Embed presentation

















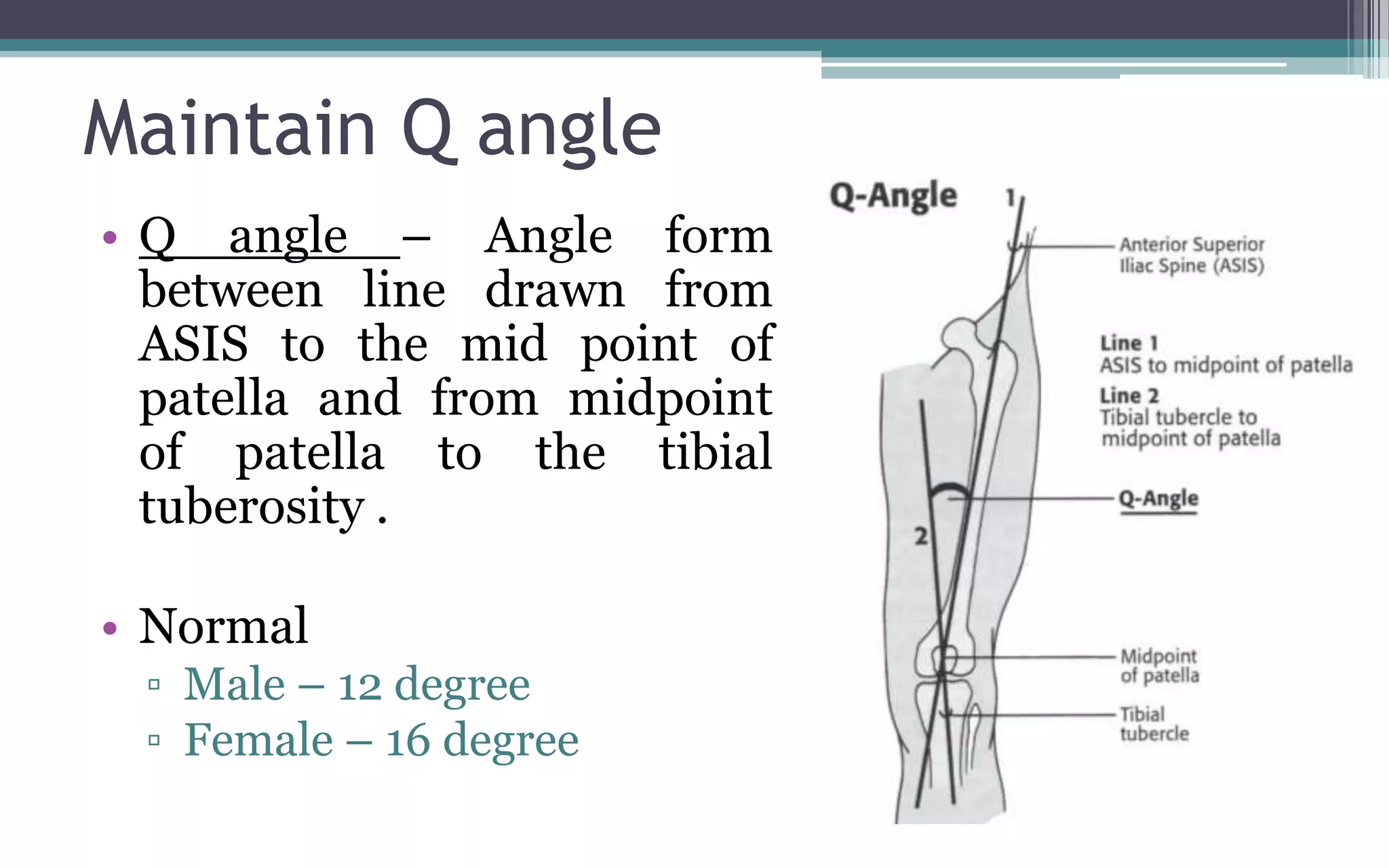







Total knee arthroplasty aims to restore mechanical alignment, preserve the joint line, balance ligaments, and maintain the Q angle through various surgical techniques. Restoring mechanical alignment involves cutting the femur and tibia perpendicular to the mechanical axis to allow forces through the knee to pass through the center. This optimizes load sharing and prevents excessive wear. Maintaining the original joint line height is also important for proper knee function and biomechanics. Ligament balancing in both the coronal and sagittal planes is required to achieve stability throughout range of motion.
























