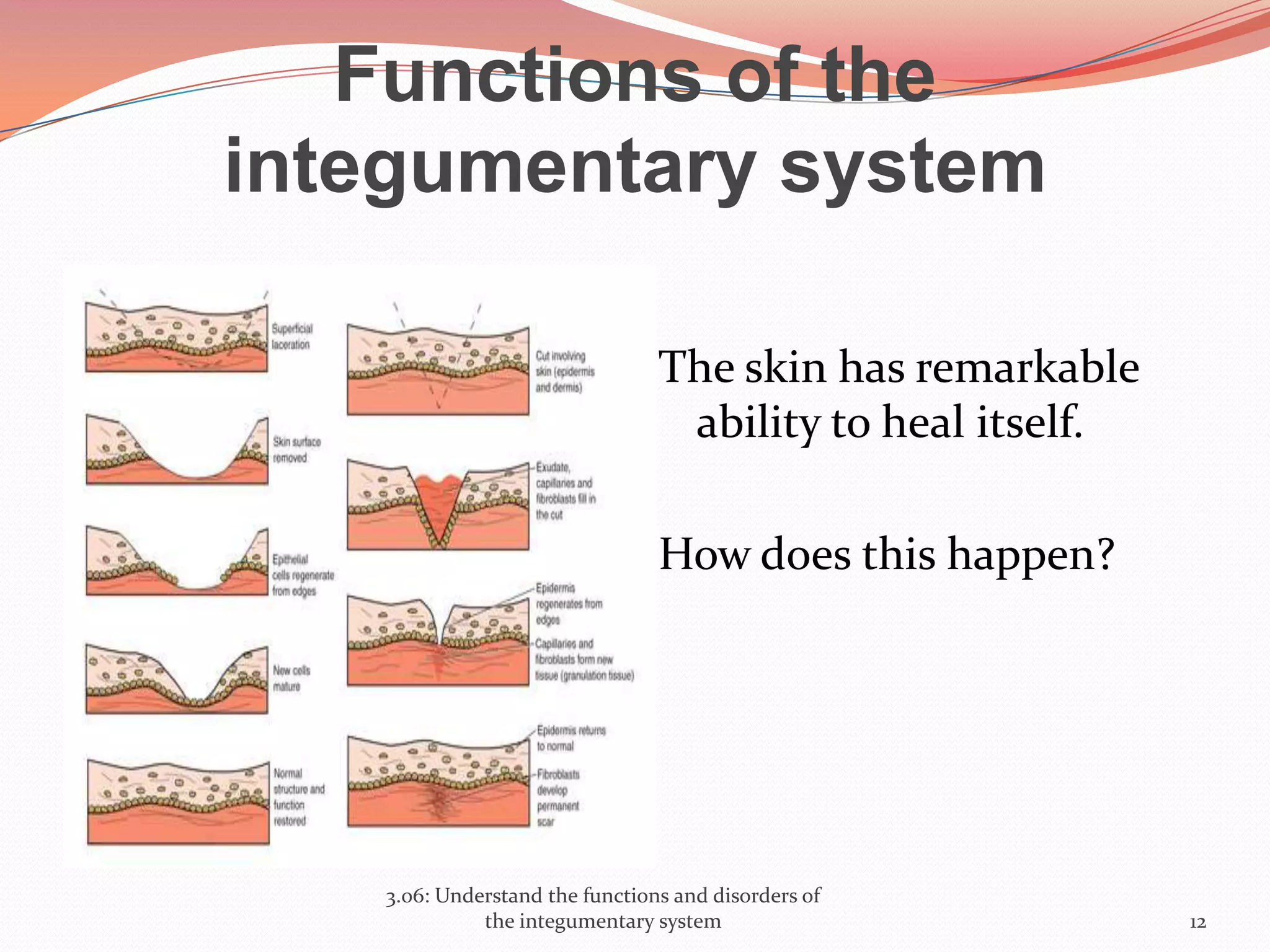
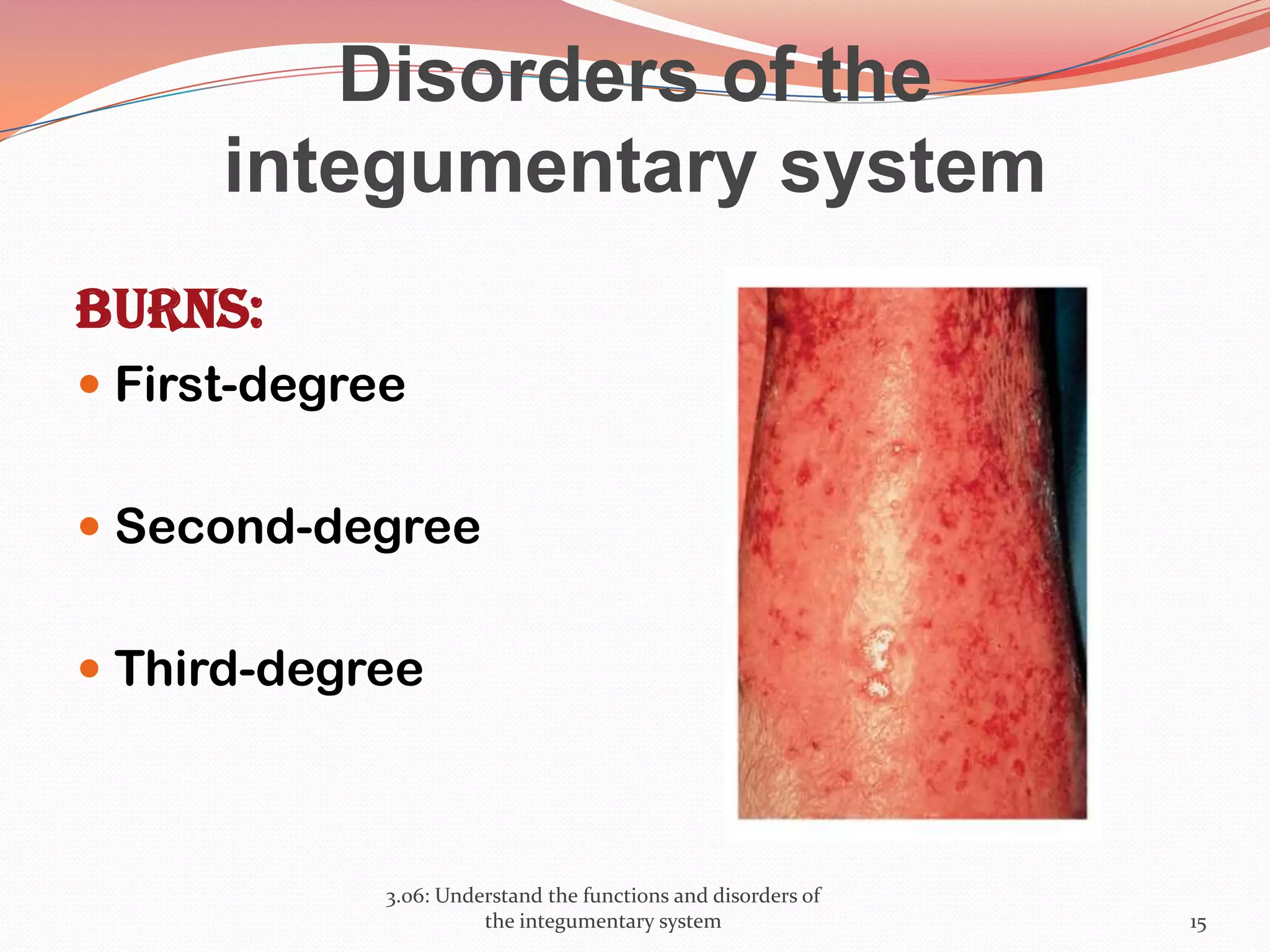
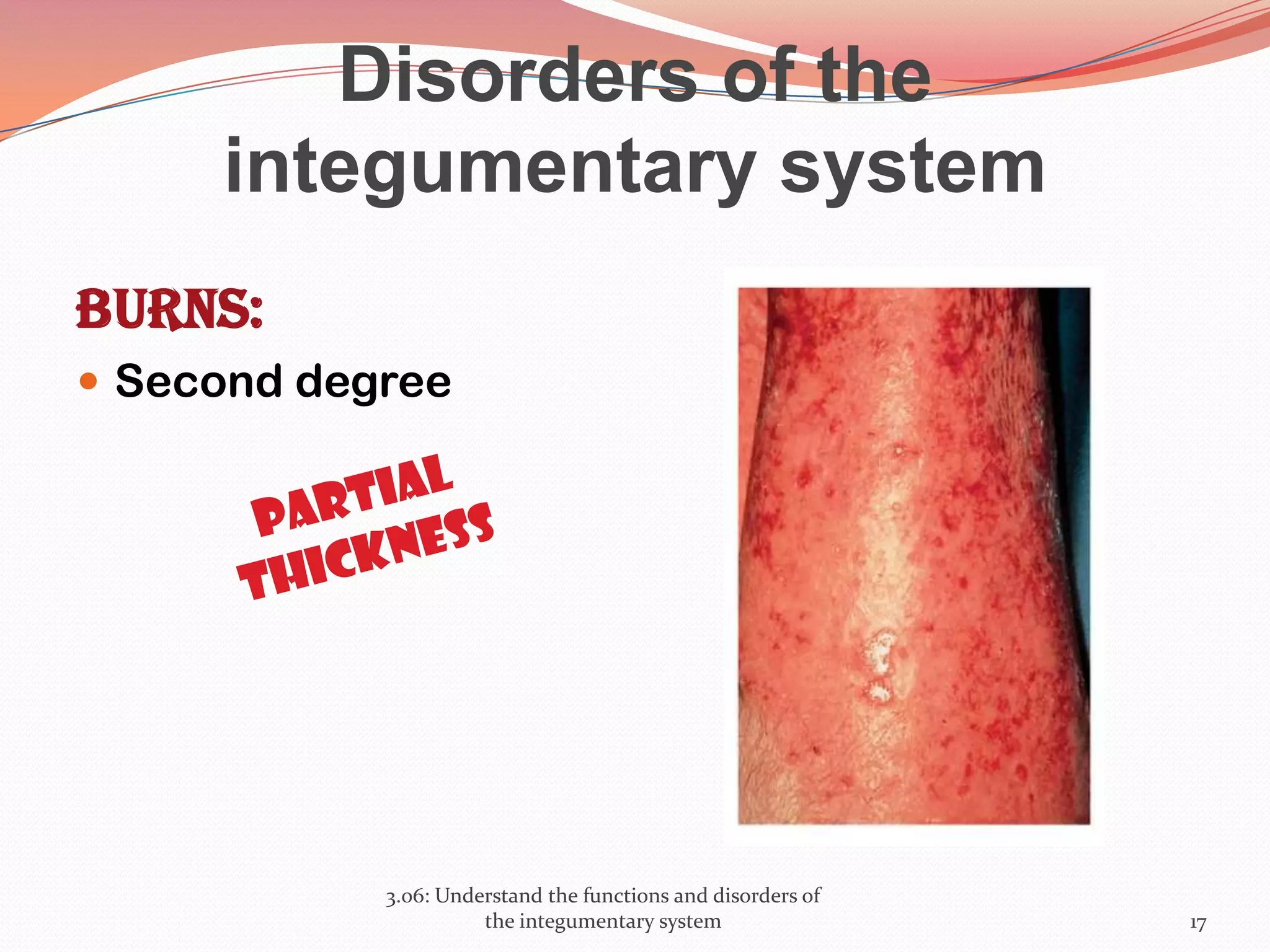
