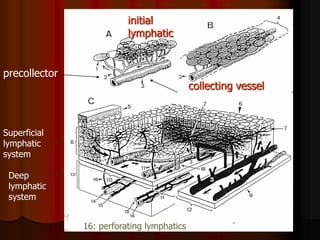
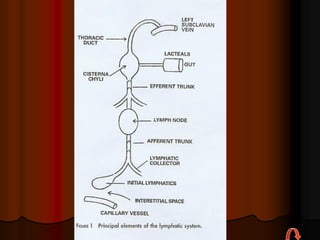
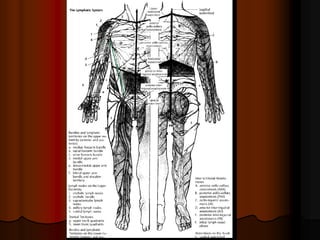
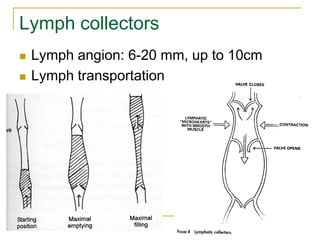
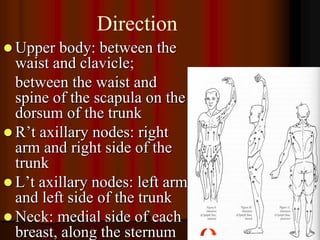
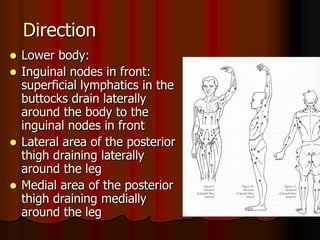
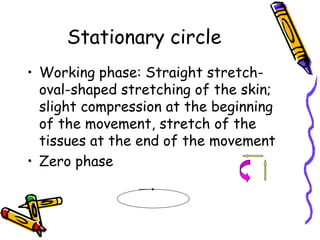
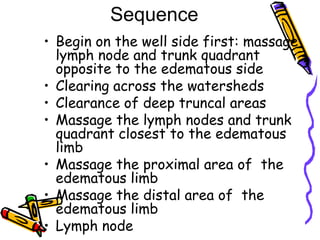
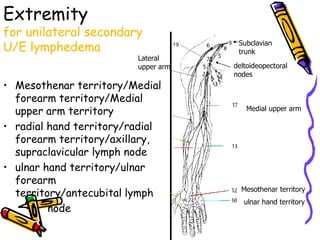
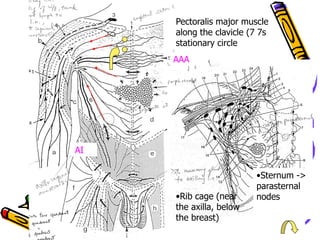
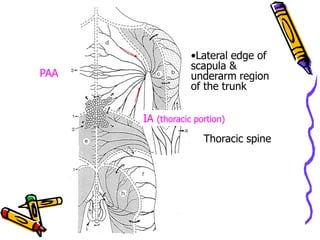
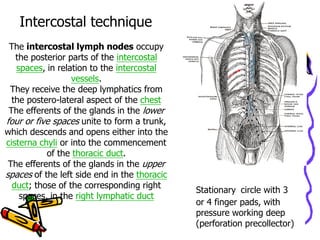
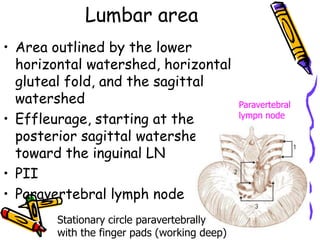
This document provides information on manual lymph drainage for treating lymphedema. It describes the lymphatic system and causes of lymphedema, stages of lymphedema, and complete decongestive physiotherapy. It details techniques for manual lymph drainage including direction of strokes, basic movements like pumps and circles, sequence of treatment, and truncal and extremity drainage patterns. The goal is to encourage lymph flow and reduce swelling through light skin stretching and movement toward lymph nodes.