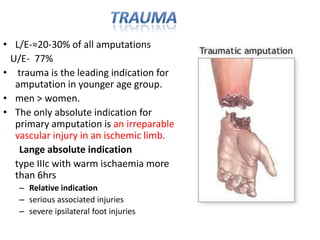
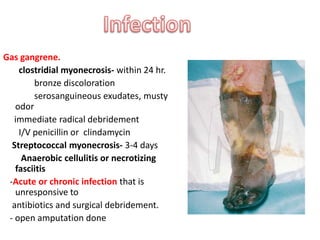
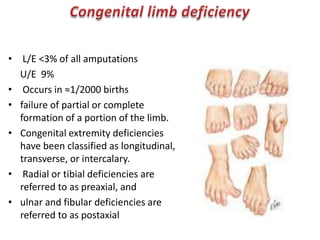
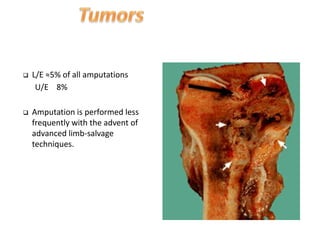
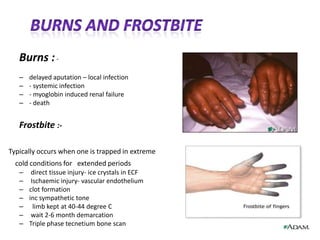
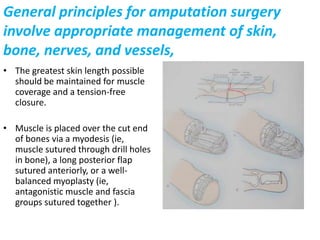
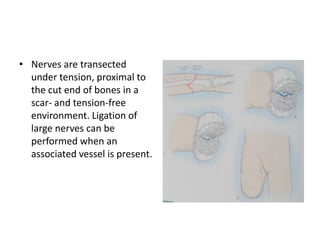
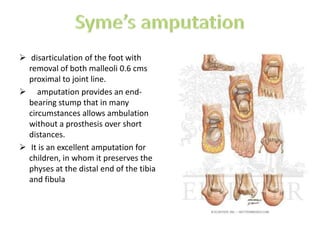
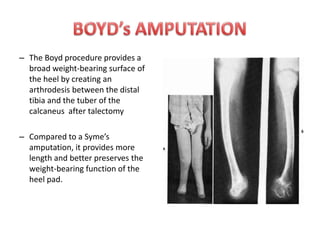
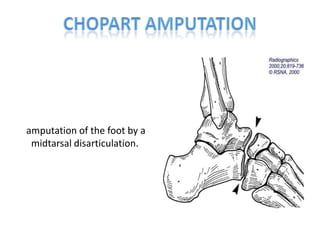
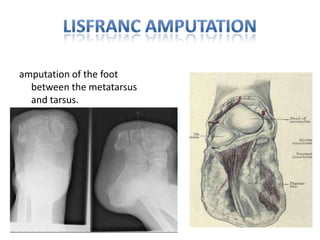
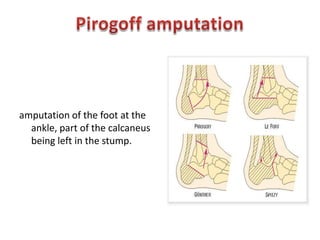
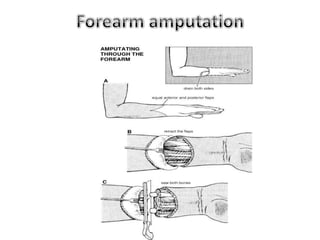
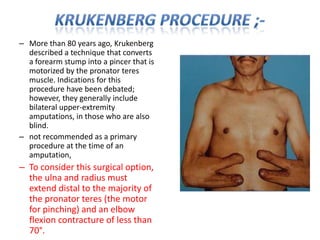
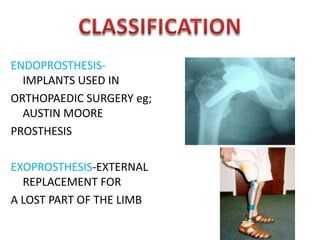
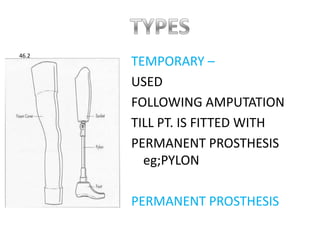
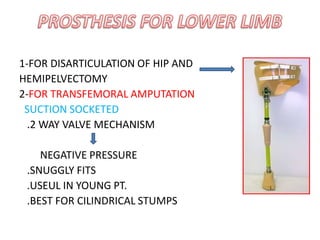
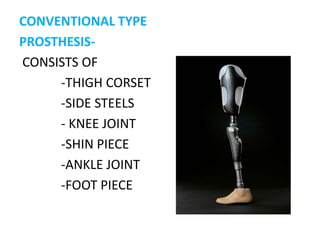
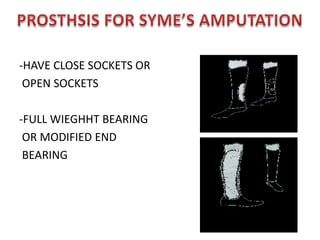
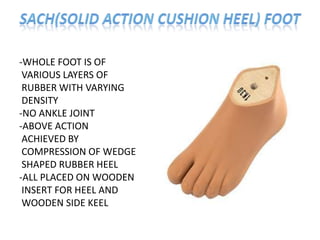
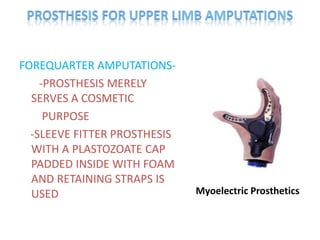
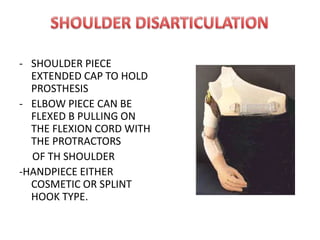
The document discusses amputation, including definitions, history, indications, types, postoperative care, complications, and special procedures. It notes that amputation involves surgical removal of part or all of a limb through bone or joints. The main indications are trauma, peripheral vascular disease, infection, tumors, and congenital anomalies. Postoperative goals are prompt healing, edema control, pain management, and early rehabilitation and prosthesis training. Complications can include wound issues, infection, phantom pain, and psychological impacts.