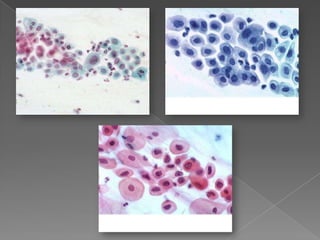
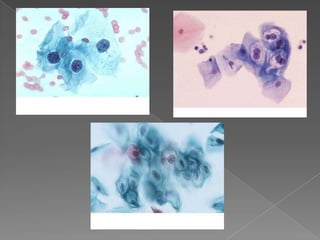
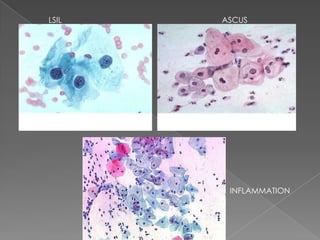
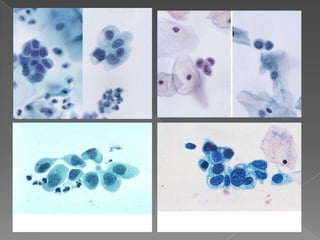
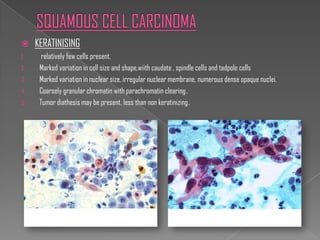
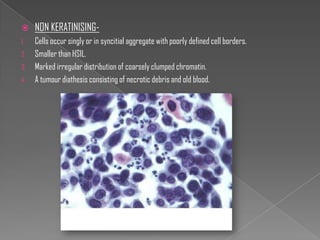
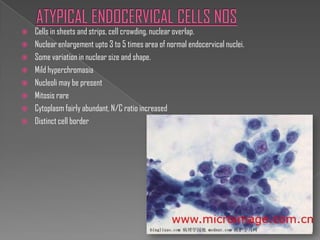
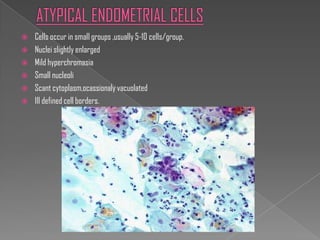
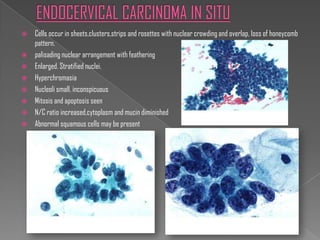
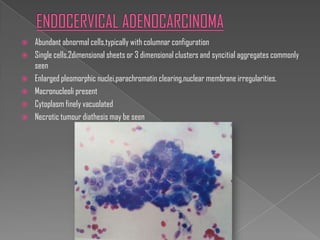
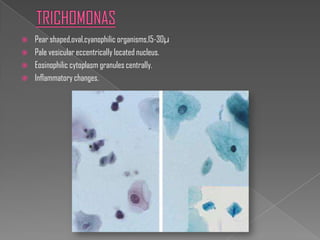
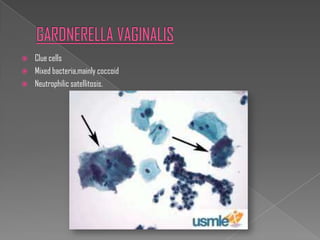
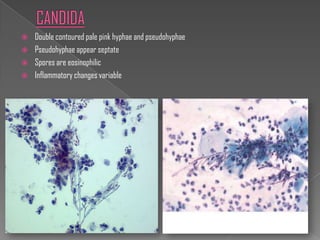
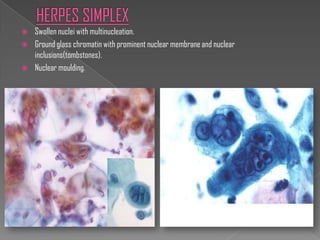
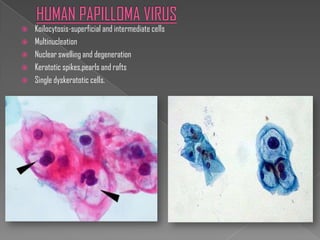
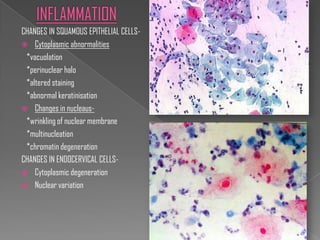
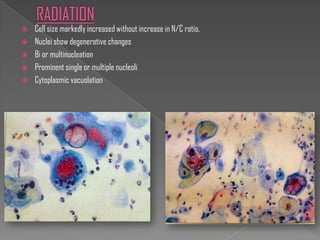
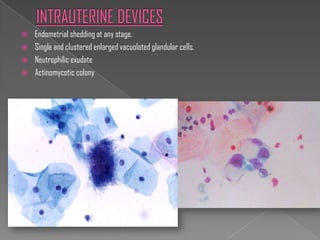
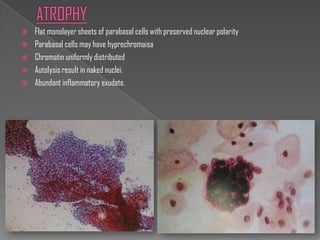
The document discusses the Bethesda system for reporting cervical cytology and Pap test results. It outlines categories for specimen adequacy, diagnostic categories including non-neoplastic and neoplastic findings, criteria for various diagnoses, and follow-up guidelines. Key aspects covered include definitions of satisfactory and unsatisfactory specimens, classification of squamous and glandular cell abnormalities, and management recommendations for different diagnoses.