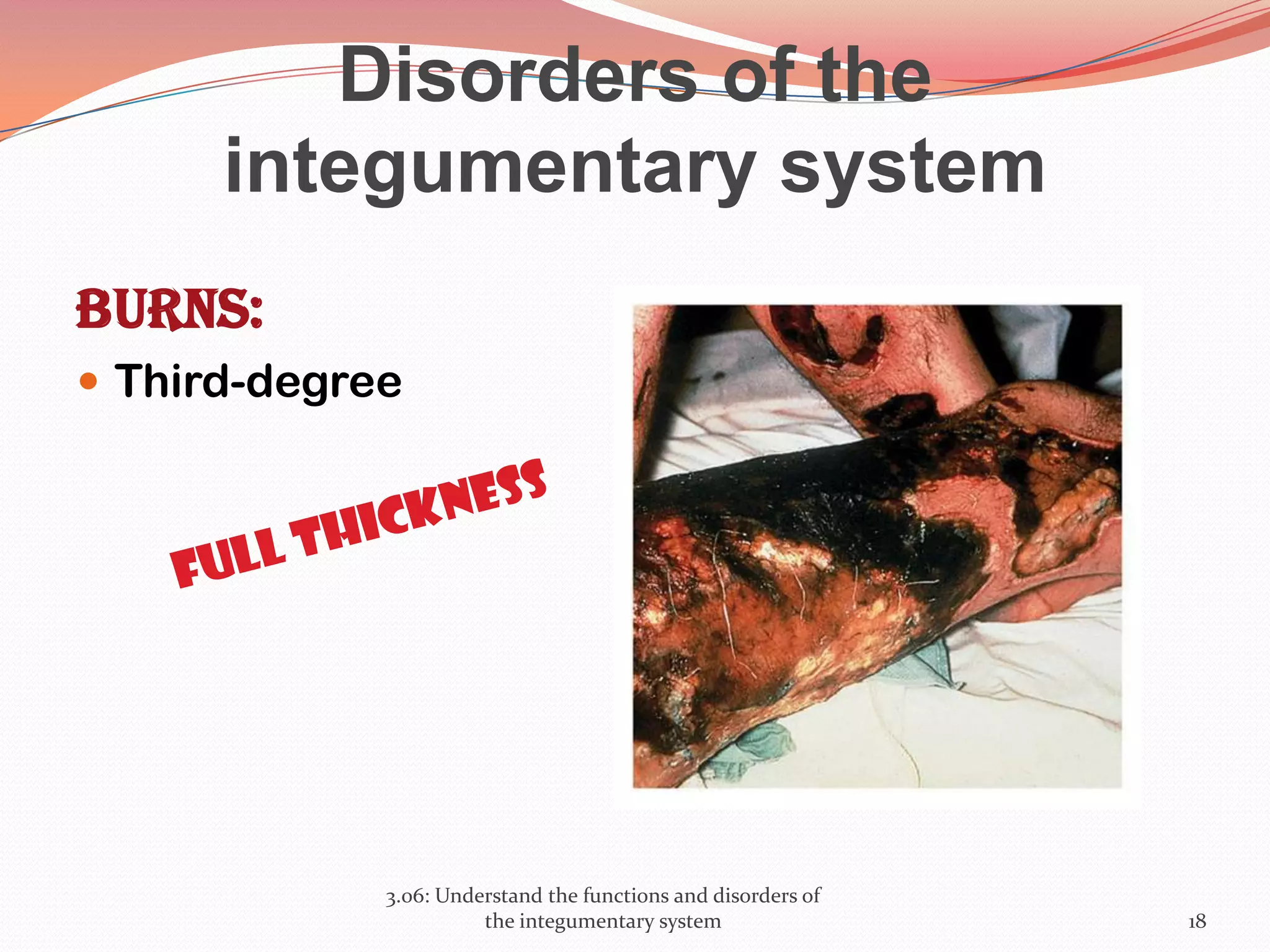
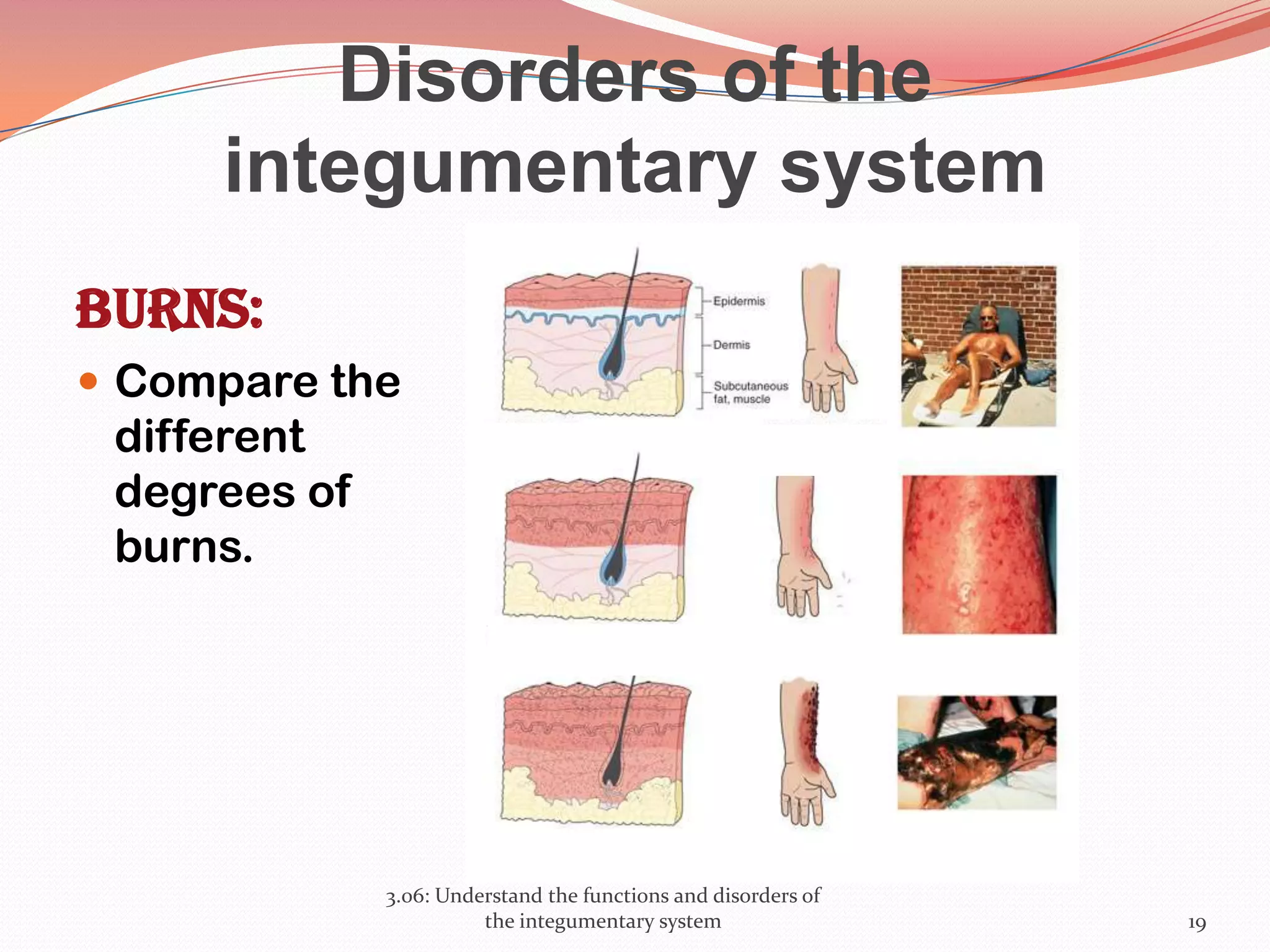
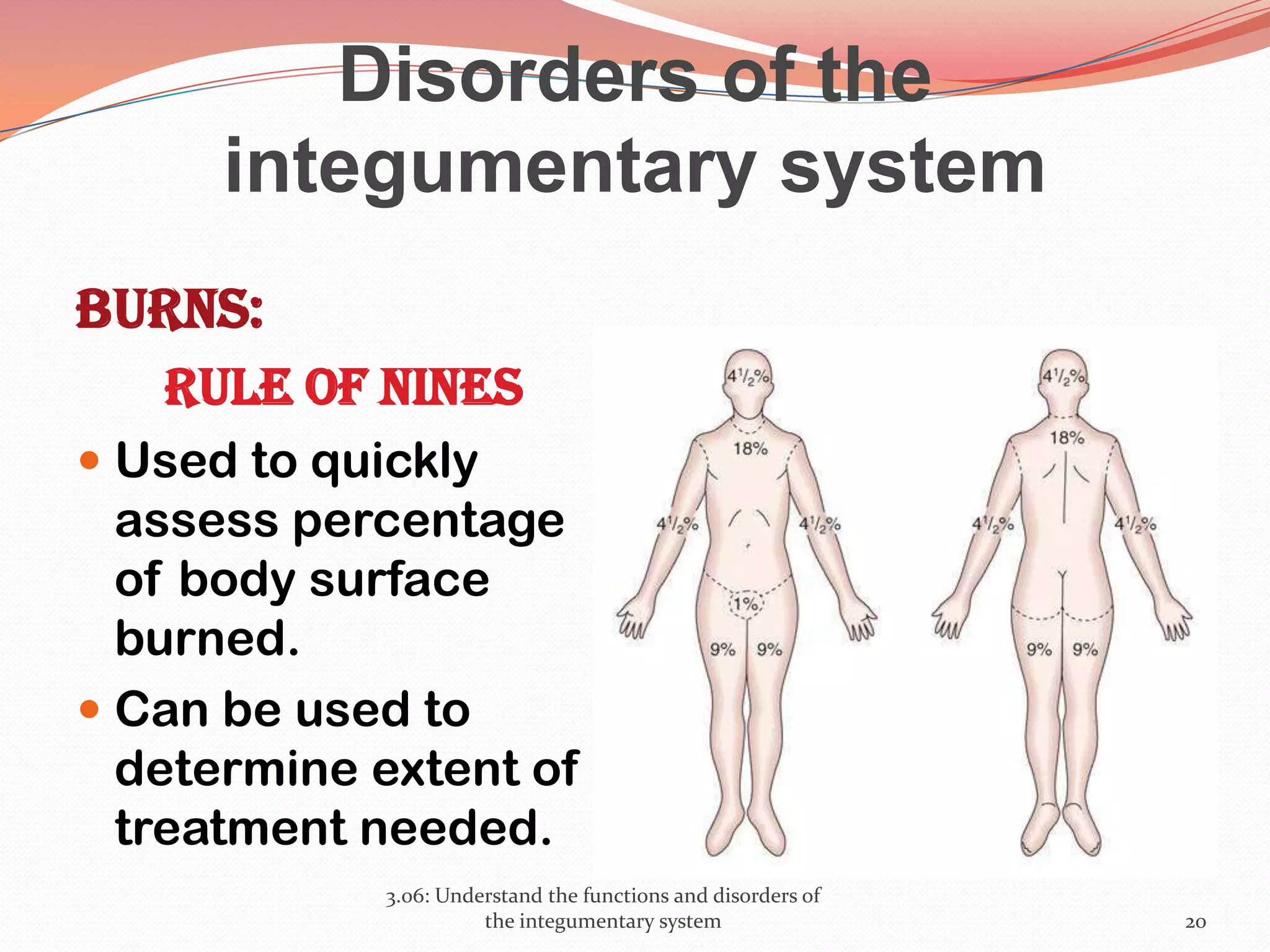
