The Large Intestine. The Large Intestine.
•Download as PPTX, PDF•
0 likes•1 view
The Large Intestine.
Report
Share
Report
Share
Recommended
Recommended
More Related Content
Similar to The Large Intestine. The Large Intestine.
Similar to The Large Intestine. The Large Intestine. (20)
Intestines(movements and secretions of small and large intestines ) The Guyto...

Intestines(movements and secretions of small and large intestines ) The Guyto...
Introduction to GIT by Pandian M, Dept of Physiology, DYPMC,KOP,MH

Introduction to GIT by Pandian M, Dept of Physiology, DYPMC,KOP,MH
More from nidhi sharma
More from nidhi sharma (20)
Muscles Bones of Lower Limb Lower Limb Bones of LL HUMAN

Muscles Bones of Lower Limb Lower Limb Bones of LL HUMAN
Male and Female Reproductive Systems 2024 jan. pptx human medical anatomy hum...

Male and Female Reproductive Systems 2024 jan. pptx human medical anatomy hum...
hepatobiliary system 2024.pptx hepatobiliary system

hepatobiliary system 2024.pptx hepatobiliary system
CELL COMPONENTS.pptx human body anatomy medical human anatomy

CELL COMPONENTS.pptx human body anatomy medical human anatomy
RADIO-ULNAR JOINT IS THE JOINT PRESENT IN HUMAN UPPER LIMB

RADIO-ULNAR JOINT IS THE JOINT PRESENT IN HUMAN UPPER LIMB
RADIO-ULNAR JOINT IS THE JOINT OF UPPER LIMB IN HUMAN BODY

RADIO-ULNAR JOINT IS THE JOINT OF UPPER LIMB IN HUMAN BODY
Recently uploaded
This presentation was provided by William Mattingly of the Smithsonian Institution, during the seventh segment of the NISO training series "AI & Prompt Design." Session 7: Open Source Language Models, was held on May 16, 2024.Mattingly "AI and Prompt Design: LLMs with Text Classification and Open Source"

Mattingly "AI and Prompt Design: LLMs with Text Classification and Open Source"National Information Standards Organization (NISO)
https://app.box.com/s/cbgl8f0rgcll2fzdqp83sjxx8nom8188TỔNG HỢP HƠN 100 ĐỀ THI THỬ TỐT NGHIỆP THPT VẬT LÝ 2024 - TỪ CÁC TRƯỜNG, TRƯ...

TỔNG HỢP HƠN 100 ĐỀ THI THỬ TỐT NGHIỆP THPT VẬT LÝ 2024 - TỪ CÁC TRƯỜNG, TRƯ...Nguyen Thanh Tu Collection
Recently uploaded (20)
Mattingly "AI and Prompt Design: LLMs with Text Classification and Open Source"

Mattingly "AI and Prompt Design: LLMs with Text Classification and Open Source"
Incoming and Outgoing Shipments in 2 STEPS Using Odoo 17

Incoming and Outgoing Shipments in 2 STEPS Using Odoo 17
PSYPACT- Practicing Over State Lines May 2024.pptx

PSYPACT- Practicing Over State Lines May 2024.pptx
Removal Strategy _ FEFO _ Working with Perishable Products in Odoo 17

Removal Strategy _ FEFO _ Working with Perishable Products in Odoo 17
MSc Ag Genetics & Plant Breeding: Insights from Previous Year JNKVV Entrance ...

MSc Ag Genetics & Plant Breeding: Insights from Previous Year JNKVV Entrance ...
TỔNG HỢP HƠN 100 ĐỀ THI THỬ TỐT NGHIỆP THPT VẬT LÝ 2024 - TỪ CÁC TRƯỜNG, TRƯ...

