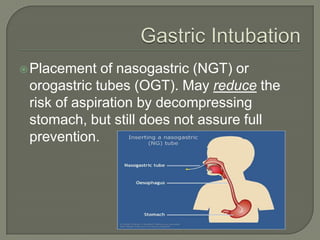
The document provides guidance on the assessment and management of trauma patients. It describes the golden hour period following trauma where rapid assessment is critical. The primary and secondary surveys are outlined, with the primary focusing on stabilizing vital functions like airway, breathing, circulation, disability and exposure. Specific injuries and treatments are discussed for areas like head trauma, spinal trauma, chest trauma, abdominal trauma and genitourinary trauma. Throughout, the emphasis is on stabilizing life-threatening injuries and rapidly diagnosing and treating problems that could impair ventilation or circulation.