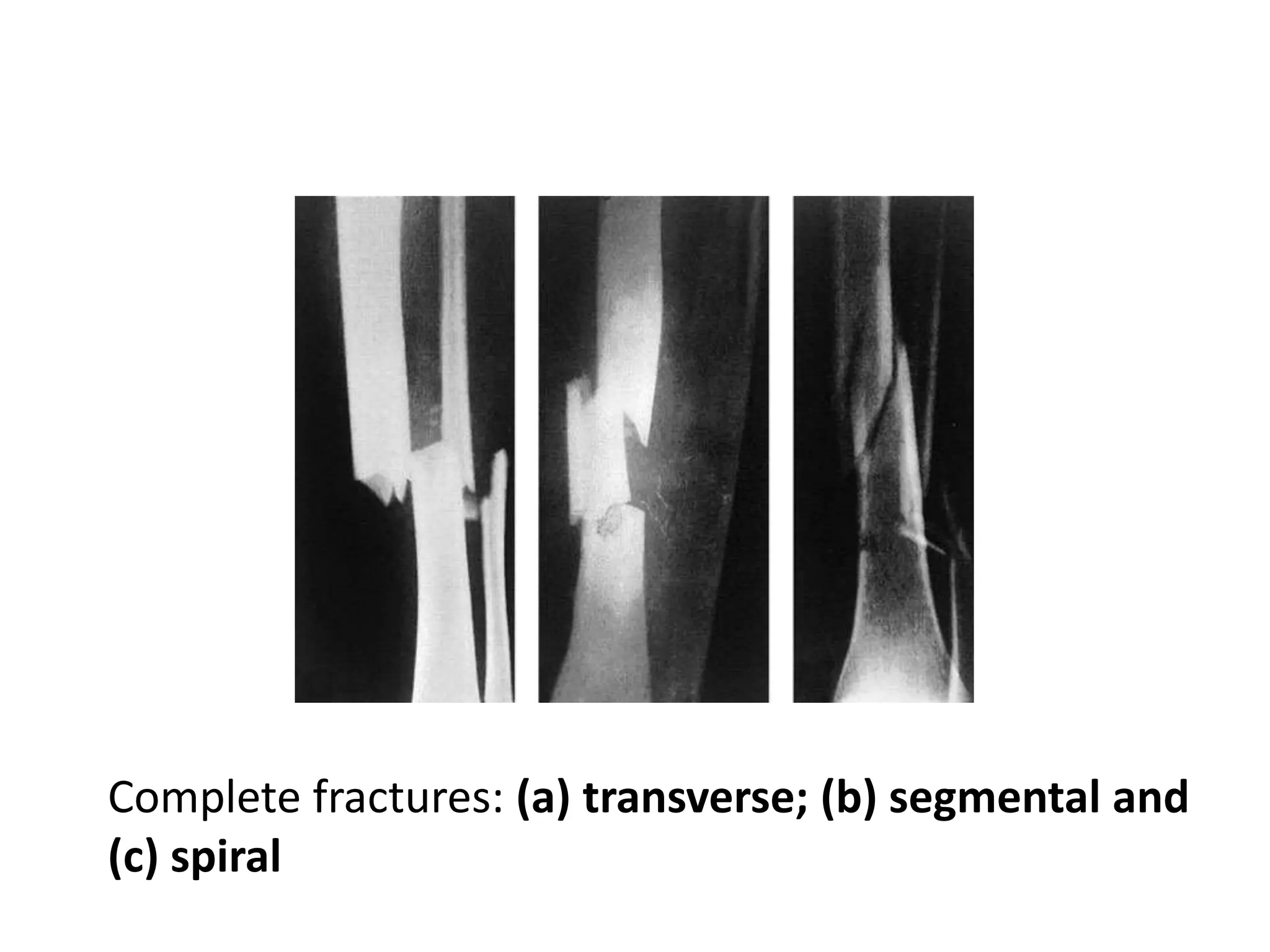
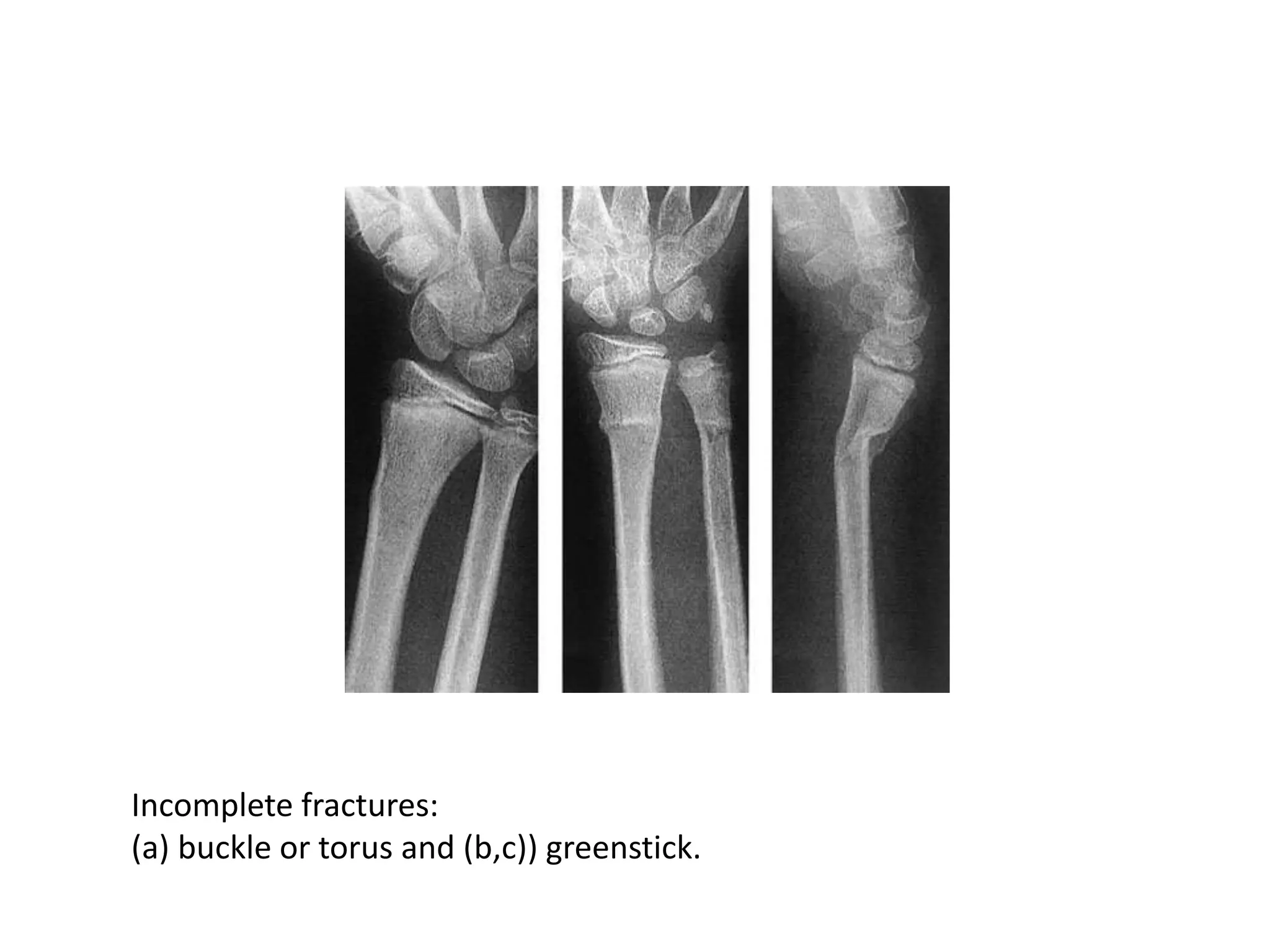
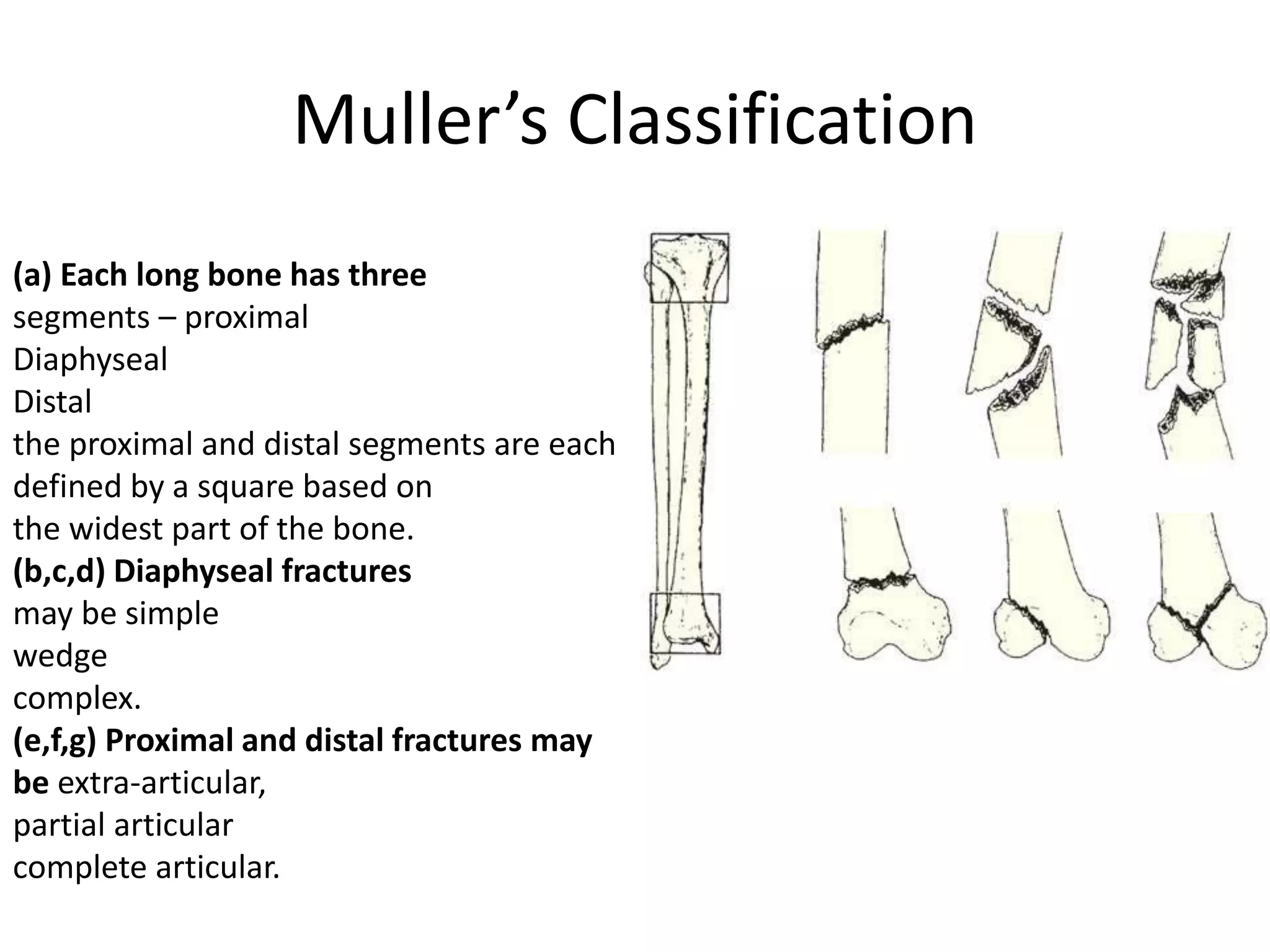
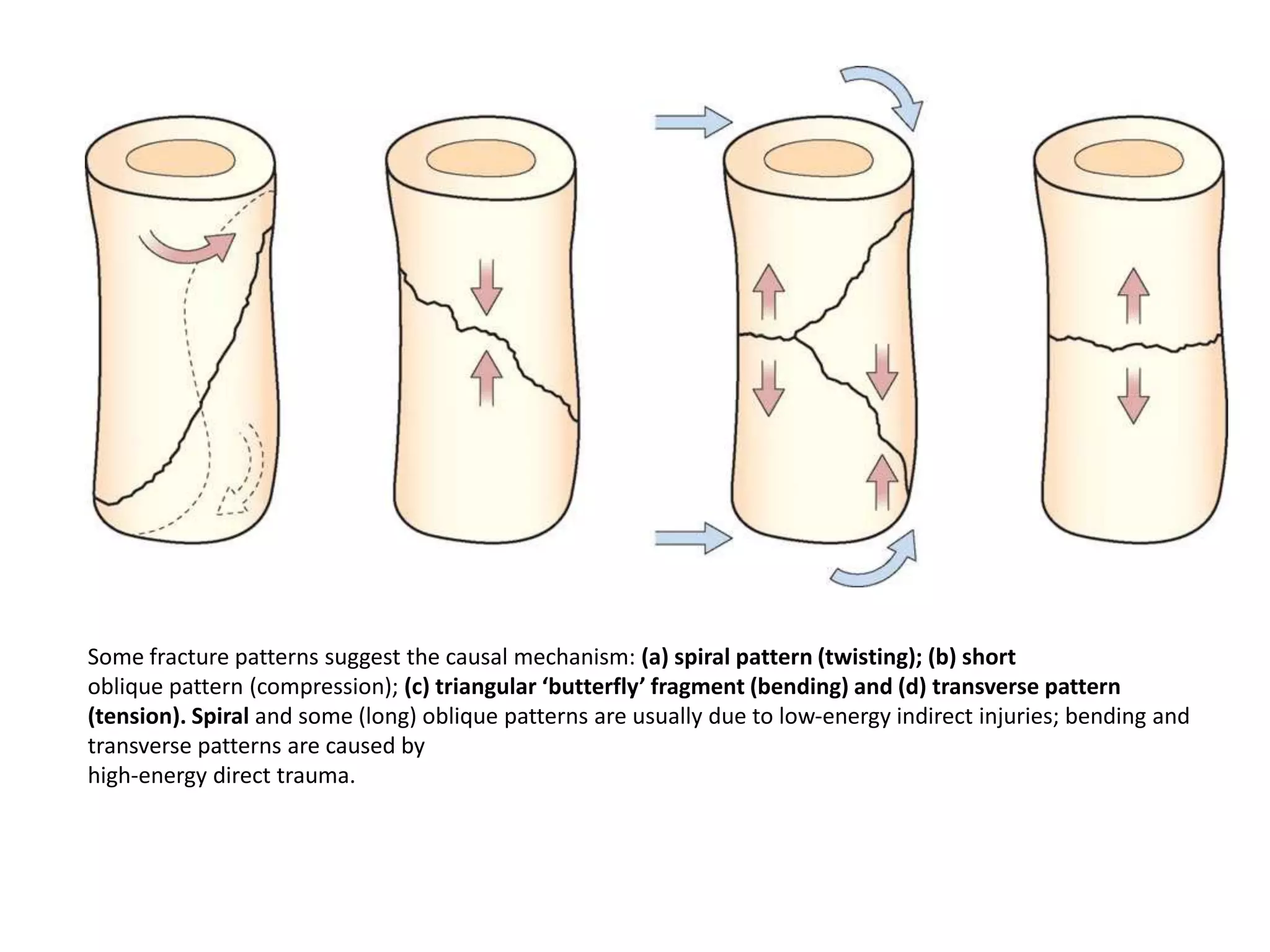