TỔNG HỢP HƠN 100 ĐỀ THI THỬ TỐT NGHIỆP THPT VẬT LÝ 2024 - TỪ CÁC TRƯỜNG, TRƯ...
Features of Video Calls in the Discuss Module in Odoo 17

Features of Video Calls in the Discuss Module in Odoo 17
The Ball Poem- John Berryman_20240518_001617_0000.pptx

The Ball Poem- John Berryman_20240518_001617_0000.pptx
Financial Accounting IFRS, 3rd Edition-dikompresi.pdf

Financial Accounting IFRS, 3rd Edition-dikompresi.pdf
Pragya Champions Chalice 2024 Prelims & Finals Q/A set, General Quiz

Pragya Champions Chalice 2024 Prelims & Finals Q/A set, General Quiz
The Large Intestine. The Large Intestine.
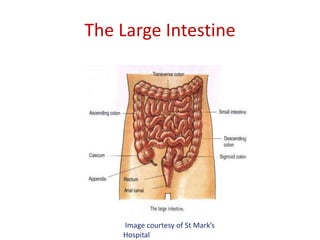
- 1. The Large Intestine Image courtesy of St Mark’s Hospital
- 2. Colon • Smooth muscle Inner circular (mixing) Outer longitudinal (peristaltic) • Haustra • Taenia Coli • Background motor activity (washing machine!) • 20-30 mins segmental propulsive contraction / massive migrating motor complexes (toothpaste!)
- 4. Nerve Supply to Colon • Extrinsic autonomic nerves (lumbar sympathetic and sacral parasympathetic innervation) • Local enteric neurones via submucosal and myenteric plexus within the layers of gut wall (capable of reflex activity without CNS activity -> peristalsis
- 5. Anal Sphincter Complex External Anal Sphincter (EAS) • Striated • 3 portions Deep- puborectalis/puboanalis Middle – coccyx posteriorly/ perineal body anteriorly Subcutaneous – no bony attachments • 15% resting pressure • Phasic • Pudendal innervation (sensory/motor/autonomic)
- 6. Anal Sphincter Complex contd. Internal Anal Sphincter (IAS) • Smooth muscle • 3cm long/2-3mm wide • Ends 10mm above anal verge • Long periods tonic activity • 85% resting pressure • No conscious control (autonomic)
- 8. © ACPWH Images courtesy of St Mark’s Hospital
- 9. A ‘normal’ ultrasound • Cone • Internal Anal Sphincter • External Anal Sphincter • Longitudinal layer • Subepithelial tissues VAGIN A
- 10. Sampling • Rectum fills • IAS relaxes exposing contents to rectal mucosa • Every 8-10 mins • 10s duration • EAS contract • RAIR (Recto-anal inhibitory reflex) • Critical volume -> 1st sensory perception (40- 50mls)
- 11. Sampling mechanism Image courtesy of St Mark’s
- 12. Resisting the urge/deferring • EAS squeeze • Generates enough pressure to prevent expulsion and return stool to rectum • Endurance required 10-15 seconds • Urge diminishes if deferment successful
- 13. Resisting the urge Image courtesy of St Mark’s
- 14. Levator Ani Pubo- visceral/ Pubo-coccygeus muscle • Pubo-vaginalis • Pubo-perinealis • Pubo-analis Puborectalis Ileococcygeus Coccygeus
- 15. Muscle fibre types • Type I Fibres approx 70% Slow oxidative - endurance • Type II Fibres approx 30% Fast glycolytic – speed and pressure • Variations from anterior to posterior – less type II posterior 1989 Gilpin et al.
- 16. Puborectalis, Puboanalis and the Anorectal Angle www.anatomy.tv
- 17. Puborectalis • Stabilises ano-rectum • Maintains the ano-rectal angle • Must be able to “pay out” /lengthen to allow for defaecation • Pubo-rectal continence reflex – involuntary contraction of pubo-rectalis during rectal filling
- 18. Puborectalis and the anorectal angle
- 20. Endopelvic Fascia Support • Level 1- Upper 1/3 vaginal wall to pelvic sidewalls • Level 2 – Middle 1/3 via pubocervical and endopelvic fascia • Level 3 – Lower 1/3 via perineal body, posterior EAS and transverse perineal muscle.
- 21. Defaecation Cycle • Rectum fills with faeces/stool • 1st sensory perception-> urge • Voluntary defaecation initiated • Sphincters relax • Pubo-rectalis lengthens and ano-rectal angle straightens • IAP raises (valsalva) • Gut contracts pressure funnels into pelvis • Faeces expelled into anal canal and out! • Closing anal reflex (final curtain down!) • Resting tone resumes.
