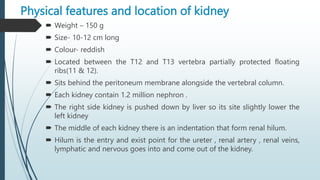
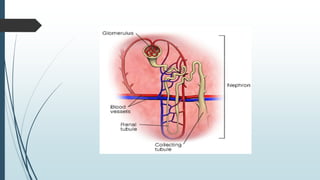
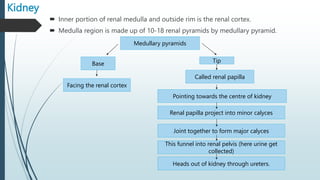
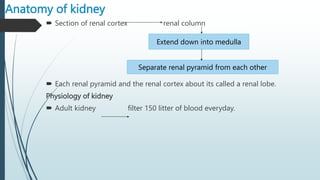
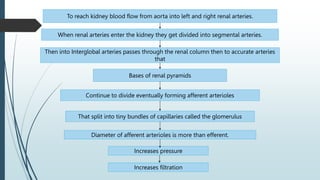
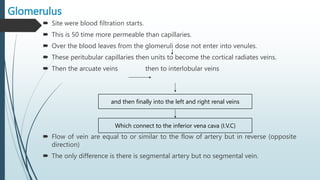
The document provides an in-depth overview of the urinary system, highlighting the structure and function of the kidneys, ureters, bladder, and urethra. It details how kidneys filter blood and manage waste, balance fluids and electrolytes, and maintain acid-base balance. Additionally, the document discusses the processes involved in urine formation and the mechanics of micturition, emphasizing the roles of various muscles and nerves in urination.