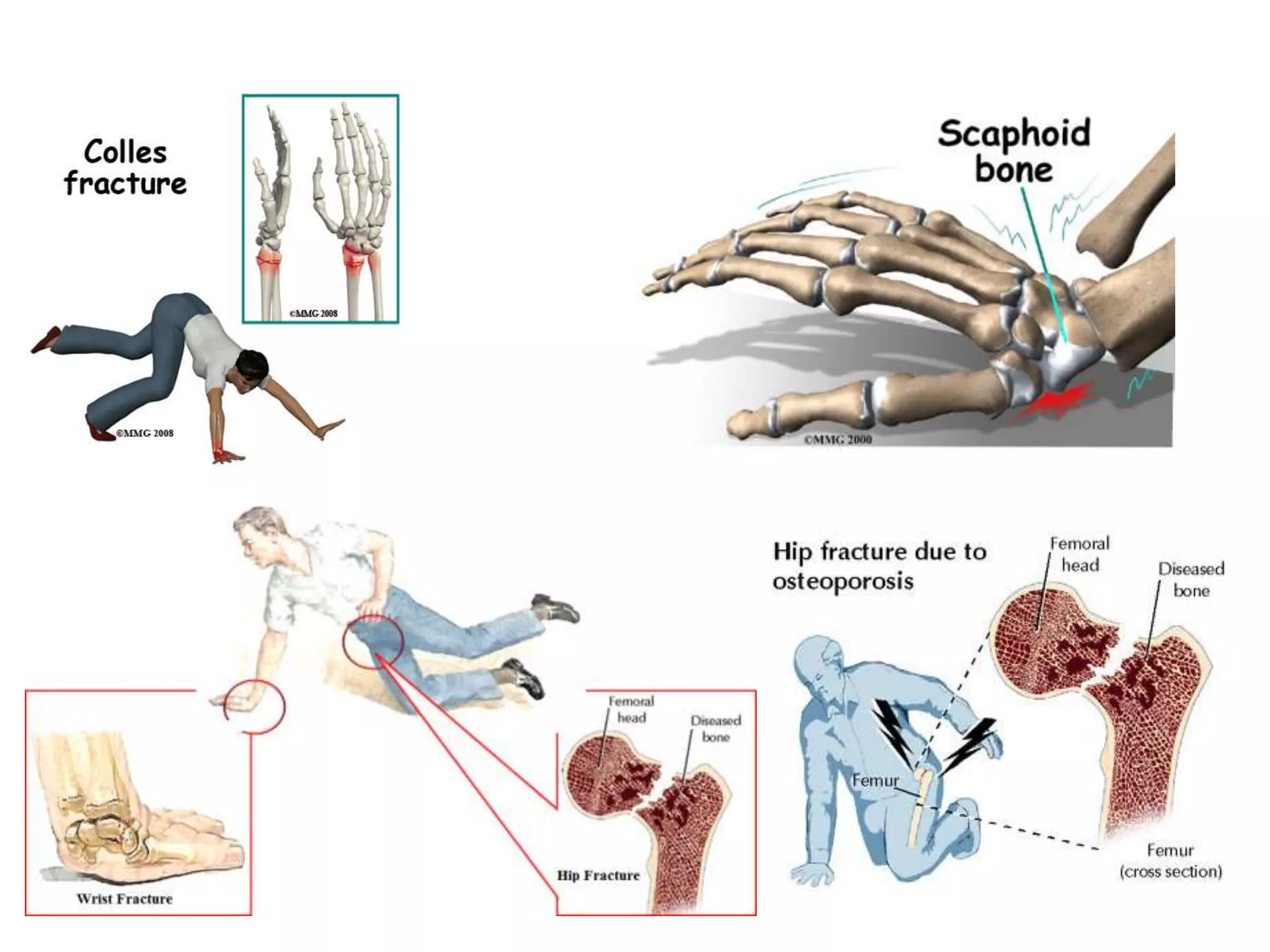
1. The document describes different types of fractures including complete, incomplete, impacted and comminuted fractures. It