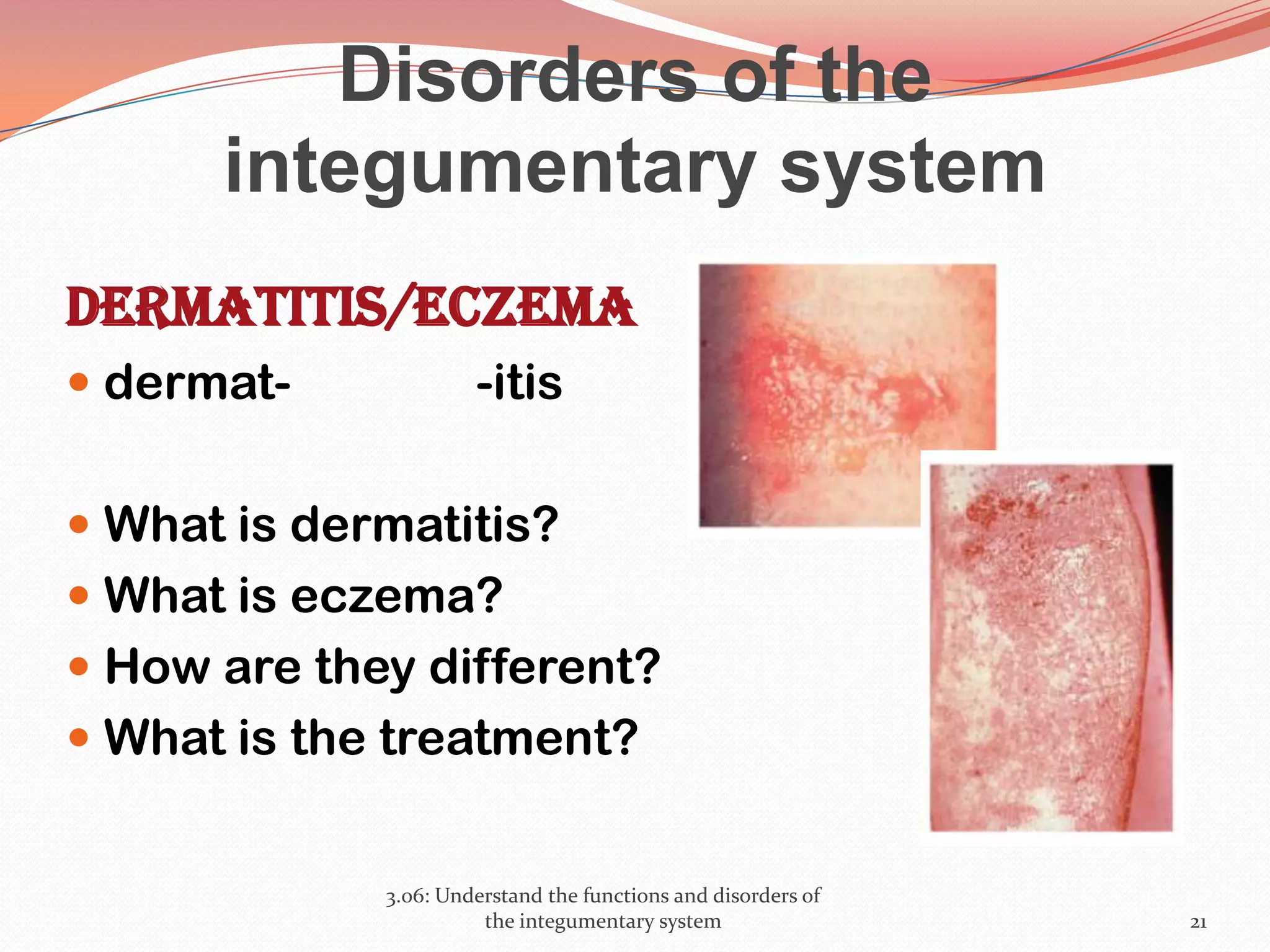
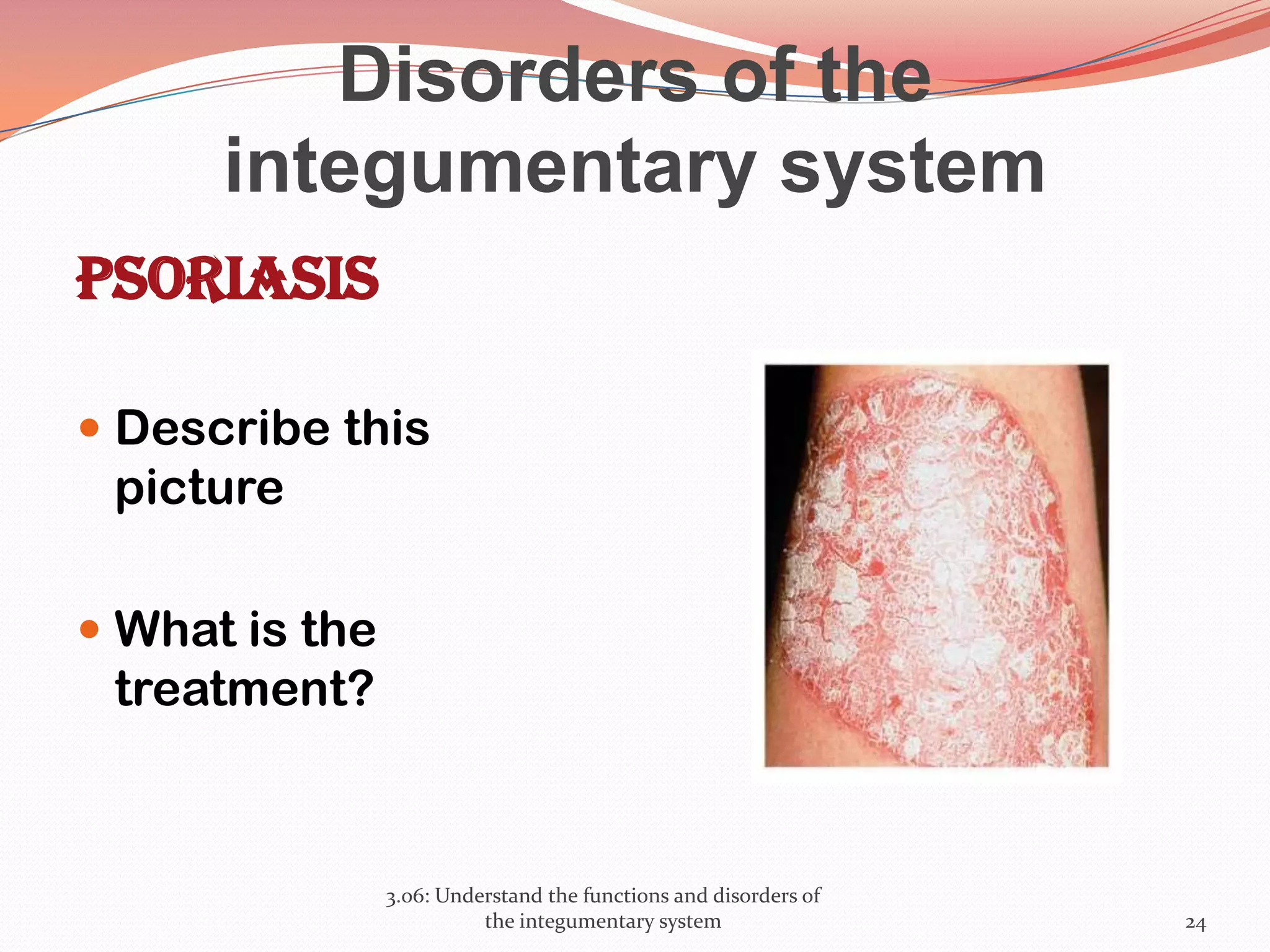
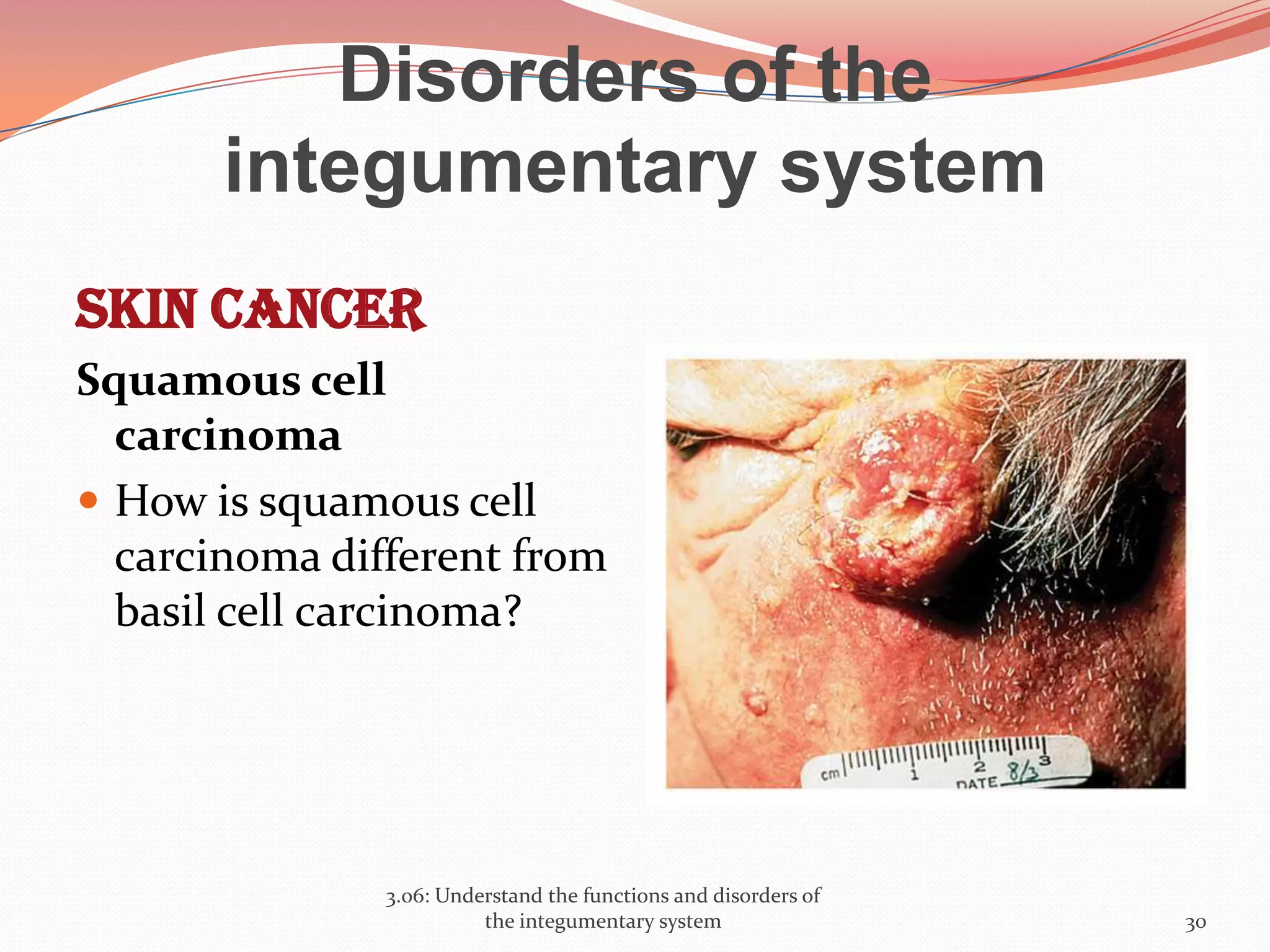