also discusses fracture classification systems and factors that influence bone healing.
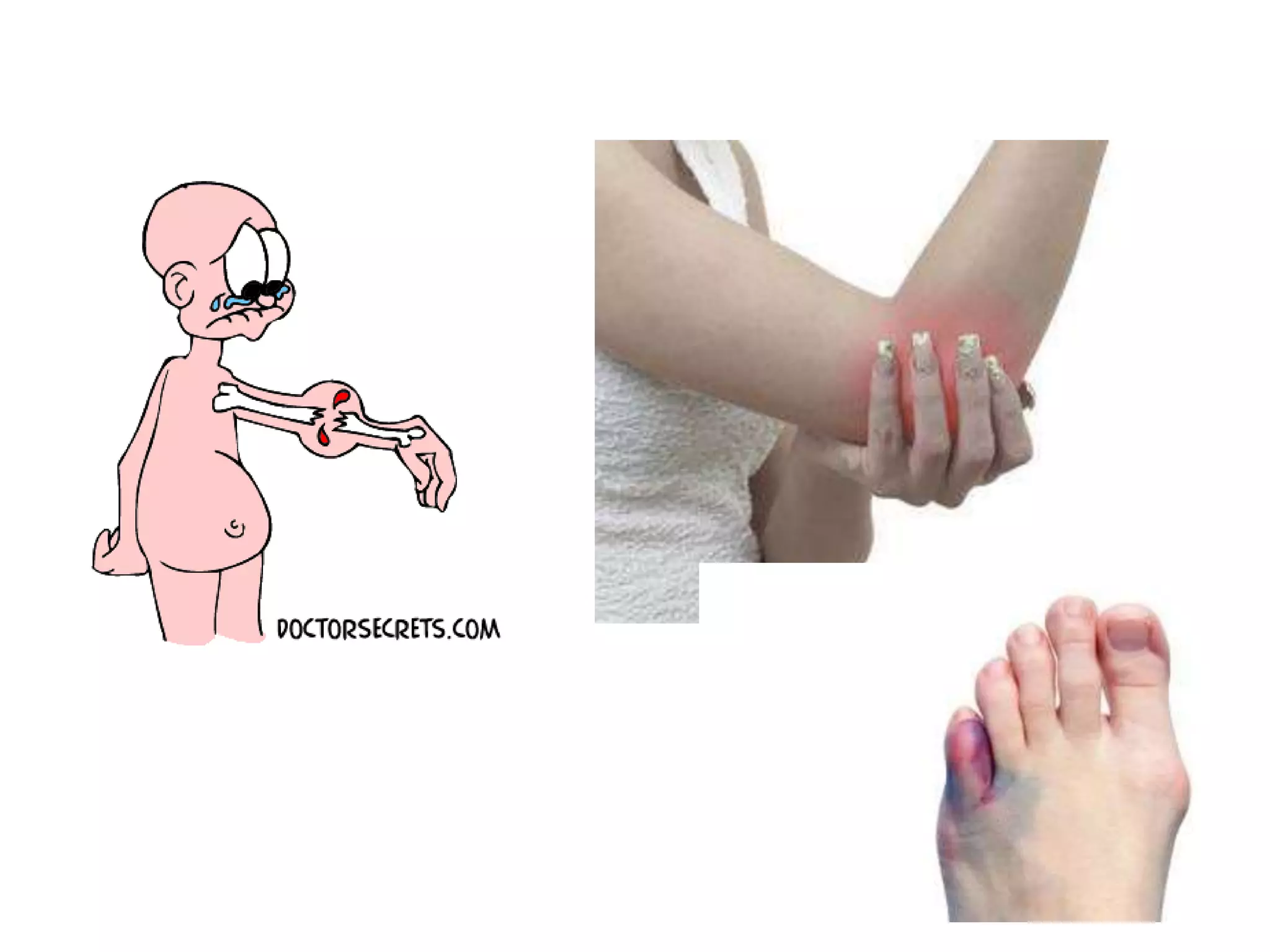
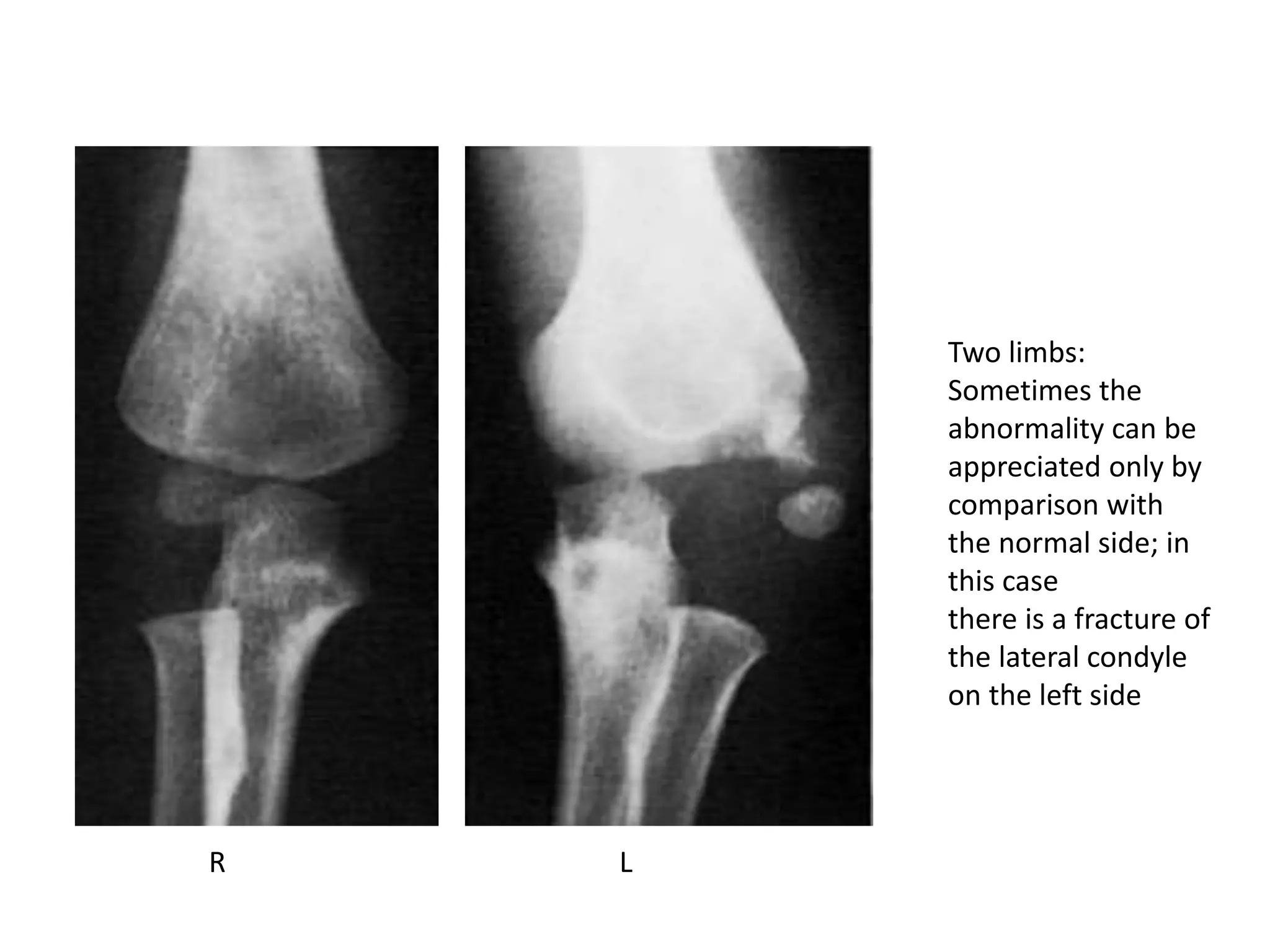
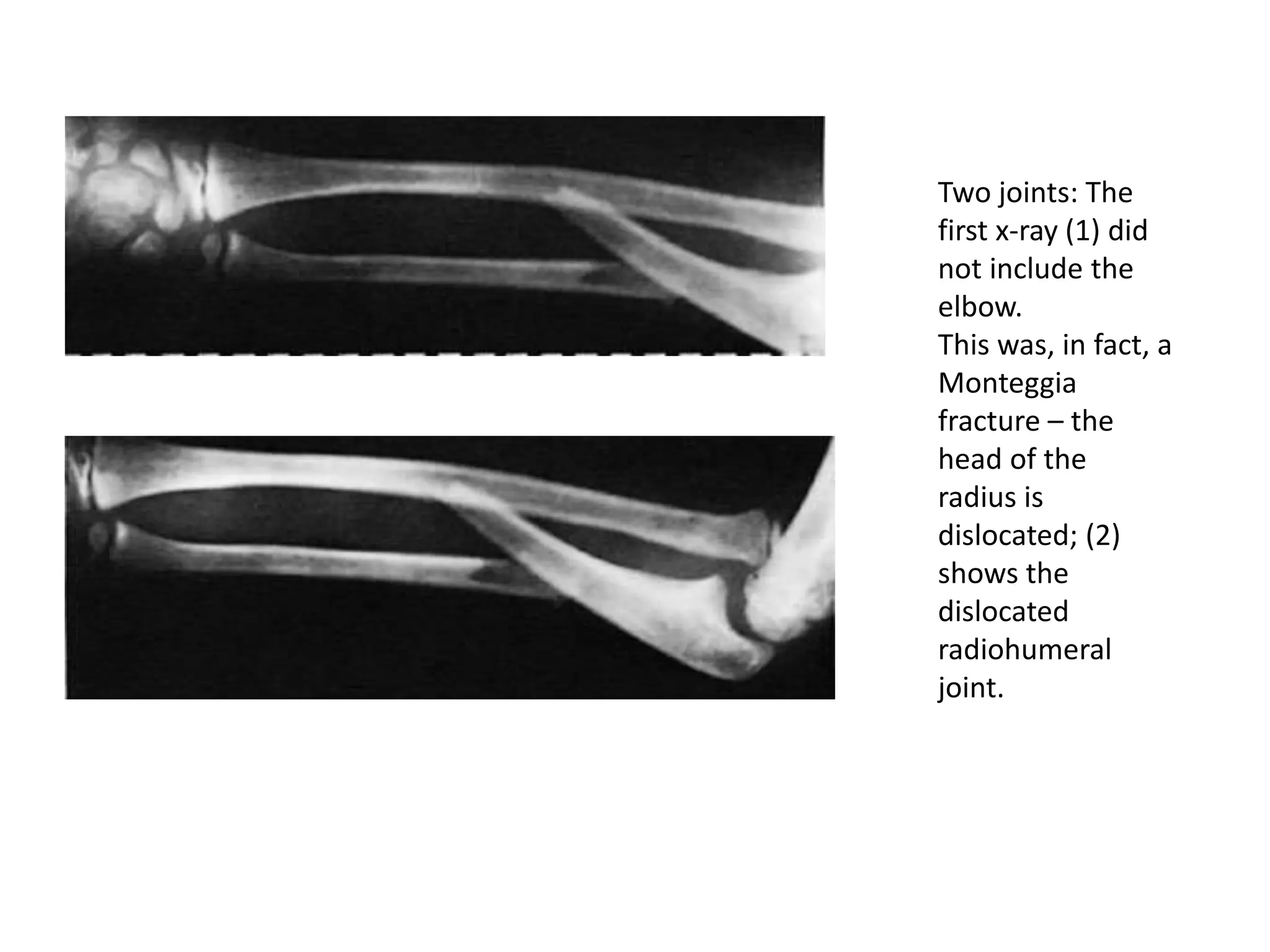
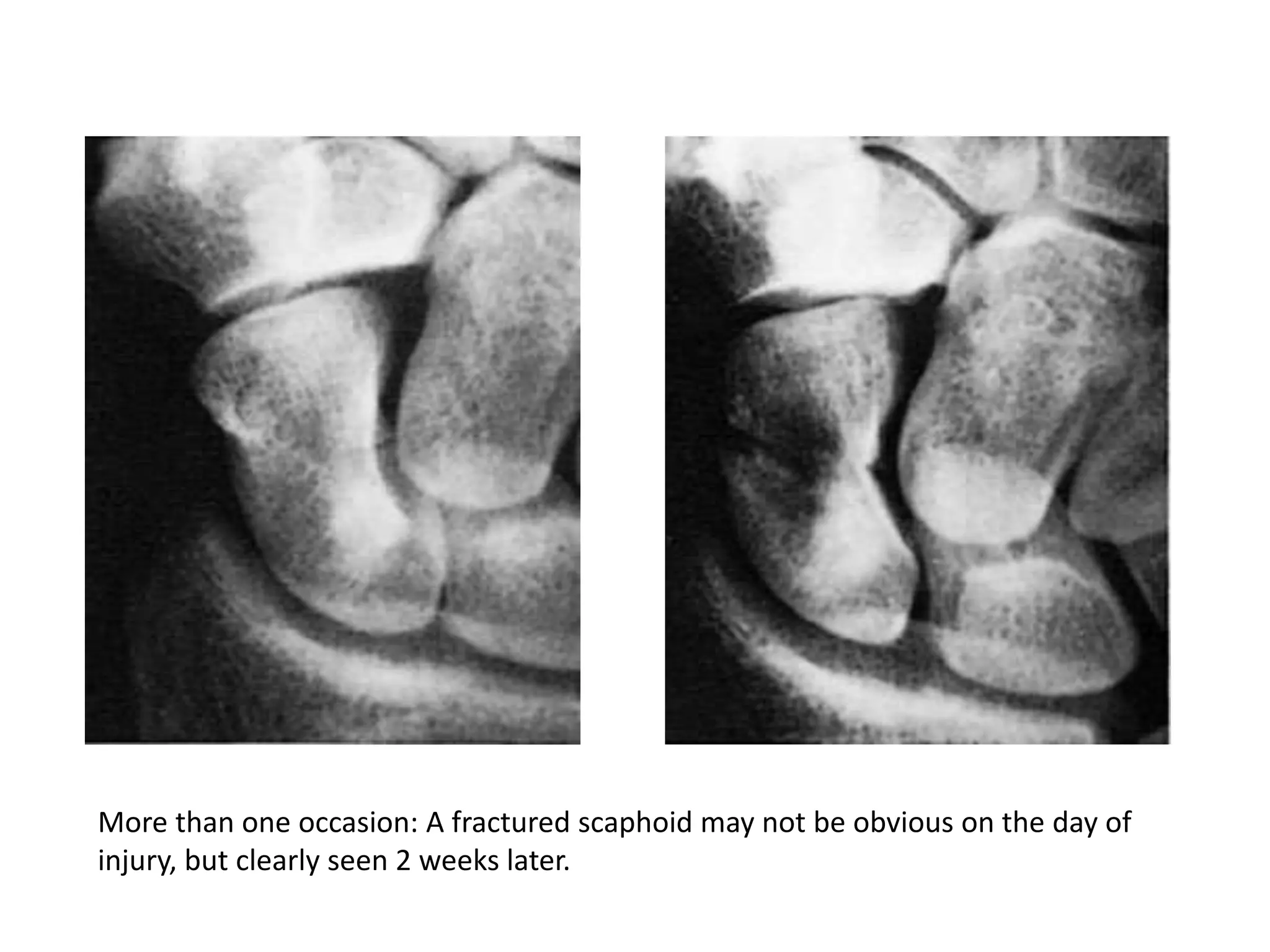
2. Clinical signs of fractures include pain, swelling, deformity, loss of function. Examination involves inspection, palpation, and assessment of range of motion. Imaging plays a key role in diagnosis and fracture characterization.