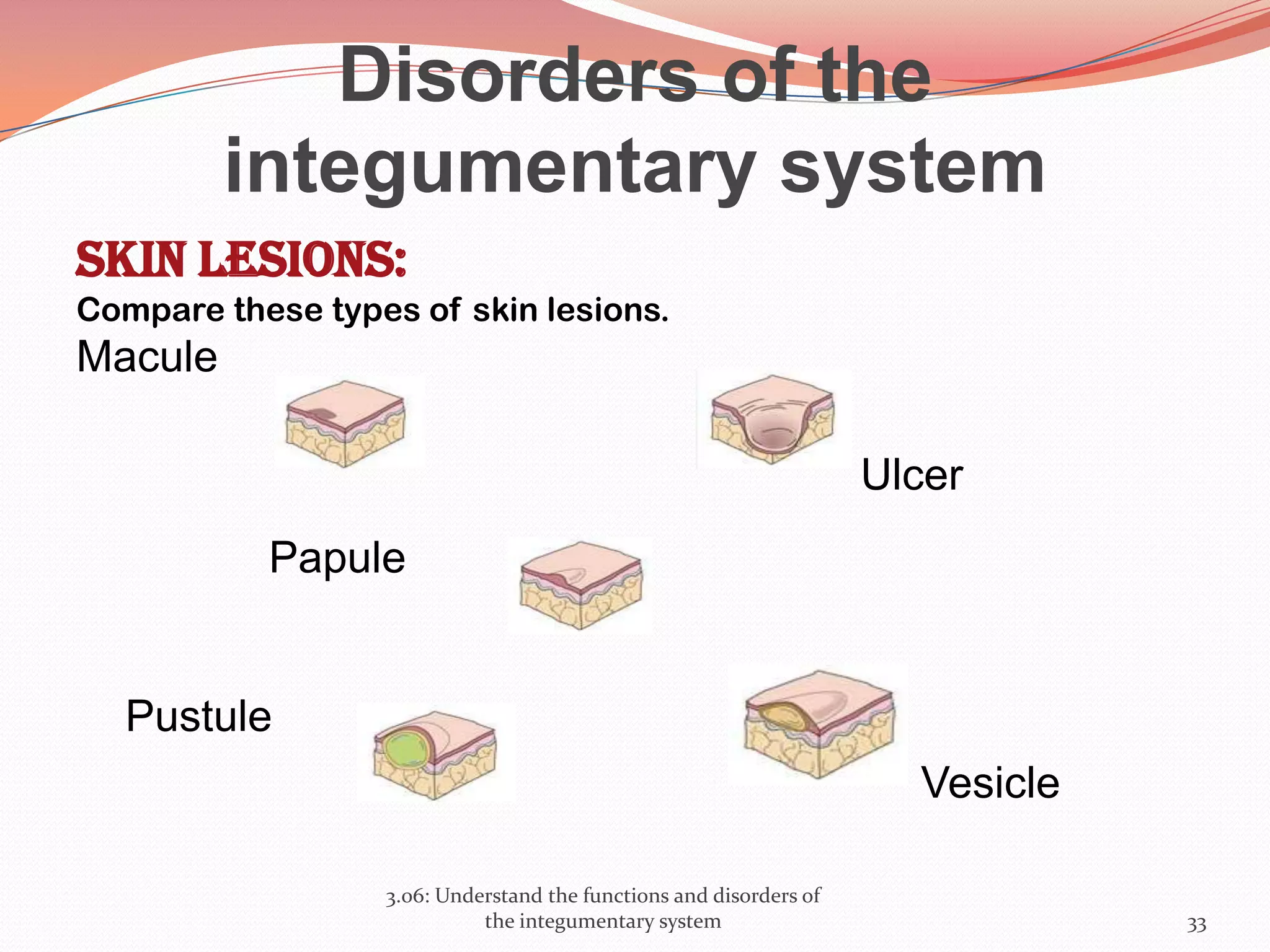
This document discusses the functions and disorders of the integumentary system. It begins by outlining the seven main functions of the skin, which include absorption, excretion, production, protection, regulation, perception, and storage. It then describes the layers of the skin - epidermis, dermis, and subcutaneous layer - and their roles. The document also examines various disorders that can affect the skin, such as acne, burns, dermatitis, eczema, herpes, impetigo, psoriasis, ringworm, scabies, shingles, and skin cancers. It concludes by relating the integumentary system to the body's communication systems.