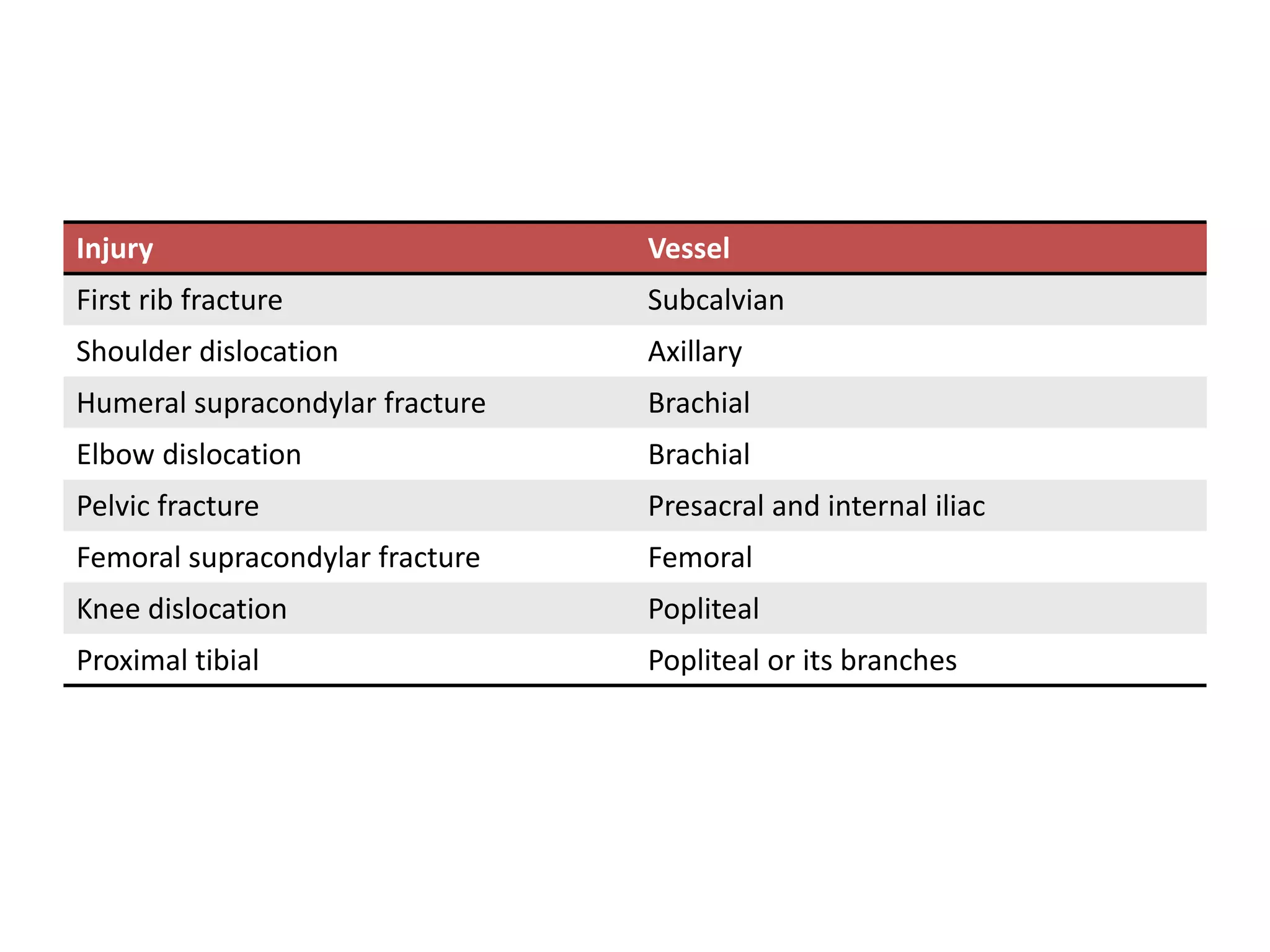
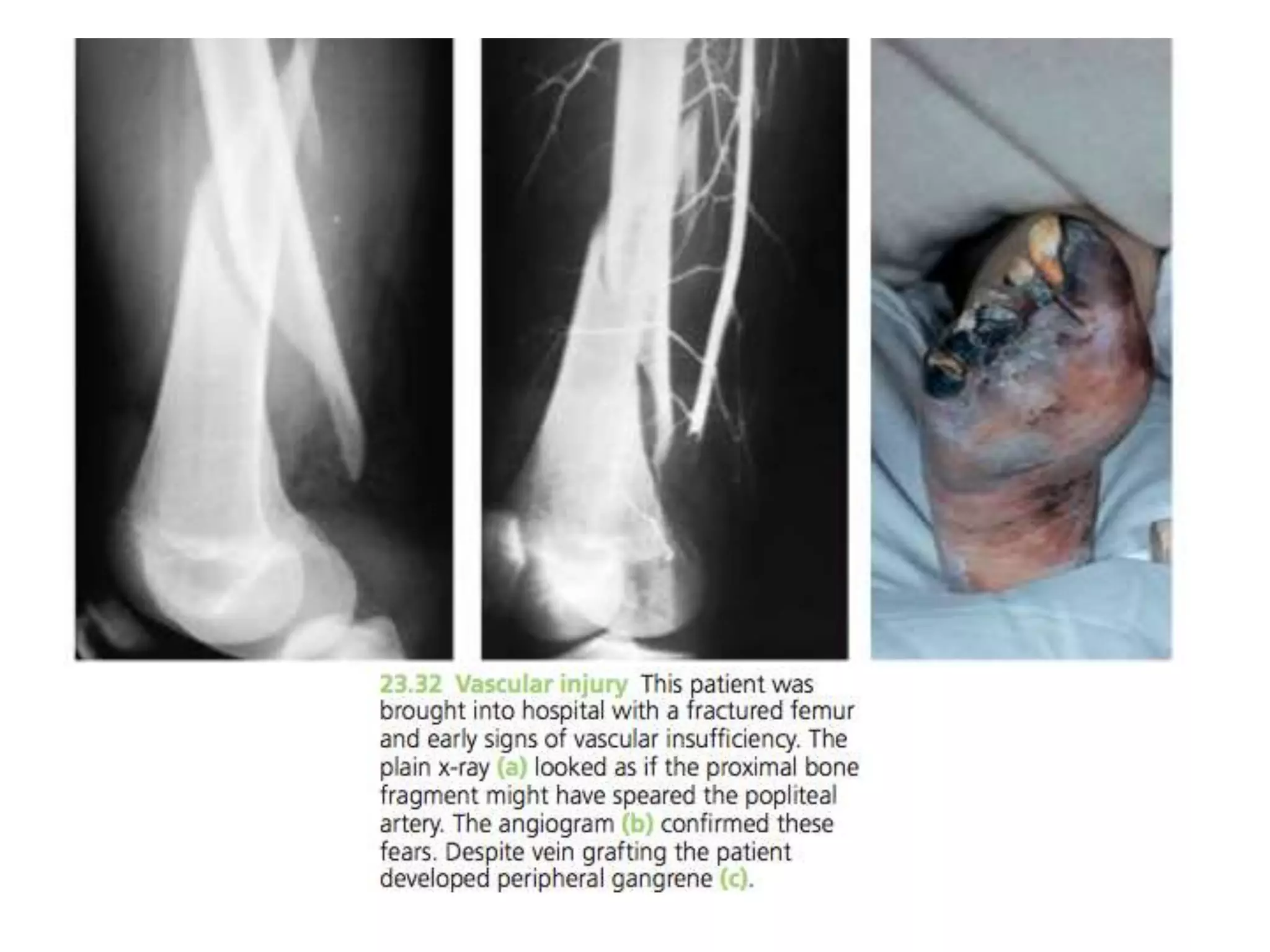
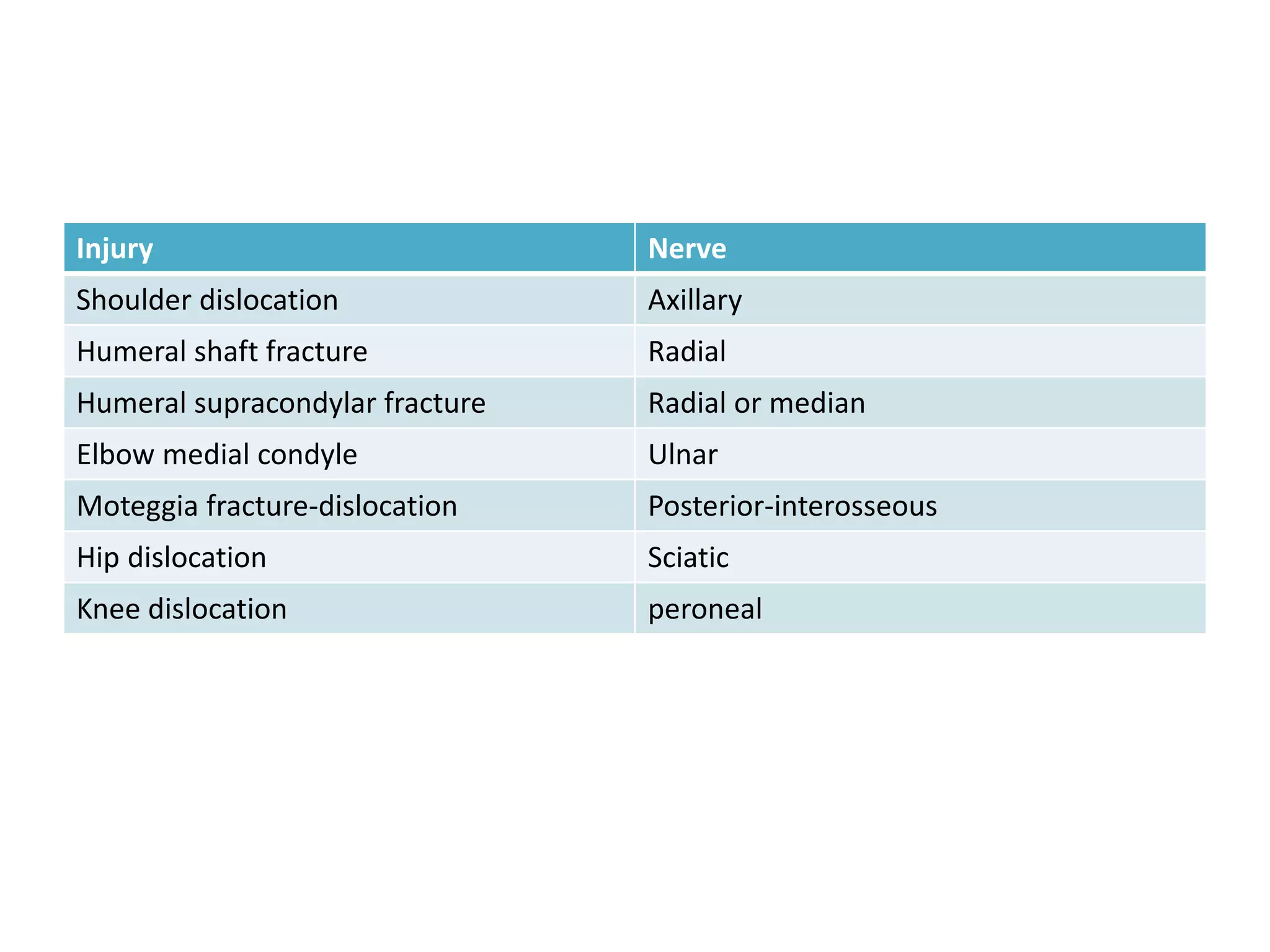
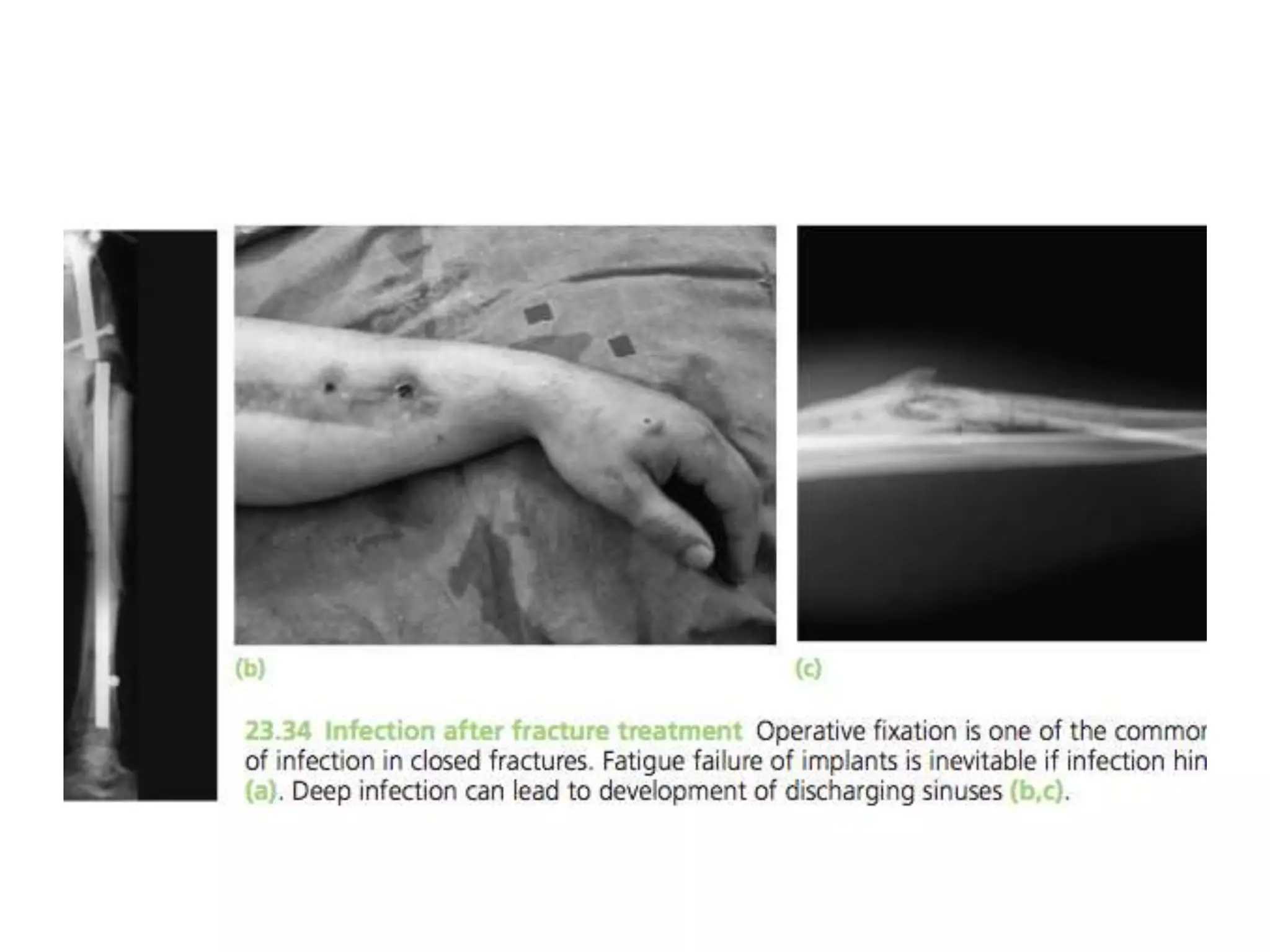
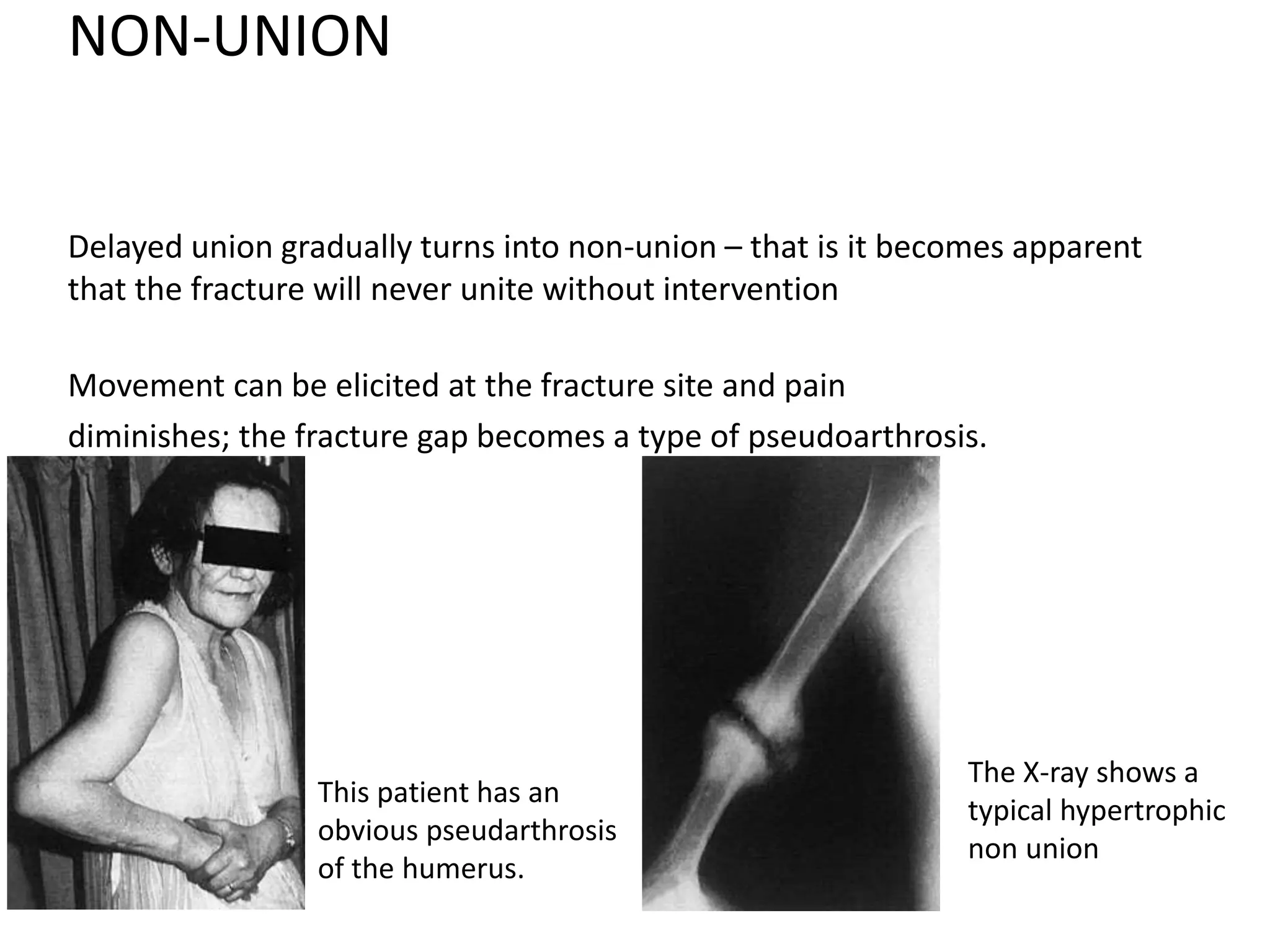
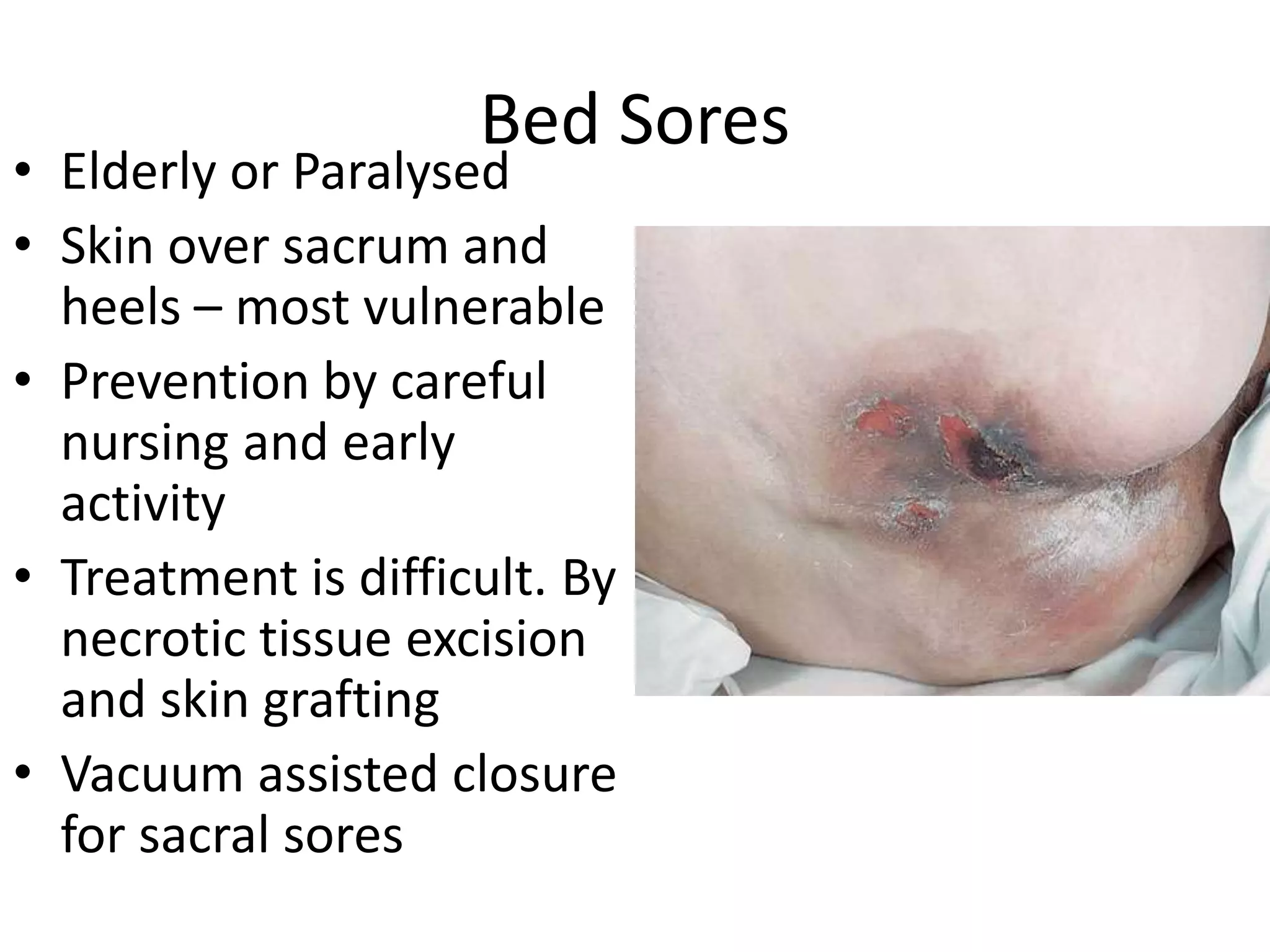
3. Potential complications of fractures include vascular or nerve injury, visceral injury, infection, and malunion. Proper diagnosis and management can help prevent long-term disability.